If you are searching from Beverly Hills and experiencing persistent testicular pain you are not alone. Many men mistakenly believe the cause is always infection, but pain in this region can stem from other sources. Pelvic floor dysfunction, nerve compression in the lower spine, or restricted pelvic blood flow are often overlooked contributors to chronic discomfort.
Because the symptoms often overlap with those of prostatitis, many individuals are misdiagnosed and prescribed antibiotics that do not provide meaningful results. When medication fails to make a difference, it usually indicates that the issue is rooted in muscle tension or nerve sensitivity rather than infection.
Men living in or near Beverly Hills can find lasting relief through pelvic floor physical and occupational therapy. These evidence-based treatments help release tight muscles, restore movement coordination, and improve nerve function. This non-invasive path promotes healing from the inside out, helping men return to normal activities without ongoing pain.
What are the Causes of Testicular Pain?
Testicular pain may arise from several interconnected physiological systems, most notably the lumbar spine, vascular structures, and pelvic floor muscles.
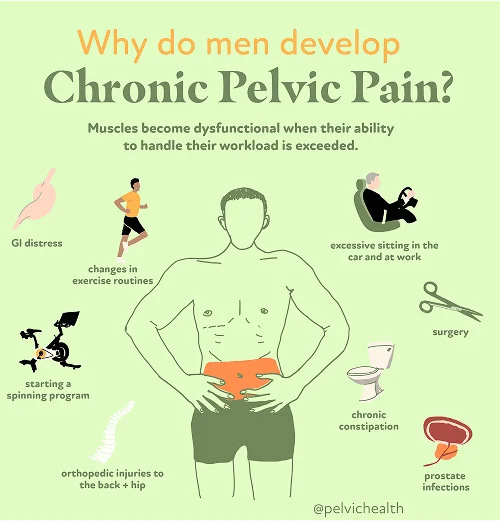
- Lumbar pathology: Since testicular nerves emerge from the lower spinal segments, any mechanical or inflammatory disorder in the lumbar region such as arthritis, a bulging disc, or nerve impingement can send pain signals downward, producing discomfort perceived in the testicle.
- Vascular pathology: Impaired venous flow in the pelvic and testicular regions can lead to varicoceles, torsion, or venous congestion, each of which generates dull, heavy, or sometimes sharp pain sensations.
- Pelvic floor pathology: The pelvic floor is composed of supportive muscles that maintain proper alignment and stability for pelvic organs. When these muscles tighten excessively or develop spasms, they can irritate nerve pathways, creating referred pain that mimics a testicular origin.
Additional causes of testicular pain can include:
- Surgical trauma (vasectomy, benign prostatic hyperplasia (BPH) interventions, prostatectomy)
- Biomechanical or structural dysfunction (hip dysfunction, piriformis syndrome, scoliosis, leg length discrepancy)
- Excessive exercise or changes to exercise routine
- Excessive sitting
- Chronic constipation and straining
- Jelqing and/or attempts at gential enhancement or foreskin regeneration
- In rare cases, bladder, prostate, or sexually transmitted infections after successful resolution of infection
- The majority of men with pelvic pain (including testicular pain), with or without urinary or bowel complaints, have pelvic floor dysfunction
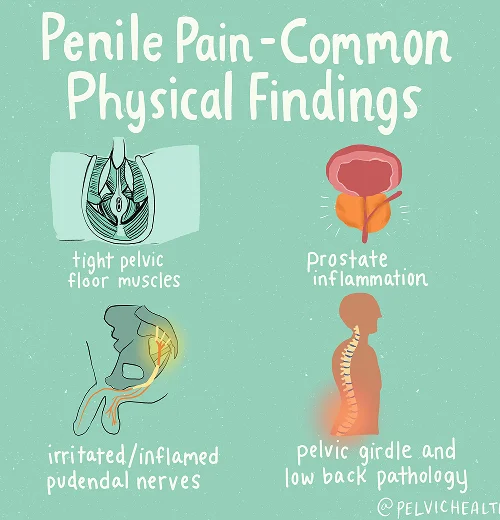

