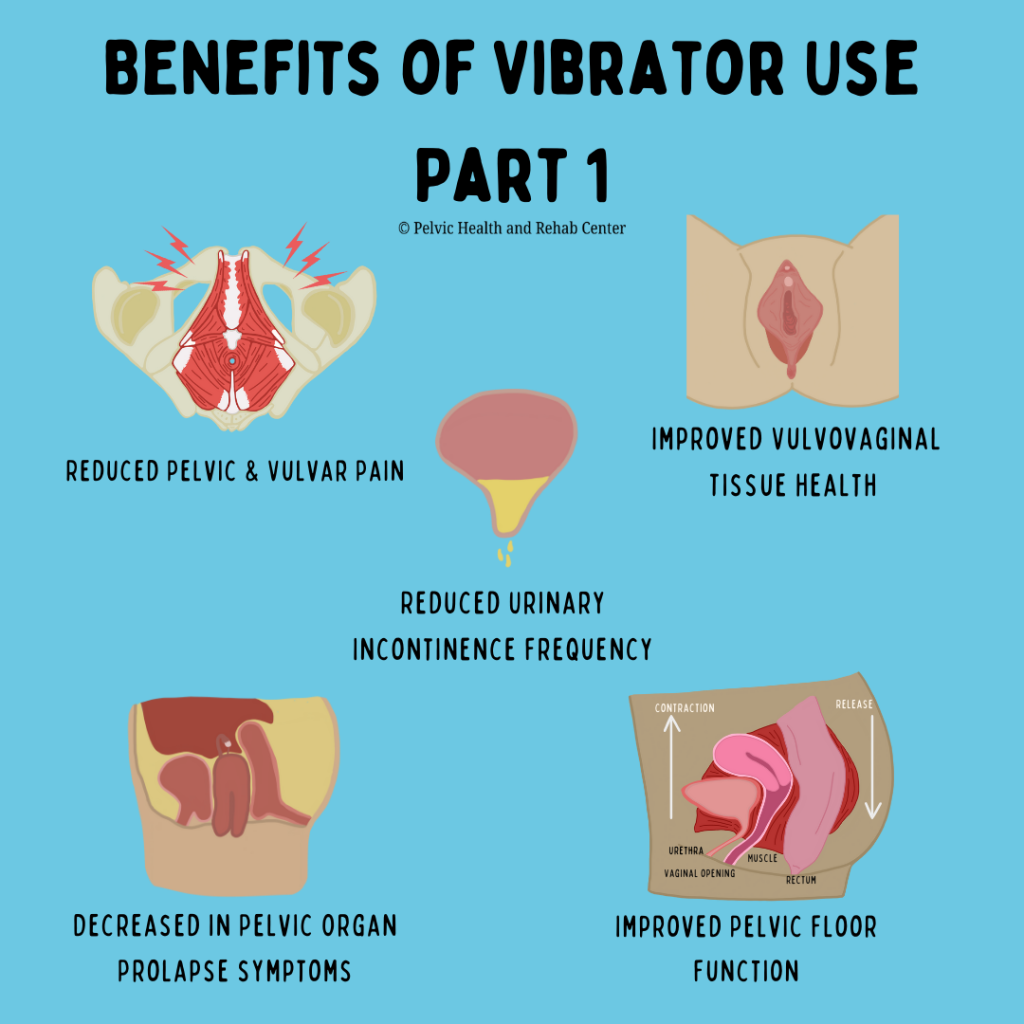
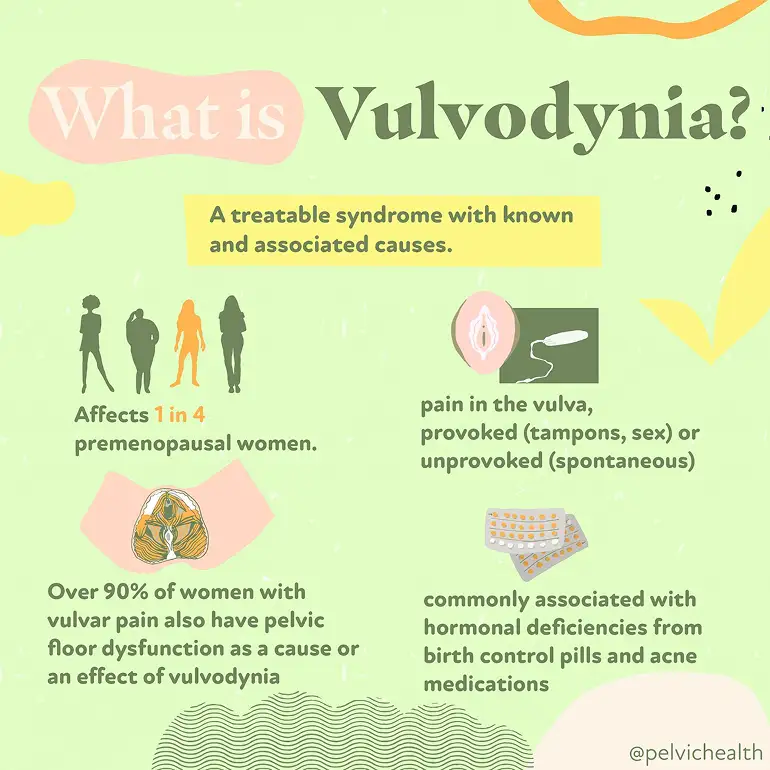
Don’t overlook the true impact of menopause! Despite affecting half the population, there’s a widespread lack of knowledge about menopause and effective treatments. Countless people are needlessly suffering. Perimenopause, the lead-up to menopause, typically begins in a person’s 40s, with most women entering menopause in their early 50s. Alongside the well-known symptoms of menopause, individuals will also experience subtler genitourinary symptoms that worsen over time if left untreated. These symptoms include painful sex, urinary urgency, frequency, leakage, burning, recurrent infections, and vaginal dryness, collectively known as the Genitourinary Syndrome of Menopause (GSM). It’s important to note that these symptoms overlap with pelvic floor dysfunction, a condition that nearly 50% of women experience by their 50s.
For menopause symptoms, systemic hormonal therapy is commonly used. However, this may not be enough for those experiencing GSM symptoms. To address this, the North American Menopause Society suggests using vaginal estrogen in menopausal women to alleviate GSM symptoms.
Don’t overlook the true impact of menopause! Despite affecting half the population, there’s a widespread lack of knowledge about menopause and effective treatments. Countless people are needlessly suffering. Perimenopause, the lead-up to menopause, typically begins in a person’s 40s, with most women entering menopause in their early 50s. Alongside the well-known symptoms of menopause, individuals will also experience subtler genitourinary symptoms that worsen over time if left untreated. These symptoms include painful sex, urinary urgency, frequency, leakage, burning, recurrent infections, and vaginal dryness, collectively known as the Genitourinary Syndrome of Menopause (GSM). It’s important to note that these symptoms overlap with pelvic floor dysfunction, a condition that nearly 50% of women experience by their 50s.
For menopause symptoms, systemic hormonal therapy is commonly used. However, this may not be enough for those experiencing GSM symptoms. To address this, the North American Menopause Society suggests using vaginal estrogen in menopausal women to alleviate GSM symptoms.
