Are you in or near Los Angeles and dealing with testicular pain that simply will not go away? Many men assume this type of pain is caused by an infection, yet the truth is that it can often come from issues unrelated to bacteria. Conditions such as pelvic floor dysfunction, nerve irritation from the lower back, or reduced blood circulation in the pelvic region can all contribute to lingering discomfort that affects daily life.
Because these symptoms often mimic other urological conditions, men sometimes receive a diagnosis of prostatitis even when the root cause lies elsewhere. This misunderstanding leads to repeated rounds of antibiotics that bring little improvement. When those medications fail to relieve the pain, the underlying cause is often muscular or neurological instead of infectious.
For men in Los Angeles and surrounding areas, pelvic floor physical and occupational therapy can be a practical and non-invasive option for relief. These therapies focus on relaxing tense pelvic muscles, improving coordination between the pelvic floor and core, and reducing strain on irritated nerves. By addressing the true cause of the problem, this approach supports long-term comfort and improved pelvic function.
What are the Causes of Testicular Pain?
A wide range of underlying issues may produce testicular pain, with the most common being lumbar, vascular, and pelvic floor pathologies.
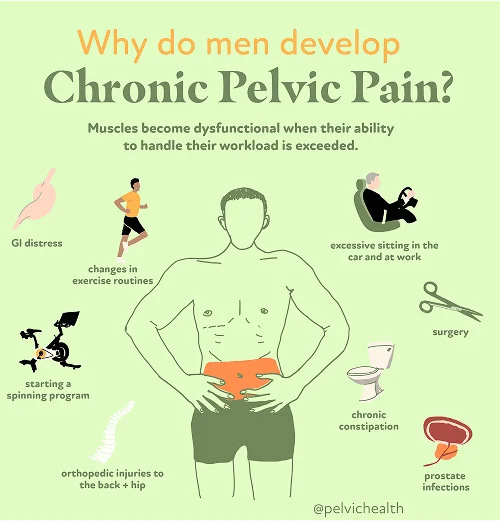
- Lumbar pathology: The testicular nerves originate from the lower spine, meaning that lumbar problems such as disc bulging, arthritis, or nerve compression can send referred pain signals downward to the testicle. The discomfort is therefore spinal in nature even though it appears to be local.
- Vascular pathology: Circulatory dysfunctions such as varicoceles, torsion, or venous congestion may interrupt normal blood flow to the testicular area. This typically manifests as aching, pressure, or sharp episodic pain.
- Pelvic floor pathology: The pelvic floor muscles create a supportive base for the pelvis. When they become tight or unbalanced, they can pinch or irritate surrounding nerves. This often results in sensations that feel like they are coming directly from the testicle when in fact the pain originates from the muscular system.
Additional causes of testicular pain can include:
- Surgical trauma (vasectomy, benign prostatic hyperplasia (BPH) interventions, prostatectomy)
- Biomechanical or structural dysfunction (hip dysfunction, piriformis syndrome, scoliosis, leg length discrepancy)
- Excessive exercise or changes to exercise routine
- Excessive sitting
- Chronic constipation and straining
- Jelqing and/or attempts at gential enhancement or foreskin regeneration
- In rare cases, bladder, prostate, or sexually transmitted infections after successful resolution of infection
- The majority of men with pelvic pain (including testicular pain), with or without urinary or bowel complaints, have pelvic floor dysfunction
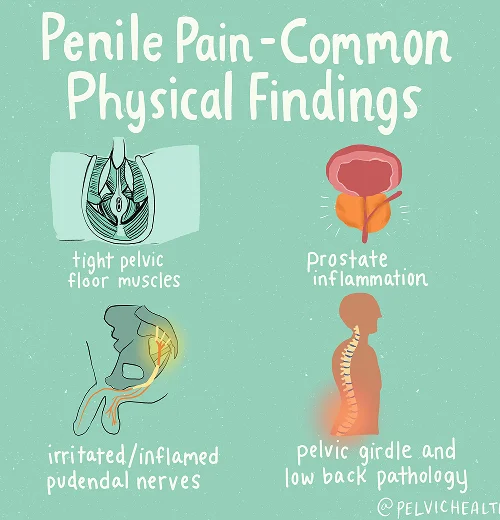