Symptoms of Testicular Pain
- Men experiencing testicular pain often describe it as a persistent burning, stabbing, or dull ache that disrupts normal comfort.
- This pain can travel beyond the testicles themselves, reaching the penis, scrotum, perineum, or the region surrounding the anus.
Many individuals also encounter a variety of additional issues alongside testicular discomfort:
- Pelvic aching tends to worsen when sitting for long durations, following physical exertion, or while wearing snug trousers or athletic wear.
- Problems with urination such as increased frequency, an urgent need to void, or a slower urinary flow are quite typical.
- Pain or discomfort during ejaculation is another symptom, with men often noting sensations extending into the scrotum or perineal area.
- In some cases, there may also be reduced erectile function or a noticeable decline in ejaculation power.
- Digestive irregularities, including feelings of bloating, constipation, or general abdominal unease, frequently accompany these symptoms.
- These gastrointestinal concerns can become more intense after exercise or sexual activity or emerge unexpectedly without reason.
- The severity of all symptoms may fluctuate over time, alternating between mild relief and heightened sensitivity.
Associated Diagnoses
Pain in the testicular and pelvic areas can result from multiple sources acting together, particularly dysfunctions within the lumbar spine, vascular structures, and pelvic floor. Lumbar issues usually appear as lumbar radiculopathy or nerve-related pain associated with spinal degeneration, disc problems, or lower back compression. Vascular conditions such as varicocele, testicular torsion, and pelvic venous congestion can disrupt circulation and cause dull or throbbing pain. The pelvic floor is intricately linked to these conditions and is often involved in Chronic Pelvic Pain Syndrome (CPPS), pudendal neuralgia, painful bladder syndrome, and hard flaccid syndrome. In numerous patients, weakness or overactivity in this area either triggers or intensifies pain resulting from other structural or vascular dysfunctions.
Diagnostic Challenges
Many men suffer from testicular pain, yet in a large number of cases, this discomfort is incorrectly attributed to prostatitis. Physicians sometimes prescribe antibiotics even though laboratory testing shows no bacterial infection. Clinical studies repeatedly demonstrate that roughly 90 percent of men who experience chronic pelvic or genital pain do not have a bacterial infection in the prostate gland.
Most of these patients are found to fall under the National Institutes of Health’s Category IIIa or IIIb, both of which form part of the broader condition identified as Chronic Pelvic Pain Syndrome (CPPS). Furthermore, nerve compression or irritation in the lumbar spine and disturbances in pelvic circulation can create symptoms identical to those of pelvic floor dysfunction, complicating the diagnostic process and prolonging treatment.
As outlined by the National Institutes of Health, prostatitis conditions are organized into the following categories:
- Category I: Acute bacterial prostatitis is defined by sharp pelvic pain, fever, and urinary infection caused by bacteria entering and inflaming the prostate.
- Category II: Chronic bacterial prostatitis involves continuous infection of the prostate with bacterial strains that produce recurring urinary issues.
- Category IIIa: Inflammatory chronic pelvic pain syndrome includes immune response activity identified through white blood cells in prostate samples.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome shows no white blood cells, indicating discomfort without inflammation.
- Category IV: Asymptomatic inflammatory prostatitis shows inflammation in diagnostic tests without any reported symptoms.

As outlined by the National Institutes of Health, prostatitis conditions are organized into the following categories:
- Category I: Acute bacterial prostatitis is defined by sharp pelvic pain, fever, and urinary infection caused by bacteria entering and inflaming the prostate.
- Category II: Chronic bacterial prostatitis involves continuous infection of the prostate with bacterial strains that produce recurring urinary issues.
- Category IIIa: Inflammatory chronic pelvic pain syndrome includes immune response activity identified through white blood cells in prostate samples.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome shows no white blood cells, indicating discomfort without inflammation.
- Category IV: Asymptomatic inflammatory prostatitis shows inflammation in diagnostic tests without any reported symptoms.

