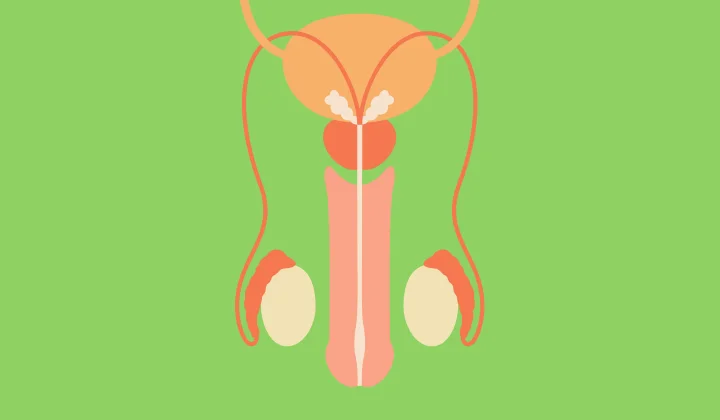
Are you based in Carlsbad or nearby and dealing with stubborn testicular pain? While infection is a common concern, the true cause may often involve pelvic floor dysfunction, nerve sensitivity from the lower spine, or restricted blood circulation within the pelvic area.
Because these symptoms are easily confused with those of prostatitis, many men receive antibiotics that fail to make a difference. Once medications prove ineffective, the source of the problem often lies in the muscles or nerves rather than an infection.
For men exploring non-surgical treatments near Carlsbad, pelvic floor physical and occupational therapy can be extremely helpful. These therapies reduce muscle tension, improve pelvic coordination, and relieve nerve pressure. This comprehensive approach provides both comfort and long-term functional improvement.
What are the Causes of Testicular Pain?
Several distinct medical conditions may lead to testicular pain, most commonly those associated with the lumbar spine, the vascular system, or the pelvic floor muscles.
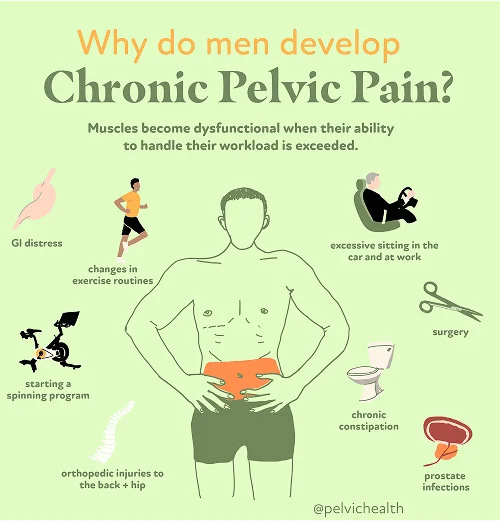
- Lumbar pathology: The nerve roots connected to the testicles trace back to the lower spine. Any irritation in this area caused by arthritis, herniated discs, or spinal compression can create pain that travels downward along the nerves. Although the pain feels localized to the testicle, the origin is usually within the lumbar spine.
- Vascular pathology: Circulatory issues are another frequent source. Problems like varicocele formation, testicular torsion, or venous pooling disrupt normal blood flow patterns. Such interference can lead to discomfort described as dull aching, pressure, or acute twinges in the scrotum.
- Pelvic floor pathology: The pelvic floor serves as a muscular base that holds and supports pelvic organs. If these muscles tighten excessively, become fatigued, or go into spasm, they may irritate nearby nerve pathways. This irritation can mimic testicular pain, even though the pain is generated from muscle dysfunction within the pelvic floor.
Additional causes of testicular pain can include:
- Surgical trauma (vasectomy, benign prostatic hyperplasia (BPH) interventions, prostatectomy)
- Biomechanical or structural dysfunction (hip dysfunction, piriformis syndrome, scoliosis, leg length discrepancy)
- Excessive exercise or changes to exercise routine
- Excessive sitting
- Chronic constipation and straining
- Jelqing and/or attempts at gential enhancement or foreskin regeneration
- In rare cases, bladder, prostate, or sexually transmitted infections after successful resolution of infection
- The majority of men with pelvic pain (including testicular pain), with or without urinary or bowel complaints, have pelvic floor dysfunction
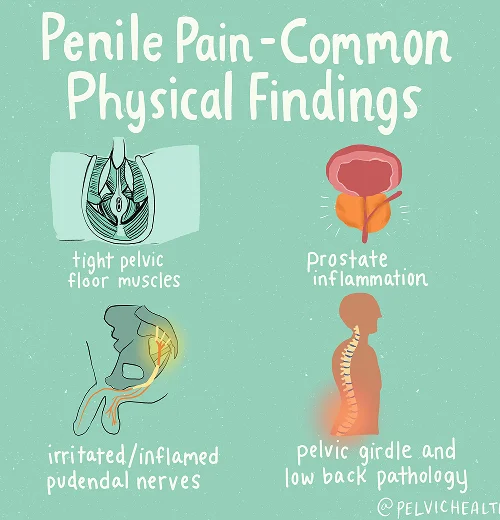

