Are you experiencing unexplained testicular pain in Burbank? It’s more common than most men realise, and it can often stem from causes that have nothing to do with infection. Testicular pain may be linked to pelvic floor dysfunction, nerve irritation from the lower back, or issues affecting blood circulation in the pelvic area.
Sadly, many men are misdiagnosed with prostatitis when they present with these symptoms, leading to the unnecessary use of antibiotics that do not resolve the issue. This approach often overlooks the true musculoskeletal or nerve-related origin of the pain.
Pelvic floor physical and occupational therapy in Burbank provides a more accurate and effective solution. By addressing muscle imbalances, improving pelvic floor and core coordination, and reducing tension in the surrounding areas, therapy helps alleviate pain at its source. Over time, men who undergo this type of treatment often find lasting relief and improved pelvic health.
What are the Causes of Testicular Pain?
There are several potential causes of testicular pain, many of which are tied to lumbar pathology, vascular pathology, and pelvic floor pathology.
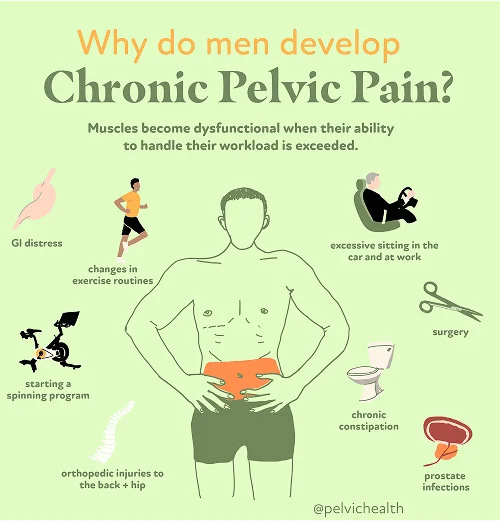
- Lumbar pathology: The nerves that control sensation in the testicles begin in the lumbar spine. When a disc slips, arthritis progresses, or inflammation affects a lumbar nerve, the discomfort can radiate downward and feel localized in the testicle, though the true source of the pain is the lower back.
- Vascular pathology: Circulatory conditions such as enlarged veins called varicoceles, twisting of the testicular blood supply known as torsion, or venous congestion can lead to pressure, aching, or intermittent sharp pain in one or both testicles.
- Pelvic floor pathology: Acting as a muscular sling beneath the pelvis, the pelvic floor can become overly tight, weak, or experience spasms, which may irritate surrounding nerves and result in pain that feels internal but actually originates from these muscles.
Additional causes of testicular pain can include:
- Surgical trauma (vasectomy, benign prostatic hyperplasia (BPH) interventions, prostatectomy)
- Biomechanical or structural dysfunction (hip dysfunction, piriformis syndrome, scoliosis, leg length discrepancy)
- Excessive exercise or changes to exercise routine
- Excessive sitting
- Chronic constipation and straining
- Jelqing and/or attempts at gential enhancement or foreskin regeneration
- In rare cases, bladder, prostate, or sexually transmitted infections after successful resolution of infection
- The majority of men with pelvic pain (including testicular pain), with or without urinary or bowel complaints, have pelvic floor dysfunction
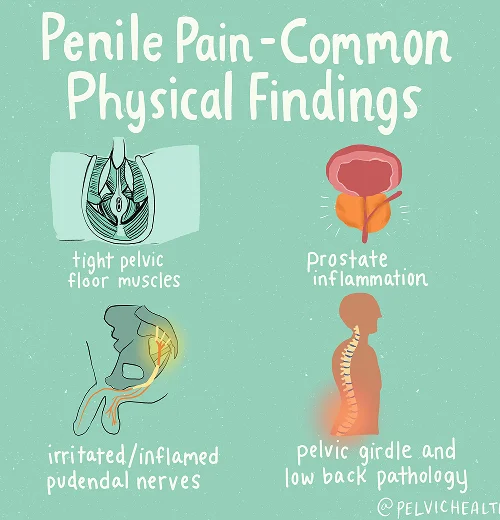