Differential Diagnosis:
GSM or Pelvic Floor Dysfunction
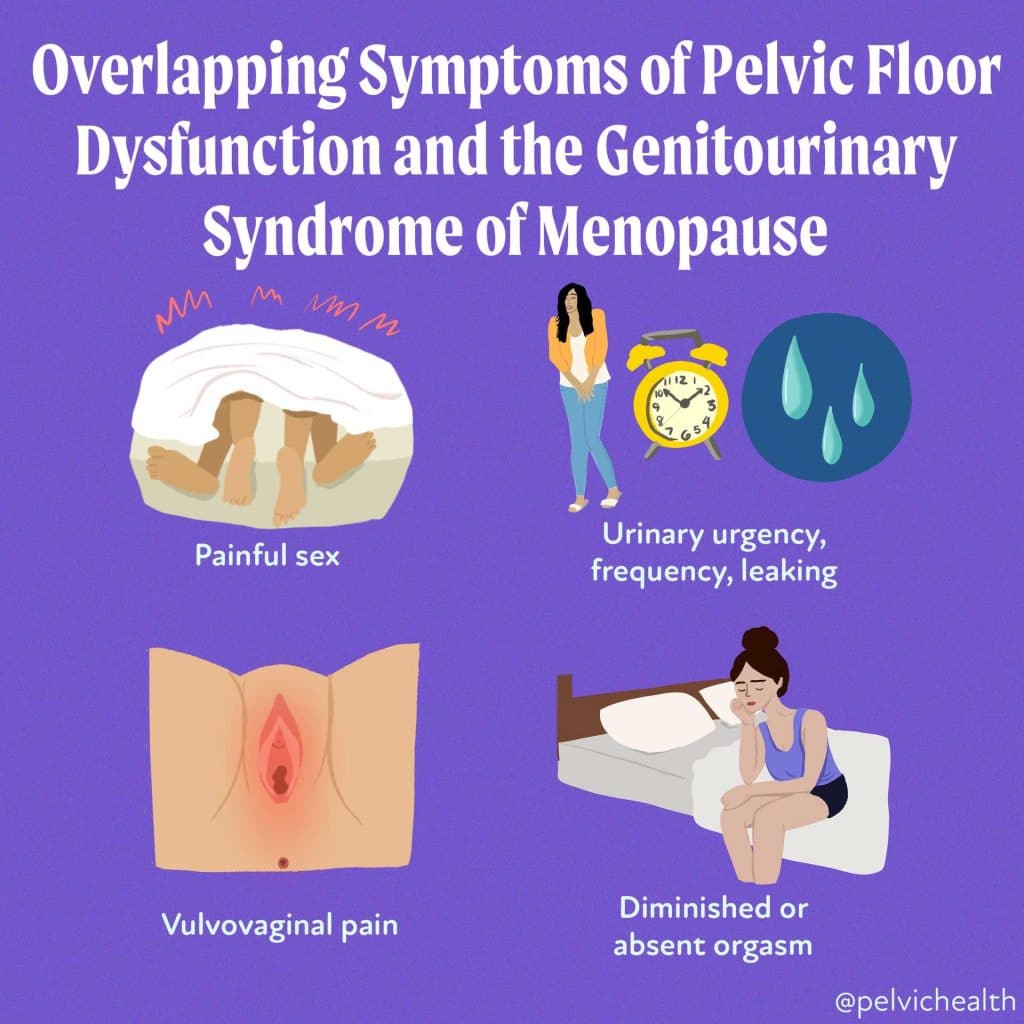
Pelvic floor dysfunction and genitourinary syndrome of menopause (GSM) can cause the following symptoms:
- Frequent and urgent need to urinate, along with a burning sensation and waking up frequently at night to use the bathroom.
- Experiencing pressure in the bladder or pelvic area.
- Pain or discomfort during sexual intercourse.
- Difficulty achieving orgasm or a decrease in sexual pleasure.
- Trouble with bowel movements and feeling unable to fully empty the bowels.
- Pain, burning, or discomfort in the vulva and vagina.
- Pain while sitting.
A knowledgeable healthcare provider, such as a pelvic floor physical and occupational therapists or medical doctor at Menopause Pelvic Floor Physical and Occupational Therapy in San Francisco, can conduct various examinations to assess vaginal and pelvic health. These include visual examinations, q-tip tests to identify pain areas, and manual examinations to detect issues like pelvic floor dysfunction, hormonal deficiencies, and pelvic organ prolapse. It’s important to note that all women may experience genitourinary syndrome of menopause (GSM) if not properly managed by medical professionals. Interestingly, many people aren’t aware that menopausal women can benefit from pelvic floor physical and occupational therapy, which can address musculoskeletal factors that contribute to discomfort. The combination of pelvic floor physical and occupational therapy and medical management at Menopause Pelvic Floor Physical and Occupational Therapy in San Francisco, is crucial in restoring enjoyable sexual experiences and resolving urinary and bowel concerns.
