If you live in Encino or are nearby and dealing with ongoing testicular pain, it is important to know that infection is not always the culprit. Chronic discomfort in this area can stem from pelvic floor dysfunction, irritated nerves in the lower back, or even limited circulation to the pelvic region.
Because these symptoms often look identical to those of prostatitis, testicular pain is sometimes misdiagnosed. As a result, many men undergo several rounds of antibiotics that do little to resolve the pain. When medication offers no improvement, it often indicates a muscular or neurological source.
Men throughout Encino who are exploring their options may find that pelvic floor physical and occupational therapy offer relief. These therapies work to reduce pelvic muscle tightness, enhance coordination, and release pressure on sensitive nerves. This restorative approach helps men regain comfort and long-term pelvic function naturally.
What are the Causes of Testicular Pain?
There are numerous reasons why men may experience testicular pain, many of which relate to lumbar, vascular, or pelvic floor dysfunction.
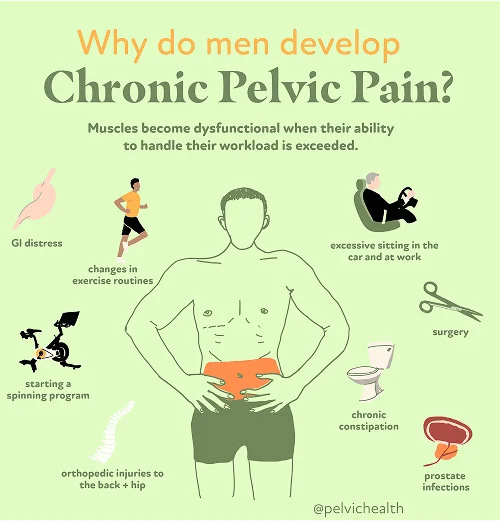
- Lumbar pathology: The nerves responsible for testicular sensation branch out from the lumbar region. Any injury or degenerative change within the spine such as herniation, arthritis, or nerve impingement can result in pain that radiates downward, creating the illusion that the testicle itself is the problem.
- Vascular pathology: Conditions that disturb normal circulation, including varicoceles, torsion, and pelvic venous congestion, can generate discomfort or throbbing pain within the scrotal region. This occurs as a result of impaired blood drainage and pressure buildup.
- Pelvic floor pathology: The pelvic floor’s muscular foundation plays a major role in posture and organ support. When these muscles are tense or fatigued, they can compress or irritate nerves that transmit pain to the testicular area, producing sensations unrelated to direct injury.
Additional causes of testicular pain can include:
- Surgical trauma (vasectomy, benign prostatic hyperplasia (BPH) interventions, prostatectomy)
- Biomechanical or structural dysfunction (hip dysfunction, piriformis syndrome, scoliosis, leg length discrepancy)
- Excessive exercise or changes to exercise routine
- Excessive sitting
- Chronic constipation and straining
- Jelqing and/or attempts at gential enhancement or foreskin regeneration
- In rare cases, bladder, prostate, or sexually transmitted infections after successful resolution of infection
- The majority of men with pelvic pain (including testicular pain), with or without urinary or bowel complaints, have pelvic floor dysfunction
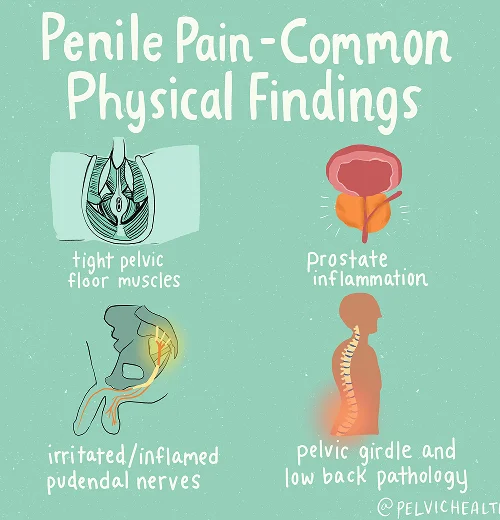

Symptoms of Testicular Pain
- Men affected by testicular pain often describe sensations that range from sharp and shooting to dull and aching.
- This pain can extend beyond the testicles, radiating into the penis, scrotum, or even deep into the perineal and anal regions.
Additional symptoms frequently accompany these sensations, providing a clearer picture of the problem:
- Pelvic pain tends to intensify during prolonged sitting, following physical activities, or when tight garments compress the area.
- Common urinary difficulties include a weak flow, frequent urination, or the urge to urinate more often than usual.
- During ejaculation, many men notice tenderness or pressure that can affect the scrotum or perineum.
- Erectile changes, such as decreased firmness or weaker ejaculation, can also arise.
- Digestive complaints like bloating, constipation, and abdominal heaviness often coexist with pelvic pain.
- These digestive issues might become worse following exertion, ejaculation, or at random times throughout the day.
- Symptoms can be unpredictable, sometimes disappearing for days or persisting steadily without relief.
Associated Diagnoses
Discomfort in the testicular and pelvic regions can originate from multiple overlapping dysfunctions involving the lumbar spine, vascular system, and pelvic floor. Lumbar pathology often appears as nerve irritation or referred pain linked to degenerative changes, herniated discs, or spinal compression. Vascular causes, such as varicocele, testicular torsion, and pelvic venous congestion, interrupt normal blood flow and contribute to persistent pelvic pain. Pelvic floor dysfunction is frequently associated with Chronic Pelvic Pain Syndrome (CPPS), pudendal neuralgia, hard flaccid syndrome, and painful bladder syndrome. In numerous patients, the pelvic floor becomes the central link that initiates, maintains, or worsens pain originating from either vascular or spinal abnormalities.
Diagnostic Challenges
Many men complain of testicular pain, but it is frequently misidentified as prostatitis, resulting in treatments that may not address the true cause. Antibiotics are often prescribed, even when testing reveals no bacterial infection present in the prostate. Medical research has found that more than 90 percent of men who live with pelvic or genital pain are not experiencing a bacterial infection.
Most of these cases fall within the National Institutes of Health’s Category IIIa and IIIb, both part of the larger Chronic Pelvic Pain Syndrome (CPPS) diagnosis. Additional factors such as nerve irritation stemming from the lumbar spine or vascular complications may mimic the same type of pelvic discomfort, which often leads to confusion in diagnosis and delays effective management.
Based on the guidelines from the National Institutes of Health, prostatitis-related syndromes are divided as follows:
- Category I: Acute bacterial prostatitis results from bacterial contamination of the prostate, leading to acute inflammation, pain, fever, and urinary symptoms.
- Category II: Chronic bacterial prostatitis develops when infection persists in the prostate, resulting in repeated urinary tract infections from the same bacterial source.
- Category IIIa:Inflammatory chronic pelvic pain syndrome includes the presence of immune cells in the prostate secretions, indicating inflammation.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome shares pain symptoms but lacks the same cellular inflammatory markers.
- Category IV: Asymptomatic inflammatory prostatitis involves internal inflammation with no noticeable pain or urinary disturbance.

