Irritable bowel syndrome (IBS) is considered a functional gastrointestinal disorder. The Rome Foundation defines IBS as when a person has chronic abdominal pain at least one day per week in the last three months combined with at least two of the following: abdominal pain related to having a bowel movement; abdominal pain onset is associated with change in stool frequency; and/or abdominal pain onset is associated with change in stool form. The National Institutes of Health (NIH) reports that in 2004 there were 3 million ambulatory care visits with IBS noted as a diagnosis, and slightly more than half were first-listed diagnoses1. This disorder is estimated to affect 11-22% of the world’s population2. IBS is an incredibly common disorder and the demand for improved treatment options to treat this dysfunction is great. In order to understand how to treat IBS, we must first understand how cognitive and behavioral factors can impact gastrointestinal health.
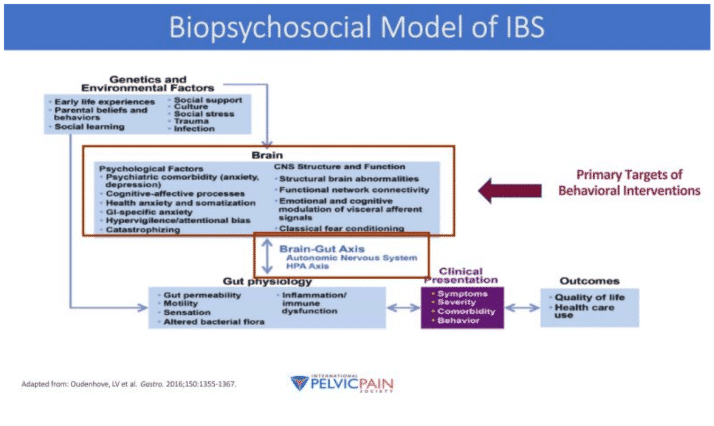
A key component affecting those who suffer from IBS is the Gut-Brain Axis (GBA). This refers to the bidirectional link between the central nervous system (CNS) and the autonomic nervous system (ANS). Specifically being effected is the enteric nervous system within the ANS, which consists of the network of neurons that governs a person’s gastrointestinal tract. Dysfunction here can manifest as symptoms including motility disturbance and visceral hypersensitivity, the most common manifestations being bowel dysfunction and pelvic and/or abdominal pain, respectively. Visceral hypersensitivity in particular can play a large role in IBS because these patients experience pain at lower thresholds than healthy controls. Unfortunately this can set off a cascading positive feedback loop of having some sort of stressful trigger which disturbs your gut and upsets the ANS, which causes visceral anxiety and increases GI symptoms, which then leads to further anxiety triggering more stress in the CNS, and the cycle continues. For more information on the link between you gut and your brain, check out our blog post called
The Brain Below: The Role Your Gut May Play in Pelvic Pain.
Most conventional approaches to treatment for IBS attempt to make changes at the level of the gut, for example, using pharmaceuticals and making diet alterations. These approaches are largely symptom based and are missing a key component in addressing this dysfunction by not including behavioral treatments. Because IBS is considered a functional GI disorder, as opposed to a structural disorder, emerging treatments have begun to include more practices that target this BGA to break the cycle of stress and symptoms by using behavioral therapies.
In October of 2019 at the annual meeting of the International Pelvic Pain Society, Sarah W. Kissinger, PhD, ABPP discussed using behavioral treatments for IBS. Dr. Kissinger discussed the efficacy of cognitive behavioral therapies (CBT) as treatment for IBS. The theory behind using CBT is to disrupt the positive feedback loop of stressors which affect the CNS proceeding to disrupt regular functioning in the ANS which will causing an escalation of GI symptoms. Cognitive behavioral therapy can give patients the tools necessary to modify physiological arousal and stress sensitivity, reduce catastrophic thoughts relating to symptoms, and address maladaptive coping behaviors. Patients who trialed CBT as treatment for IBS experienced positive changes in illness perceptions following intervention which mediated the treatment effect on improved IBS symptom severity and social adjustment six months later. 3
Treatment for IBS requires a multifaceted approach including behavioral therapies such as CBT and/or hypnosis. Traditional treatments such as pharmacological management and dietary changes are largely symptom based and do not do enough to affect the Brain-Gut Axis. Many patients will benefit from the addition of these alternative treatment methods to best reduce a patient’s symptoms and improve quality of life.
Additional information on IBS and hypnosis, as well as resources for how to find providers who specialize in this can be found at ibshypnosis.com. To learn more about PHRC and get in touch with a provider who can help you tackle IBS check out our website.
References:
- Everhart JE. Functional Intestinal Disorders. Everhart JE, editor. The burden of digestive diseases in the United States. US Department of Health and Human Services, Public Health Service, National Institutes of Health, National Institute of Diabetes and Digestive and Kidney Diseases. Washington, DC: US Government Printing Office, 2008; NIH Publication No. 09-6443 [pp. 77-87].
- Aziz et al, AM J Gastroenterol. 2018;113:86-96:Russo et al., J Clin Gastroenterol 1999; 29:339-43; National Institutes of Health. The burden of digestive diseases in the United States, 09-6443; January 2010.
- Chilcot J, Moss-Morris R. Changes in illness-related cognitions rather than distress mediate improvements in irritable bowel syndrome (IBS) symptoms and disability following a brief cognitive behavioural therapy intervention. Health Psychology Section, Psychology Department, Institute of Psychiatry, King’s College London, UK
- Palsson, O.S., Turner, M.J., Johnson, D.A. et al. Dig Dis Sci (2002) 47: 2605. https://doi.org/10.1023/A:1020545017390
FAQ
What are pelvic floor muscles?
