Are you dealing with testicular pain in Echo Park that just won’t go away? Many men assume this kind of discomfort results from infection, but it is often linked to other causes such as pelvic floor dysfunction, nerve irritation in the lower back, or restricted blood circulation within the pelvic area.
Because these symptoms can mimic other urological conditions, testicular pain is frequently misdiagnosed as prostatitis. As a result, many men undergo unnecessary courses of antibiotics that do little to address the real issue. When antibiotics do not work, the true cause is often muscular or neurological.
Pelvic floor physical and occupational therapy in Echo Park provides a non-invasive and effective path to recovery. These therapies help relieve tight or overactive pelvic muscles, improve coordination between the pelvic floor and core, and reduce pressure on affected nerves. This holistic approach targets the root cause of the pain and helps men achieve long-term relief and better pelvic function.
What are the Causes of Testicular Pain?
There are several potential causes of testicular pain, including those that stem from lumbar pathology, vascular pathology, and pelvic floor pathology.
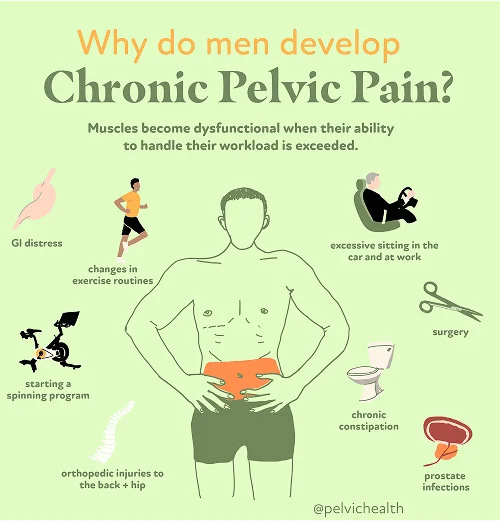
- Lumbar pathology: Because the nerves that serve the testicles begin in the lower back, conditions such as a herniated disc, lumbar arthritis, or nerve irritation can refer pain downward to the testicle, even though the discomfort originates from the spine.
- Vascular pathology: Circulatory problems such as varicoceles, torsion, or congestion of the veins can disrupt normal blood flow, resulting in sensations of dull aching, heaviness, or acute pain in the testicle.
- Pelvic floor pathology: The pelvic floor acts as a supportive network of muscles beneath the pelvis. When these muscles become too tight, weak, or experience spasms, they may irritate nerves and send pain signals that feel like they are coming from inside the testicle even though they arise from muscle tension.
Additional causes of testicular pain can include:
- Surgical trauma (vasectomy, benign prostatic hyperplasia (BPH) interventions, prostatectomy)
- Biomechanical or structural dysfunction (hip dysfunction, piriformis syndrome, scoliosis, leg length discrepancy)
- Excessive exercise or changes to exercise routine
- Excessive sitting
- Chronic constipation and straining
- Jelqing and/or attempts at gential enhancement or foreskin regeneration
- In rare cases, bladder, prostate, or sexually transmitted infections after successful resolution of infection
- The majority of men with pelvic pain (including testicular pain), with or without urinary or bowel complaints, have pelvic floor dysfunction
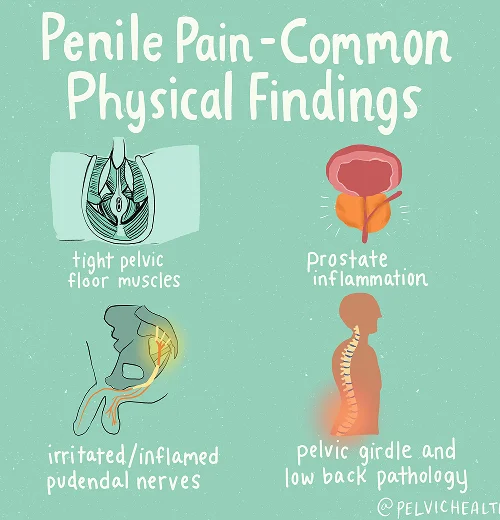

Symptoms of Testicular Pain
- A burning, sharp, or aching sensation in the testicles
- These sensations may extend into surrounding areas, including the penis, scrotum, perineum, and anus
In addition to testicular discomfort, men often report several accompanying symptoms:
- Pelvic pain that worsens during prolonged sitting, after physical activities, or when wearing tight-fitting garments
- Urinary symptoms such as urgency, frequency, and a slower, weaker urinary stream are common
- Men may feel discomfort or pain in the penis, scrotum, or perineum during ejaculation
- Erectile difficulties and reduced ejaculation strength may also occur in some cases
- Digestive distress such as bloating, constipation, and general gastrointestinal discomfort is also reported
- These digestive issues may flare up after ejaculation, following exercise, or without any clear reason
- Symptoms can fluctuate in intensity, appearing at intervals or continuing persistently
Associated Diagnoses
Testicular and pelvic discomfort may stem from a combination of lumbar, vascular, and pelvic floor dysfunctions, which frequently coexist and influence one another. Lumbar pathology typically manifests as lumbar radiculopathy or referred pain caused by disc damage, arthritis, or compression within the lower spinal region. Vascular pathology involves problems such as varicocele, testicular torsion, and pelvic venous congestion, all of which disturb normal blood flow and create painful sensations in the pelvic region. Pelvic floor pathology remains closely connected with Chronic Pelvic Pain Syndrome (CPPS), pudendal neuralgia, hard flaccid syndrome, and painful bladder syndrome. In many patients, the pelvic floor becomes the central element that either initiates the pain process or amplifies discomfort resulting from structural or vascular disturbances elsewhere in the body.
Diagnostic Challenges
Testicular pain is a common complaint among men, yet it is frequently misdiagnosed as prostatitis. In many of these cases, antibiotics are prescribed unnecessarily because no bacterial infection is found. Studies consistently reveal that more than 90 percent of men who experience pelvic or genital pain symptoms do not have a bacterial infection of the prostate.
The majority of such cases fit within the National Institutes of Health categories IIIa and IIIb, which are both part of the broader diagnosis of Chronic Pelvic Pain Syndrome (CPPS). Additionally, nerve irritation in the lumbar region and vascular dysfunction can imitate the pain patterns of pelvic floor dysfunction, making accurate diagnosis more difficult and delaying appropriate treatment.
According to the National Institutes of Health, prostatitis syndromes are classified as follows:
- Category I: Acute bacterial prostatitis, marked by intense pain, fever, and urinary tract infection due to bacterial infection.
- Category II: Chronic bacterial prostatitis, involving persistent prostate infection with recurring urinary tract infections caused by the same strain of bacteria.
- Category IIIa: Inflammatory chronic pelvic pain syndrome, characterized by the presence of white blood cells in semen, expressed prostatic secretions, or the third sample of urine.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome, which presents without white blood cells in any of these samples.
- Category IV: Asymptomatic inflammatory prostatitis, where inflammation exists within the prostate despite the absence of pain or urinary tract symptoms.