Symptoms of Testicular Pain
- A burning, heavy, or aching feeling within the testicles
- These sensations can spread to the penis, scrotum, perineal region, or anal area
Aside from testicular pain itself, many men experience a mix of additional symptoms:
- Persistent pelvic pain that becomes more pronounced with sitting, certain exercises, or when wearing constrictive clothing
- Urinary concerns such as urgency, frequency, hesitancy, or a slow and weakened urine stream often accompany pelvic pain
- Men frequently describe aching or discomfort in the penis, scrotum, or perineum when ejaculating
- There may also be signs of erectile dysfunction or a noticeable reduction in ejaculatory pressure
- Digestive issues including constipation, abdominal bloating, or a general sense of gastrointestinal discomfort are common
- These gastrointestinal issues might worsen after ejaculation, physical exertion, or appear randomly without a clear cause
- The intensity of symptoms can vary, with some men experiencing brief flare-ups while others have constant discomfort
Associated Diagnoses
The lumbar spine, vascular system, and pelvic floor each play significant roles in contributing to testicular and pelvic discomfort, often creating a complex web of overlapping conditions. Lumbar pathology commonly appears as lumbar radiculopathy or referred pain caused by disc protrusion, degenerative changes, or arthritis of the lower spine. Vascular pathology is represented by conditions such as varicocele, testicular torsion, or pelvic venous congestion, all of which interfere with normal circulation and provoke pain responses. Pelvic floor pathology, meanwhile, is frequently connected with Chronic Pelvic Pain Syndrome (CPPS), pudendal neuralgia, hard flaccid syndrome, and painful bladder syndrome. Pelvic floor dysfunction often emerges as the underlying element, either being the primary source of discomfort or amplifying pain that stems from spinal or vascular abnormalities.
Diagnostic Challenges
Testicular pain in men is often misinterpreted as prostatitis, leading to unnecessary prescriptions for antibiotics even when no infection exists. Numerous medical studies have indicated that more than 90 percent of men presenting with pelvic or genitourinary pain do not actually have a bacterial prostate infection.
In most instances, these men fall within the National Institutes of Health categories IIIa and IIIb, which make up Chronic Pelvic Pain Syndrome (CPPS). Complicating diagnosis further, pain originating from lumbar nerve irritation or vascular congestion can produce symptoms nearly identical to those of pelvic floor dysfunction. This overlap makes it challenging to pinpoint the actual source of pain and can lead to prolonged misdiagnosis before effective treatment is provided.
The National Institutes of Health provides the following classifications for prostatitis syndromes:
- Category I: Acute bacterial prostatitis, typically associated with intense discomfort, systemic infection, and an acute bacterial urinary tract infection.
- Category II: Chronic bacterial prostatitis, caused by a long-term bacterial infection of the prostate, sometimes accompanied by repeated urinary tract infections from the same organism.
- Category IIIa: Inflammatory chronic pelvic pain syndrome, marked by the presence of white blood cells in semen, expressed prostatic fluid, or the third urine specimen.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome, where no white blood cells are found in the same samples.
- Category IV: Asymptomatic inflammatory prostatitis, identified by inflammation within the prostate without any noticeable urinary or pelvic symptoms.

The National Institutes of Health provides the following classifications for prostatitis syndromes:
- Category I: Acute bacterial prostatitis, typically associated with intense discomfort, systemic infection, and an acute bacterial urinary tract infection.
- Category II: Chronic bacterial prostatitis, caused by a long-term bacterial infection of the prostate, sometimes accompanied by repeated urinary tract infections from the same organism.
- Category IIIa: Inflammatory chronic pelvic pain syndrome, marked by the presence of white blood cells in semen, expressed prostatic fluid, or the third urine specimen.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome, where no white blood cells are found in the same samples.
- Category IV: Asymptomatic inflammatory prostatitis, identified by inflammation within the prostate without any noticeable urinary or pelvic symptoms.

Treatment for Testicular Pain
Treatment for testicular or pelvic pain varies depending on what is causing your symptoms. Contributing factors may include pelvic floor muscle tension, irritation of the nerves, or circulation challenges that restrict proper blood flow to the area.
- Pelvic floor physical and occupational therapy for pelvic floor dysfunction: This therapy helps relax overly active muscles, retrain them for balanced function, and reduce nerve sensitivity in the pelvic region, which can significantly ease discomfort.
- Spine and back treatment: If nerve involvement in the lower back is found to be part of the problem, your plan may include targeted physical and occupational therapy, guided postural work, and possibly medical procedures like injections to calm inflamed nerves.
- Vascular-related treatment: For men experiencing vascular congestion, therapy can support improved blood circulation by addressing muscle guarding and teaching techniques that promote better posture and diaphragmatic breathing.
- Addressing biomechanical issues: When poor hip alignment or mobility issues contribute to pain, therapeutic exercise and joint mobilisation can restore healthy movement and reduce stress on the pelvic structures.
- Lifestyle adjustments: Making practical changes such as eating to prevent constipation, limiting sitting time, and gradually building up activity levels helps support long-term improvement and pelvic balance.
How We Can Help You with Testicular Pain
Men from Burbank who suffer from testicular pain may benefit from scheduling an assessment with a pelvic floor physical and occupational therapist specialising in men’s pelvic health. At PHRC, each evaluation begins with a discussion about your symptoms, previous diagnoses, and the treatments you have already pursued. The therapist works to identify which methods were effective and which ones were not in order to build a better plan for you.
Our Burbank therapists are fully aware that men dealing with chronic pelvic or testicular pain often arrive feeling defeated. We listen carefully, acknowledging your frustration and the difficult journey that has brought you to this point.
During your exam, the therapist performs a detailed assessment of your pelvic floor muscles, connective tissues, joints, and nerves, analysing movement to uncover the root cause of your discomfort. Once this evaluation is complete, your therapist shares the findings and outlines the specific factors contributing to your condition. A treatment plan is then created with short-term milestones and long-term strategies for recovery.

How We Can Help You with Testicular Pain
Men from Burbank who suffer from testicular pain may benefit from scheduling an assessment with a pelvic floor physical and occupational therapist specialising in men’s pelvic health. At PHRC, each evaluation begins with a discussion about your symptoms, previous diagnoses, and the treatments you have already pursued. The therapist works to identify which methods were effective and which ones were not in order to build a better plan for you.
Our Burbank therapists are fully aware that men dealing with chronic pelvic or testicular pain often arrive feeling defeated. We listen carefully, acknowledging your frustration and the difficult journey that has brought you to this point.
During your exam, the therapist performs a detailed assessment of your pelvic floor muscles, connective tissues, joints, and nerves, analysing movement to uncover the root cause of your discomfort. Once this evaluation is complete, your therapist shares the findings and outlines the specific factors contributing to your condition. A treatment plan is then created with short-term milestones and long-term strategies for recovery.

Your therapy typically takes place once or twice per week for about 12 weeks. You will also receive a customized home exercise plan to complement your in-clinic sessions, while your therapist collaborates with other healthcare providers as needed. PHRC Burbank is committed to helping you reduce pain, restore normal function, and regain your confidence.
