For men in Culver City who are struggling with unrelenting testicular pain finding answers can be frustrating. While it is easy to assume that infection is the cause, pain in this area is often linked to issues such as pelvic floor dysfunction, nerve irritation in the lower back, or circulation problems within the pelvic region.
Because these symptoms resemble prostatitis and other urological conditions, many men are treated with antibiotics that fail to bring relief. When such treatments do not work, it is a sign that the problem may come from muscle tightness or nerve entrapment rather than infection.
Men throughout Culver City and nearby neighborhoods may benefit from pelvic floor physical and occupational therapy. These approaches help loosen overactive muscles, restore coordination, and relieve pressure on nerves. Addressing the real cause of the discomfort helps achieve lasting relief and improved pelvic well-being./p>
What are the Causes of Testicular Pain?
The origins of testicular pain are often complex, with contributing factors that involve spinal, vascular, and muscular systems.
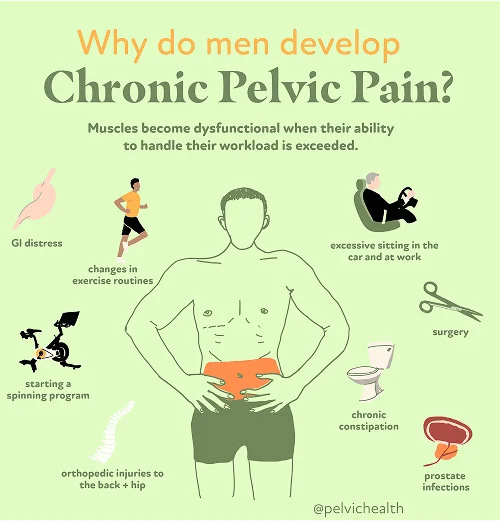
- Lumbar pathology: The lower back serves as the starting point for nerves that travel toward the testicles. Spinal abnormalities such as herniated discs, arthritis, or nerve root compression can trigger pain that radiates downward, resulting in referred pain within the testicular region.
- Vascular pathology: Blood flow disruption in the veins surrounding the testicles can cause sensations of heaviness or discomfort. Common vascular conditions include varicoceles, torsion, and pelvic venous congestion, each of which may produce persistent or acute testicular pain.
- Pelvic floor pathology: The pelvic floor muscles support vital pelvic structures. When these muscles are either overly tense or weakened, they can compress nerves that communicate with the testicles, leading to referred pain that feels internal though it originates from the pelvic musculature.
Additional causes of testicular pain can include:
- Surgical trauma (vasectomy, benign prostatic hyperplasia (BPH) interventions, prostatectomy)
- Biomechanical or structural dysfunction (hip dysfunction, piriformis syndrome, scoliosis, leg length discrepancy)
- Excessive exercise or changes to exercise routine
- Excessive sitting
- Chronic constipation and straining
- Jelqing and/or attempts at gential enhancement or foreskin regeneration
- In rare cases, bladder, prostate, or sexually transmitted infections after successful resolution of infection
- The majority of men with pelvic pain (including testicular pain), with or without urinary or bowel complaints, have pelvic floor dysfunction
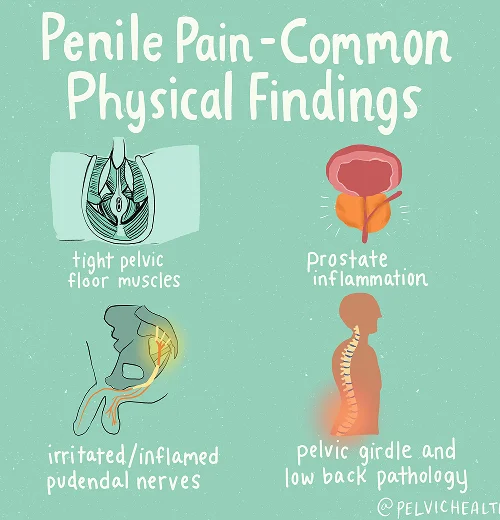

Symptoms of Testicular Pain
- Testicular discomfort often appears as a burning or throbbing ache that may fluctuate between mild and intense.
- The sensation can travel into nearby areas such as the penis, perineum, anus, or lower abdomen, affecting overall pelvic comfort.
Men with ongoing pain may also experience a wide range of associated symptoms:
- Pelvic soreness tends to increase after sitting for long intervals, completing strenuous workouts, or wearing clothing that restricts circulation.
- Urinary disturbances, including difficulty initiating urination, increased frequency, or a weak urine stream, are commonly observed.
- Discomfort during ejaculation is another frequent concern, often spreading across the penis, perineum, or scrotal tissues.
- Some men also report erectile dysfunction or a reduction in ejaculation pressure and volume.
- Digestive problems such as bloating, gas retention, or constipation often appear concurrently, intensifying pelvic tension.
- These digestive sensations may flare up unpredictably after exertion, intercourse, or sometimes without any identifiable cause.
- The duration and severity of symptoms can vary considerably, presenting intermittently or persisting over time.
Associated Diagnoses
Testicular and pelvic pain often arise from the combined influence of lumbar, vascular, and pelvic floor dysfunctions that coexist and reinforce each other. Lumbar pathology can take the form of radiculopathy or referred pain caused by herniated discs, arthritic joints, or nerve compression in the lower spine. Vascular pathology may include varicocele, testicular torsion, or pelvic venous congestion, all of which restrict normal circulation and result in deep aching pain in the pelvis. Pelvic floor dysfunction connects closely with conditions like Chronic Pelvic Pain Syndrome (CPPS), painful bladder syndrome, hard flaccid syndrome, and pudendal neuralgia. In many cases, the pelvic floor serves as the focal point where pain begins or is intensified by other underlying conditions.
Diagnostic Challenges
Testicular discomfort is one of the most common symptoms reported by men, yet it is often incorrectly diagnosed as prostatitis. In numerous situations, antibiotics are administered unnecessarily even though bacterial testing returns negative. Scientific research has confirmed that more than 90 percent of individuals with pelvic or genital pain do not actually have an infection of the prostate gland.
A majority of these men fit within the National Institutes of Health classifications known as Category IIIa and Category IIIb, both of which represent different forms of Chronic Pelvic Pain Syndrome (CPPS). In some cases, pain is worsened or caused by irritation of nerves in the lower back or poor blood flow, both of which can reproduce symptoms resembling pelvic floor dysfunction and delay accurate diagnosis.
The National Institutes of Health has defined prostatitis syndromes in the following manner:
- Category I: Acute bacterial prostatitis presents with sudden pelvic pain, urinary urgency, and fever caused by bacterial infection of the prostate gland.
- Category II: Chronic bacterial prostatitis persists over a long period and leads to recurrent urinary infections caused by the same bacteria.
- Category IIIa: Inflammatory chronic pelvic pain syndrome occurs when inflammatory cells are found in prostate secretions or semen samples.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome mirrors the same symptoms yet presents no evidence of inflammation in testing.
- Category IV: Asymptomatic inflammatory prostatitis reveals silent inflammation within the prostate discovered incidentally during medical testing.