According to the National Institutes of Health, prostatitis syndromes are classified as follows:
- Category I: Acute bacterial prostatitis, marked by intense pain, fever, and urinary tract infection due to bacterial infection.
- Category II: Chronic bacterial prostatitis, involving persistent prostate infection with recurring urinary tract infections caused by the same strain of bacteria.
- Category IIIa: Inflammatory chronic pelvic pain syndrome, characterized by the presence of white blood cells in semen, expressed prostatic secretions, or the third sample of urine.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome, which presents without white blood cells in any of these samples.
- Category IV: Asymptomatic inflammatory prostatitis, where inflammation exists within the prostate despite the absence of pain or urinary tract symptoms.

Treatment for Testicular Pain
Depending on the underlying reason for your discomfort, whether it stems from tight or overactive pelvic floor muscles, nerve irritation in the lower back, or circulation-related issues; your treatment plan may include a combination of several therapeutic approaches designed to restore normal pelvic function.
- Pelvic floor physical and occupational therapy for pelvic floor dysfunction: This form of therapy focuses on relaxing overly tense muscles, improving coordination, and soothing any irritation affecting the pelvic nerves. Over time, this can greatly reduce pain and improve daily comfort.
- Spine and back treatment: If the pain originates from nerve irritation or compression in the lumbar spine, treatment may include targeted physical and occupational therapy, posture correction, and in some cases, guided injections to address inflammation and nerve sensitivity.
- Vascular-related treatment: When poor blood flow contributes to the discomfort, pelvic floor physical and occupational therapy can help relieve tension, encourage healthier circulation through proper breathing and posture techniques, and decrease pressure on veins that may be congested.
- Addressing biomechanical issues: For men whose pain is influenced by misalignment or limited movement in the hips, targeted therapy and corrective exercises can improve mobility, balance, and muscle mechanics to reduce strain on the pelvic region.
- Lifestyle adjustments: This may involve strategies for preventing constipation, reducing long periods of sitting, and reintroducing physical activity gradually to prevent overstressing the pelvic area.
How We Can Help You with Testicular Pain
Men from Echo Park who experience ongoing testicular pain can benefit from a professional evaluation with a pelvic floor physical and occupational therapist who specialises in pelvic pain conditions. At PHRC, we begin each evaluation with an in-depth discussion of your medical background, past diagnoses, symptoms, and the effectiveness of any treatments you have already undergone. This helps identify the underlying causes of your discomfort and the best next steps.
We know that many Echo Park men arrive at our clinic feeling frustrated and hopeless after years of ineffective treatments. Our compassionate therapists take time to listen and provide a clear, structured plan that brings clarity and direction.
During the physical exam, your therapist examines your pelvic floor muscles, nearby tissues, nerves, and joints, and evaluates how your movements may be contributing to pain. After completing the assessment, your therapist discusses your results with you, outlines how your pain developed, and sets realistic short- and long-term goals to guide your treatment.

How We Can Help You with Testicular Pain
Men from Echo Park who experience ongoing testicular pain can benefit from a professional evaluation with a pelvic floor physical and occupational therapist who specialises in pelvic pain conditions. At PHRC, we begin each evaluation with an in-depth discussion of your medical background, past diagnoses, symptoms, and the effectiveness of any treatments you have already undergone. This helps identify the underlying causes of your discomfort and the best next steps.
We know that many Echo Park men arrive at our clinic feeling frustrated and hopeless after years of ineffective treatments. Our compassionate therapists take time to listen and provide a clear, structured plan that brings clarity and direction.
During the physical exam, your therapist examines your pelvic floor muscles, nearby tissues, nerves, and joints, and evaluates how your movements may be contributing to pain. After completing the assessment, your therapist discusses your results with you, outlines how your pain developed, and sets realistic short- and long-term goals to guide your treatment.

Therapy typically occurs one to two times weekly for a period of roughly 12 weeks. You’ll also receive a set of home exercises designed to enhance your recovery between sessions. Your PHRC Echo Park therapist will collaborate with your wider healthcare team to ensure a fully coordinated approach to your rehabilitation. Our mission is to help you finally experience relief and reclaim your wellbeing.