Treatment for Testicular Pain
Depending on what contributes to your pain, whether it is due to chronic muscle tension, irritated nerves within the lumbar region, or restricted blood movement in the pelvic area, your therapist may design a program that blends several therapeutic interventions to help bring your pelvic floor back into balance. This approach allows the body to heal naturally and restore proper coordination of the surrounding muscles and tissues.
- Pelvic floor physical and occupational therapy for pelvic floor dysfunction: This therapy centers on teaching the pelvic floor muscles how to relax, coordinate, and function properly again. Through manual techniques and guided exercises, it helps calm irritated pelvic nerves, reduce tightness, and restore healthy muscle tone, leading to gradual but lasting pain relief and better comfort in everyday movements.
- Spine and back treatment: When your symptoms originate in the lumbar spine, the treatment approach may focus on gentle spine mobilization, targeted strengthening, and postural training. In more complex cases, guided injections may be recommended to ease inflammation and relieve nerve compression that contributes to pelvic pain.
- Vascular-related treatment: For individuals whose discomfort is related to reduced blood flow, therapy may use posture correction, breathing retraining, and relaxation techniques to stimulate better circulation. This improves oxygen delivery to the tissues and helps decrease the pressure on pelvic veins that may be congested.
- Addressing biomechanical issues: If limited movement or alignment problems in the hips are adding strain to the pelvic muscles, your therapist will use stretching, strengthening, and balance exercises to restore proper mobility and mechanical support. The goal is to reduce stress on sensitive pelvic tissues.
- Lifestyle adjustments: Modifying daily habits is also key. Patients are often guided to manage constipation, avoid long sitting sessions, and gradually resume light physical activity to help their body heal safely and prevent future tension from developing in the pelvic region.
How We Can Help You with Testicular Pain
If you are from Beverly Hills and have been coping with long-lasting testicular pain, professional support from a pelvic floor physical and occupational therapist could make a significant difference. At PHRC, we start with a thorough consultation that reviews your medical background, past treatments, and any symptoms that have persisted. Understanding your full history helps us uncover the true source of your discomfort and determine which next steps are most appropriate.
We recognize that many men searching for help in Beverly Hills often feel discouraged after trying numerous treatments without success. Our experienced therapists prioritize compassion and education, ensuring that you leave your evaluation with a plan that is both structured and easy to follow.
During the assessment, your therapist will evaluate your pelvic muscles, surrounding tissues, and nerve function, while observing your movement patterns and alignment. After this detailed review, you will discuss the results together, gain insight into how your condition developed, and set realistic goals for progress.

How We Can Help You with Testicular Pain
If you are from Beverly Hills and have been coping with long-lasting testicular pain, professional support from a pelvic floor physical and occupational therapist could make a significant difference. At PHRC, we start with a thorough consultation that reviews your medical background, past treatments, and any symptoms that have persisted. Understanding your full history helps us uncover the true source of your discomfort and determine which next steps are most appropriate.
We recognize that many men searching for help in Beverly Hills often feel discouraged after trying numerous treatments without success. Our experienced therapists prioritize compassion and education, ensuring that you leave your evaluation with a plan that is both structured and easy to follow.
During the assessment, your therapist will evaluate your pelvic muscles, surrounding tissues, and nerve function, while observing your movement patterns and alignment. After this detailed review, you will discuss the results together, gain insight into how your condition developed, and set realistic goals for progress.

Treatment sessions are usually scheduled once or twice a week for roughly three months, with targeted home exercises to continue your recovery between visits. Throughout your care, your PHRC therapist collaborates with your healthcare providers to ensure a coordinated and effective approach. Our commitment is to help you achieve lasting comfort and renewed confidence in your health.