The National Institutes of Health has defined prostatitis syndromes in the following manner:
- Category I: Acute bacterial prostatitis presents with sudden pelvic pain, urinary urgency, and fever caused by bacterial infection of the prostate gland.
- Category II: Chronic bacterial prostatitis persists over a long period and leads to recurrent urinary infections caused by the same bacteria.
- Category IIIa: Inflammatory chronic pelvic pain syndrome occurs when inflammatory cells are found in prostate secretions or semen samples.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome mirrors the same symptoms yet presents no evidence of inflammation in testing.
- Category IV: Asymptomatic inflammatory prostatitis reveals silent inflammation within the prostate discovered incidentally during medical testing.

Treatment for Testicular Pain
Depending on the underlying factors involved, whether your discomfort results from muscle tightness in the pelvic floor, nerve inflammation in the lower spine, or blood flow restrictions throughout the pelvis, your therapist will develop a plan using a range of treatments to restore normal pelvic activity. This may include hands-on therapy, relaxation training, and corrective exercises tailored to your condition.
- Pelvic floor physical and occupational therapy for pelvic floor dysfunction: This therapeutic method aims to release tension in overactive muscles, restore coordination between the pelvic floor and surrounding structures, and calm irritated nerves. Through repeated sessions, it enhances circulation, reduces discomfort, and supports smoother motion throughout the day.
- Spine and back treatment: When pain stems from lower back nerve compression, treatment focuses on improving posture, retraining movement, and sometimes using guided injections to decrease swelling and nerve pressure. These strategies help the spine move more freely and reduce referred pain in the pelvis.
- Vascular-related treatment: When reduced circulation is a factor, pelvic therapy can improve blood flow and ease venous pressure by combining muscle relaxation techniques with breathing and posture exercises. The improved circulation aids tissue recovery and overall pelvic wellness.
- Addressing biomechanical issues: If the hips or lower back are not moving correctly, customized exercises and mobility work can restore proper mechanics, relieve stiffness, and improve balance. These adjustments help lower the strain placed on pelvic muscles during daily activity.
- Lifestyle adjustments: Recommendations often include learning how to manage bowel movements, avoiding prolonged sitting, and carefully adding light exercise into the routine. These changes support continued healing and prevent unnecessary irritation to the pelvic area.
How We Can Help You with Testicular Pain
Men living in or around Culver City who are dealing with chronic testicular pain should consider scheduling an evaluation with a pelvic floor physical and occupational therapist. At PHRC, we begin every appointment by thoroughly discussing your symptoms, previous diagnoses, and any past treatments to gain a clear understanding of what you have already experienced. This process allows us to identify the possible sources of your pain and create a focused plan for recovery.
Many men who contact us from the Culver City community share stories of years spent searching for answers. Our team understands how discouraging that can be, and we pride ourselves on listening carefully and providing reassurance through a detailed, goal-oriented treatment plan.
During your evaluation, your therapist examines the pelvic floor muscles, surrounding nerves, and connective tissues while also observing how your daily movements might influence your pain. Once the assessment is complete, your therapist reviews your results, explains why the discomfort may have developed, and outlines practical steps toward improvement.

How We Can Help You with Testicular Pain
Men living in or around Culver City who are dealing with chronic testicular pain should consider scheduling an evaluation with a pelvic floor physical and occupational therapist. At PHRC, we begin every appointment by thoroughly discussing your symptoms, previous diagnoses, and any past treatments to gain a clear understanding of what you have already experienced. This process allows us to identify the possible sources of your pain and create a focused plan for recovery.
Many men who contact us from the Culver City community share stories of years spent searching for answers. Our team understands how discouraging that can be, and we pride ourselves on listening carefully and providing reassurance through a detailed, goal-oriented treatment plan.
During your evaluation, your therapist examines the pelvic floor muscles, surrounding nerves, and connective tissues while also observing how your daily movements might influence your pain. Once the assessment is complete, your therapist reviews your results, explains why the discomfort may have developed, and outlines practical steps toward improvement.

Therapy is generally provided one or two times per week for about 12 weeks. You will also receive individualized home exercises to strengthen your progress between sessions. Your PHRC therapist works closely with your existing healthcare team to maintain consistency and continuity of care. Our aim is to help you find lasting relief and regain control of your daily life.