Symptoms of Testicular Pain
- A persistent aching or stinging feeling in the testicles is one of the most reported symptoms.
- This sensation can move outward into nearby regions such as the penis, perineum, and anus.
Additional issues commonly associated with this pain include:
- Worsening pelvic discomfort after long sitting sessions, physical activity, or tight clothing.
- Urinary changes such as an urgent need to urinate or weak urine flow.
- Ejaculation discomfort felt across the scrotum and perineal area.
- Reduced erectile function and ejaculation strength in some men.
- Digestive complaints such as bloating, abdominal heaviness, or constipation.
- These digestive problems may increase following physical strain or intercourse.
- Symptoms often fluctuate in severity, shifting between mild and intense phases.
Associated Diagnoses
Testicular and pelvic pain may develop from a combination of lumbar, vascular, and pelvic floor dysfunctions that influence one another in complex ways. Lumbar pathology typically involves nerve root irritation, herniated discs, or degenerative changes that cause pain to radiate into the pelvis. Vascular problems such as varicocele, testicular torsion, and pelvic venous congestion disturb normal blood circulation and lead to discomfort or swelling. Pelvic floor pathology often intertwines with these issues and is associated with Chronic Pelvic Pain Syndrome (CPPS), pudendal neuralgia, painful bladder syndrome, and hard flaccid syndrome. In many cases, the pelvic floor serves as the central point that magnifies or maintains pain resulting from spinal or circulatory dysfunction elsewhere in the body.
Diagnostic Challenges
Among men, testicular pain is a frequent medical complaint, but it is often inaccurately diagnosed as prostatitis. As a result, many patients receive antibiotics unnecessarily, even when testing reveals no sign of infection. Research continues to show that more than 90 percent of men with pelvic or genital discomfort do not suffer from a bacterial infection of the prostate gland.
Most of these presentations fall into the National Institutes of Health’s classifications of Category IIIa and IIIb, both parts of the chronic condition known as Chronic Pelvic Pain Syndrome (CPPS). At times, nerve compression in the lower back or vascular dysfunction can reproduce pelvic pain symptoms, leading to challenges in diagnosis and delays in proper care.
According to the National Institutes of Health, prostatitis syndromes can be categorized in the following way:
- Category I: Acute bacterial prostatitis manifests as sudden and sharp pelvic pain, high fever, and urinary infection caused by bacteria that inflame the prostate gland.
- Category II: Chronic bacterial prostatitis persists over time, bringing recurrent infections due to the same bacterial strain that repeatedly infects the prostate.
- Category IIIa: Inflammatory chronic pelvic pain syndrome reveals the presence of white blood cells in semen or prostatic fluids, confirming active inflammation.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome produces ongoing pain and discomfort, yet laboratory analysis detects no white blood cells or infection.
- Category IV: Asymptomatic inflammatory prostatitis shows hidden inflammation discovered through routine exams, even though the patient experiences no urinary or pain symptoms.