Based on the guidelines from the National Institutes of Health, prostatitis-related syndromes are divided as follows:
- Category I: Acute bacterial prostatitis results from bacterial contamination of the prostate, leading to acute inflammation, pain, fever, and urinary symptoms.
- Category II: Chronic bacterial prostatitis develops when infection persists in the prostate, resulting in repeated urinary tract infections from the same bacterial source.
- Category IIIa:Inflammatory chronic pelvic pain syndrome includes the presence of immune cells in the prostate secretions, indicating inflammation.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome shares pain symptoms but lacks the same cellular inflammatory markers.
- Category IV: Asymptomatic inflammatory prostatitis involves internal inflammation with no noticeable pain or urinary disturbance.

Treatment for Testicular Pain
Depending on the primary cause of your discomfort, whether it arises from pelvic floor muscles that are too tight or overactive, irritation of nearby nerves in the lumbar region, or circulation-related problems affecting the pelvic area, your therapist may recommend several treatment techniques that work in combination to restore balance and promote proper function. This approach helps address both muscular and neurological elements of the pain.
- Pelvic floor physical and occupational therapy for pelvic floor dysfunction: This therapy works by helping the muscles of the pelvic floor relax and regain healthy function. Techniques such as stretching, manual therapy, and breathing coordination help reduce irritation around the nerves and encourage balanced muscle movement, which leads to less pain and improved comfort.
- Spine and back treatment: If your pain is connected to spinal nerve irritation, targeted therapy sessions will focus on spinal stability, posture, and body mechanics. At times, guided injections can be used alongside therapy to decrease inflammation and relieve nerve stress.
- Vascular-related treatment: When poor blood circulation contributes to pelvic pain, therapy may involve relaxation and posture-based strategies to help open the pelvic vessels, improve oxygen flow, and ease vein congestion. This process supports tissue recovery and lowers discomfort.
- Addressing biomechanical issues: Men who have tight hips or limited movement often benefit from corrective exercises that improve strength, flexibility, and joint mobility. These techniques help restore balance and reduce unnecessary tension on the pelvic region.
- Lifestyle adjustments: Your therapist may also recommend simple changes such as avoiding long sitting periods, improving hydration and diet to prevent constipation, and slowly increasing activity levels as your body adapts. These daily habits enhance the results of therapy.
How We Can Help You with Testicular Pain
For men in Encino experiencing testicular pain that has persisted for months or even years, working with a pelvic floor physical and occupational therapist could be a life-changing step. PHRC begins each evaluation with a comprehensive discussion about your health history, previous treatments, and current symptoms to ensure that we understand the full picture before moving forward. This initial review helps pinpoint the true cause of your pain and guides our clinical recommendations.
We know that many men from Encino seek our expertise after being disappointed by years of temporary or ineffective treatments. Our therapists approach each case with empathy and thoroughness, taking the time to explain your condition and provide a clear strategy for improvement.
During your examination, your therapist will assess your pelvic floor muscles, surrounding soft tissues, and joints, and will observe how your movements may affect your symptoms. After the evaluation, you will receive a detailed explanation of your findings, an overview of how your pain developed, and both short- and long-term treatment goals to track your recovery.

How We Can Help You with Testicular Pain
For men in Encino experiencing testicular pain that has persisted for months or even years, working with a pelvic floor physical and occupational therapist could be a life-changing step. PHRC begins each evaluation with a comprehensive discussion about your health history, previous treatments, and current symptoms to ensure that we understand the full picture before moving forward. This initial review helps pinpoint the true cause of your pain and guides our clinical recommendations.
We know that many men from Encino seek our expertise after being disappointed by years of temporary or ineffective treatments. Our therapists approach each case with empathy and thoroughness, taking the time to explain your condition and provide a clear strategy for improvement.
During your examination, your therapist will assess your pelvic floor muscles, surrounding soft tissues, and joints, and will observe how your movements may affect your symptoms. After the evaluation, you will receive a detailed explanation of your findings, an overview of how your pain developed, and both short- and long-term treatment goals to track your recovery.

Most clients participate in therapy sessions once or twice a week over a period of approximately 12 weeks, complemented by customized home exercises. Throughout your care, your PHRC therapist will coordinate with your broader medical team, ensuring a seamless and effective plan. Our purpose is to help you feel genuine relief and return to a higher quality of life.