The pelvic floor muscles are a group of muscles that run from the coccyx to the pubic bone. They are part of the core, helping to support our entire body as well as providing support for the bowel, bladder and uterus. These muscles help us maintain bowel and bladder control and are involved in sexual pleasure and orgasm. The technical name of the pelvic floor muscles is the Levator Ani muscle group. The pudendal nerve, the levator ani nerve, and branches from the S2 – S4 nerve roots innervate the pelvic floor muscles. They are under voluntary and autonomic control, which is a unique feature only they possess compared to other muscle groups.
What is pelvic floor physical and occupational therapy?
Pelvic floor physical and occupational therapy is a specialized area of physical and occupational therapy. Currently, physical and occupational therapistss need advanced post-graduate education to be able to help people with pelvic floor dysfunction because pelvic floor disorders are not yet being taught in standard physical and occupational therapy curricula. The Pelvic Health and Rehabilitation Center provides extensive training for our staff because we recognize the limitations of physical and occupational therapy education in this unique area.
What happens at pelvic floor therapy?
During an evaluation for pelvic floor dysfunction the physical and occupational therapists will take a detailed history. Following the history the physical and occupational therapists will leave the room to allow the patient to change and drape themselves. The physical and occupational therapists will return to the room and using gloved hands will perform an external and internal manual assessment of the pelvic floor and girdle muscles. The physical and occupational therapists will once again leave the room and allow the patient to dress. Following the manual examination there may also be an examination of strength, motor control, and overall biomechanics and neuromuscular control. The physical and occupational therapists will then communicate the findings to the patient and together with their patient they establish an assessment, short term and long term goals and a treatment plan. Typically people with pelvic floor dysfunction are seen one time per week for one hour for varying amounts of time based on the severity and chronicity of the disease. A home exercise program will be established and the physical and occupational therapists will help coordinate other providers on the treatment team. Typically patients are seen for 3 months to a year.
What is pudendal neuralgia and how is it treated?
Pudendal Neuralgia is a clinical diagnosis that means pain in the sensory distribution of the pudendal nerve. The pudendal nerve is a mixed nerve that exits the S2 – S4 sacral nerve roots, we have a right and left pudendal nerve and each side has three main trunks: the dorsal branch, the perineal branch, and the inferior rectal branch. The branches supply sensation to the clitoris/penis, labia/scrotum, perineum, anus, the distal ⅓ of the urethra and rectum, and the vulva and vestibule. The nerve branches also control the pelvic floor muscles. The pudendal nerve follows a tortuous path through the pelvic floor and girdle, leaving it vulnerable to compression and tension injuries at various points along its path.
Pudendal Neuralgia occurs when the nerve is unable to slide, glide and move normally and as a result, people experience pain in some or all of the above-mentioned areas. Pelvic floor physical and occupational therapy plays a crucial role in identifying the mechanical impairments that are affecting the nerve. The physical and occupational therapy treatment plan is designed to restore normal neural function. Patients with pudendal neuralgia require pelvic floor physical and occupational therapy and may also benefit from medical management that includes pharmaceuticals and procedures such as pudendal nerve blocks or botox injections.
What is interstitial cystitis and how is it treated?
Interstitial Cystitis is a clinical diagnosis characterized by irritative bladder symptoms such as urinary urgency, frequency, and hesitancy in the absence of infection. Research has shown the majority of patients who meet the clinical definition have pelvic floor dysfunction and myalgia. Therefore, the American Urologic Association recommends pelvic floor physical and occupational therapy as first-line treatment for Interstitial Cystitis. Patients will benefit from pelvic floor physical and occupational therapy and may also benefit from pharmacologic management or medical procedures such as bladder instillations.
Who is the Pelvic Health and Rehabilitation Team?
The Pelvic Health and Rehabilitation Center was founded by Elizabeth Akincilar and Stephanie Prendergast in 2006, they have been treating people with pelvic floor disorders since 2001. They were trained and mentored by a medical doctor and quickly became experts in treating pelvic floor disorders. They began creating courses and sharing their knowledge around the world. They expanded to 11 locations in the United States and developed a residency style training program for their employees with ongoing weekly mentoring. The physical and occupational therapistss who work at PHRC have undergone more training than the majority of pelvic floor physical and occupational therapistss and as a result offer efficient and high quality care.
How many years of experience do we have?
Stephanie and Liz have 24 years of experience and help each and every team member become an expert in the field through their training and mentoring program.
Why PHRC versus anyone else?
PHRC is unique because of the specific focus on pelvic floor disorders and the leadership at our company. We are constantly lecturing, teaching, and staying ahead of the curve with our connections to medical experts and emerging experts. As a result, we are able to efficiently and effectively help our patients restore their pelvic health.
Do we treat men for pelvic floor therapy?
The Pelvic Health and Rehabilitation Center is unique in that the Cofounders have always treated people of all genders and therefore have trained the team members and staff the same way. Many pelvic floor physical and occupational therapistss focus solely on people with vulvas, this is not the case here.
Do I need pelvic floor therapy forever?
The majority of people with pelvic floor dysfunction will undergo pelvic floor physical and occupational therapy for a set amount of time based on their goals. Every 6 -8 weeks goals will be re-established based on the physical improvements and remaining physical impairments. Most patients will achieve their goals in 3 – 6 months. If there are complicating medical or untreated comorbidities some patients will be in therapy longer.



Comments
https://waterfallmagazine.com
Superb blog! Do you have any tips and hints for aspiring writers?
I’m hoping to start my own website soon but
I’m a little lost on everything. Would you suggest starting
with a free platform like WordPress or go for a paid option? There are so many choices out there
that I’m completely confused .. Any tips? Kudos!
Thank you! We use wordpress, and it works for us. It all depends on what you are trying to put out or accomplish with your website. Best of luck to you!