According to the National Institutes of Health, prostatitis syndromes can be categorized in the following way:
- Category I: Acute bacterial prostatitis manifests as sudden and sharp pelvic pain, high fever, and urinary infection caused by bacteria that inflame the prostate gland.
- Category II: Chronic bacterial prostatitis persists over time, bringing recurrent infections due to the same bacterial strain that repeatedly infects the prostate.
- Category IIIa: Inflammatory chronic pelvic pain syndrome reveals the presence of white blood cells in semen or prostatic fluids, confirming active inflammation.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome produces ongoing pain and discomfort, yet laboratory analysis detects no white blood cells or infection.
- Category IV: Asymptomatic inflammatory prostatitis shows hidden inflammation discovered through routine exams, even though the patient experiences no urinary or pain symptoms.

Treatment for Testicular Pain
Depending on what is found to be driving your pain, whether it is excessive muscle tension within the pelvic floor, nerve entrapment in the lower back, or limited circulation in the pelvic region, your care plan may include a variety of evidence-based therapies that promote healthy movement and function. These may include relaxation techniques, mobility exercises, and manual therapy to reduce restrictions and restore balance.
- Pelvic floor physical and occupational therapy for pelvic floor dysfunction: This specialized form of care uses relaxation, stretching, and coordination exercises to retrain muscles that may be overly tight or unresponsive. Over time, the body relearns how to function without unnecessary tension, resulting in less pain and greater comfort.
- Spine and back treatment: If imaging or examination shows irritation in the lumbar nerves, therapy aims to improve spinal strength, relieve compression, and promote proper movement patterns. In some cases, guided injections provide additional relief from inflammation.
- Vascular-related treatment: Addressing circulation is vital when blood flow is restricted. Therapists use techniques that reduce muscle pressure and enhance venous return through controlled posture and diaphragmatic breathing exercises.
- Addressing biomechanical issues: Correcting movement dysfunctions in the hips and pelvis can significantly ease discomfort. Therapeutic exercises restore proper mechanics and reduce excessive muscle strain in surrounding tissues.
- Lifestyle adjustments: Advice typically includes tips for maintaining healthy bowel function, taking breaks from sitting, and performing regular low-impact activities to help maintain pelvic stability.
How We Can Help You with Testicular Pain
Men from the Carlsbad area who continue to experience testicular pain may benefit from seeing a pelvic floor physical and occupational therapist who specializes in men’s pelvic health. At PHRC, each evaluation begins with a thorough review of your health background and prior treatments to uncover the possible causes of your discomfort.
We understand that many men from Carlsbad come to us after years of unsuccessful medical care. Our caring therapists take time to listen and provide guidance, ensuring that your treatment plan is well-organized and easy to follow.
During the examination, your therapist will assess your pelvic muscles, nerves, and tissues, paying close attention to how certain postures and movements may influence pain. Once the evaluation is complete, you will discuss your results in detail and establish achievable goals for your rehabilitation.

How We Can Help You with Testicular Pain
Men from the Carlsbad area who continue to experience testicular pain may benefit from seeing a pelvic floor physical and occupational therapist who specializes in men’s pelvic health. At PHRC, each evaluation begins with a thorough review of your health background and prior treatments to uncover the possible causes of your discomfort.
We understand that many men from Carlsbad come to us after years of unsuccessful medical care. Our caring therapists take time to listen and provide guidance, ensuring that your treatment plan is well-organized and easy to follow.
During the examination, your therapist will assess your pelvic muscles, nerves, and tissues, paying close attention to how certain postures and movements may influence pain. Once the evaluation is complete, you will discuss your results in detail and establish achievable goals for your rehabilitation.

Treatment typically involves one or two sessions per week over approximately 12 weeks, complemented by at-home exercises. Your PHRC therapist will communicate with your broader healthcare team to maintain continuity of care. Our goal is to help you overcome discomfort and regain confidence in your health.