FACTS
From: https://www.letstalkmenopause.org/further-reading
- Every day, 6000 women experience menopause.
- In the US, there are currently 50 million women going through menopause.
- A staggering 84% of women face genital, sexual, and urinary discomfort during menopause, and only a small number seek professional help.
- Surprisingly, 80% of OBGYN residents admit to lacking the knowledge to effectively address menopause.
- 90% of postmenopausal women have GSM, but only ⅓ of them actually report experiencing symptoms.
- Common barriers to treatment include women having to initiate the conversation, believing that symptoms are a normal part of aging, and failing to connect their symptoms to menopause.
- Surprisingly, only 13% of healthcare providers ask their patients about menopause symptoms.
- Even after diagnosis, the majority of women with GSM don’t receive treatment, despite studies showing it can negatively affect their quality of life. This is due to hesitation from providers, as well as concerns from patients about the safety of vaginal therapies.
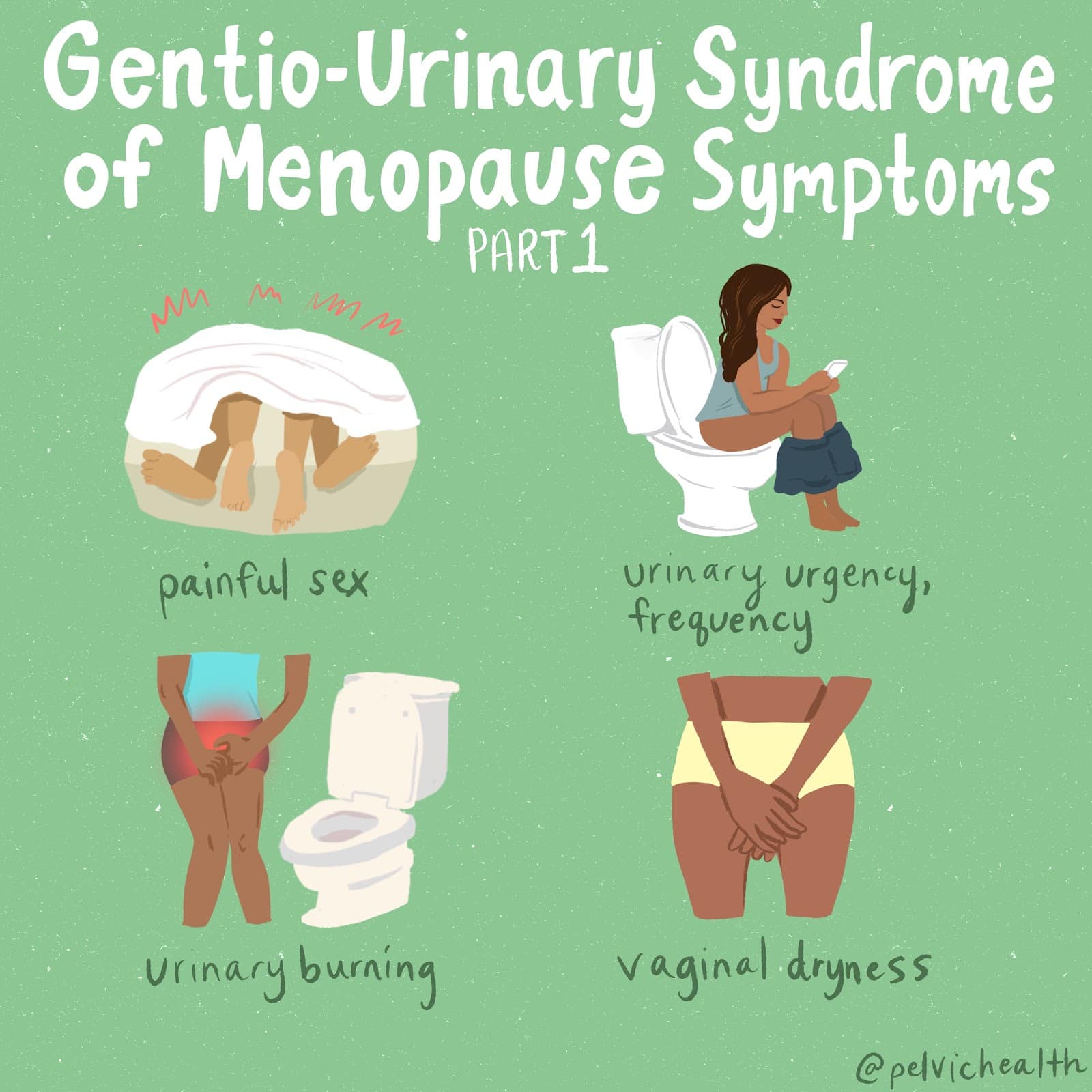
Hormone insufficiency can cause itching in the areas between the labia and vagina. It’s important to note that there are other skin conditions, such as Lichen Sclerosus and yeast infections, that should also be taken into account.
Menopausal women are at risk of recurring vaginal and urinary tract infections due to three main factors:
- Changes in pH and tissue
- Incomplete bladder emptying
- Pelvic organ prolapse affecting urinary function
Recurrent infections can cause pelvic floor dysfunction, a common issue. It is important to address these infections promptly to prevent further pain and dysfunction once the infection is treated. If left untreated without hormone therapy, infections can continue to occur and result in serious consequences. Women may experience unprovoked pain, difficulty with sex, and undetected UTIs can lead to kidney problems and other health issues. Taking action is crucial to minimize the negative effects of these infections.
Consulting a menopause expert at Menopause Pelvic Floor Physical and Occupational Therapy in San Francisco, is vital for monitoring, preventing, and treating these significant and treatable issues. Let’s remove the stigma surrounding GSM and openly discuss its effects; there’s no need for embarrassment. With proper care, individuals with vulvas can lead fulfilling lives. Pelvic floor physical and occupational therapy and medical management complement each other effectively.
How We Can Help You

Get evaluated by a therapist for pelvic floor therapy at Menopause Pelvic Floor Physical and Occupational Therapy in San Francisco, if you’re having issues with your sexual function. They will assess your pelvic floor and determine the contributing factors. The therapist will discuss your medical history, previous treatments, and their effectiveness. The evaluation will include an examination of your nerves, muscles, joints, tissues, and movement patterns. Afterwards, the therapist will review the results with you and establish short-term and long-term therapy goals. Physical therapy treatments are typically done once or twice a week for 12 weeks. Your therapist will coordinate your recovery with other professionals on your treatment team. They will provide you with exercises to do at home and in-person sessions. Our goal is to help you improve and live your best life.
Check out our IC/PBS Resource List for more information about IC/PBS.

How We Can Help You
Get evaluated by a therapist for pelvic floor therapy at Menopause Pelvic Floor Physical and Occupational Therapy in San Francisco, if you’re having issues with your sexual function. They will assess your pelvic floor and determine the contributing factors. The therapist will discuss your medical history, previous treatments, and their effectiveness. The evaluation will include an examination of your nerves, muscles, joints, tissues, and movement patterns. Afterwards, the therapist will review the results with you and establish short-term and long-term therapy goals. Physical therapy treatments are typically done once or twice a week for 12 weeks. Your therapist will coordinate your recovery with other professionals on your treatment team. They will provide you with exercises to do at home and in-person sessions. Our goal is to help you improve and live your best life.
Check out our IC/PBS Resource List for more information about IC/PBS.