Symptoms of Testicular Pain
- A burning, sharp, or deep aching sensation may develop within the testicles, sometimes varying in intensity throughout the day.
- These uncomfortable feelings can radiate into neighbouring regions such as the penis, scrotum, perineum, or anal area, creating a broader sense of pelvic tension.
In many men, this testicular discomfort is accompanied by other symptoms that provide further insight into the underlying condition:
- Pelvic pain may intensify during long periods of sitting, after strenuous activity, or while wearing restrictive clothing that places added pressure on the groin.
- Urinary disturbances, including increased urgency, frequent trips to the bathroom, and a weak or interrupted stream, are often reported.
- Some men also describe pain or pressure during ejaculation, with discomfort extending through the penis, scrotum, or perineum.
- Erectile challenges and a noticeable decrease in ejaculation force can occasionally appear alongside these sensations.
- Digestive symptoms such as constipation, abdominal bloating, and a heavy feeling in the lower abdomen are also common.
- These gastrointestinal disturbances might worsen following sexual activity, exercise, or even occur spontaneously without a clear trigger.
- Overall, symptom intensity can rise and fall unpredictably, either appearing periodically or persisting over extended periods.
Associated Diagnoses
Testicular and pelvic discomfort frequently have overlapping causes involving the lumbar spine, vascular system, and pelvic floor muscles, which tend to influence each other’s function. Lumbar pathology may appear as nerve compression, referred pain, or radiculopathy resulting from disc herniation, spinal arthritis, or degenerative changes in the lower back. Vascular problems such as varicocele, testicular torsion, and pelvic venous congestion hinder proper circulation and lead to persistent pelvic pain. Pelvic floor dysfunction, strongly associated with Chronic Pelvic Pain Syndrome (CPPS), pudendal neuralgia, hard flaccid syndrome, and painful bladder syndrome, is often the unifying factor. For many individuals, it becomes the central element that either initiates discomfort or amplifies pain originating from other regions of the body.
Diagnostic Challenges
Testicular pain is a frequent concern for men, yet it is often mistakenly labeled as prostatitis. In many instances, antibiotics are prescribed despite there being no evidence of a bacterial infection. Research consistently shows that over 90 percent of men who report pelvic or genital discomfort do not actually have an infection of the prostate.
Most of these situations fall within the National Institutes of Health classifications of Category IIIa or Category IIIb, both of which belong to a larger group known as Chronic Pelvic Pain Syndrome (CPPS). In addition, irritation of nerves in the lower back or restricted blood flow in the pelvic region can mimic the same pain felt with pelvic floor dysfunction, which makes diagnosis more complex and can delay proper therapy.
According to the National Institutes of Health, prostatitis-related syndromes are categorized as follows:
- Category I: Acute bacterial prostatitis causes severe pelvic discomfort, fever, and urinary infection linked to an active bacterial process in the prostate.
- Category II: Chronic bacterial prostatitis remains persistent, with the same bacterial strain responsible for ongoing prostate inflammation and repeated infections.
- Category IIIa: Inflammatory chronic pelvic pain syndrome demonstrates inflammation detected by white blood cells in seminal or prostate fluid samples.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome has similar pain patterns but shows no sign of inflammation in medical tests.
- Category IV: Asymptomatic inflammatory prostatitis involves inflammation within the prostate found through evaluation despite an absence of physical symptoms.

According to the National Institutes of Health, prostatitis-related syndromes are categorized as follows:
- Category I: Acute bacterial prostatitis causes severe pelvic discomfort, fever, and urinary infection linked to an active bacterial process in the prostate.
- Category II: Chronic bacterial prostatitis remains persistent, with the same bacterial strain responsible for ongoing prostate inflammation and repeated infections.
- Category IIIa: Inflammatory chronic pelvic pain syndrome demonstrates inflammation detected by white blood cells in seminal or prostate fluid samples.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome has similar pain patterns but shows no sign of inflammation in medical tests.
- Category IV: Asymptomatic inflammatory prostatitis involves inflammation within the prostate found through evaluation despite an absence of physical symptoms.

Treatment for Testicular Pain
Depending on the source of your discomfort, whether it comes from hyperactive pelvic floor muscles, nerve compression originating in the lower back, or decreased blood flow through the pelvic region, your therapist may employ a combination of techniques aimed at promoting mobility and normalizing pelvic floor function. This integrated plan helps release tight muscles, ease nerve tension, and restore natural balance.
- Pelvic floor physical and occupational therapy for pelvic floor dysfunction: This type of therapy is designed to retrain and relax tight or overactive muscles within the pelvic floor, improve the way these muscles coordinate with your core, and ease any irritation or tension affecting nearby nerves. With consistent treatment, many patients experience significant reductions in discomfort and better overall function during daily activities.
- Spine and back treatment: When discomfort is traced to nerve irritation or compression within the lumbar spine, treatment often involves a tailored combination of physical and occupational therapy sessions, posture correction strategies, and occasionally guided injections to reduce inflammation, calm nerve sensitivity, and restore balance through the spine.
- Vascular-related treatment: In cases where poor circulation plays a role in pelvic pain, therapy can be used to relieve muscular tension, improve blood flow through posture and breathing training, and reduce congestion or pressure on sensitive veins in the area. Improved circulation helps tissues heal and function more efficiently.
- Addressing biomechanical issues: For men whose symptoms stem from structural imbalance or restricted hip movement, focused manual therapy and corrective exercises work to enhance alignment, coordination, and flexibility. This helps decrease unnecessary strain and supports smoother movement throughout the pelvic region.
- Lifestyle adjustments: The therapist may also recommend simple but meaningful changes such as increasing daily mobility, improving bowel habits to prevent constipation, taking frequent standing breaks, and reintroducing physical activity in a controlled way to protect the pelvic floor during recovery.
How We Can Help You with Testicular Pain
Men in or near Los Angeles who are struggling with testicular pain that will not subside may benefit from seeking a professional assessment with a pelvic floor physical and occupational therapist who specializes in men’s pelvic health. At PHRC, every evaluation begins with a detailed conversation about your health history, previous diagnoses, and the treatments you may have already tried. This allows our team to identify potential underlying causes of your pain and map out a personalized plan of care.
Many men from the Los Angeles area reach out to us after years of frustration and limited progress. Our therapists understand how discouraging that journey can be, which is why they take time to listen carefully and explain every step of your treatment process. We focus on providing a clear, organized plan that gives you direction and confidence.
During your physical examination, your therapist will assess the strength and tone of your pelvic floor muscles, nearby tissues, and joints, while also observing how your movements and posture may contribute to discomfort. Once the evaluation is complete, your therapist will review your findings with you, explain how your pain developed, and help set achievable short- and long-term goals to guide your recovery.

How We Can Help You with Testicular Pain
Men in or near Los Angeles who are struggling with testicular pain that will not subside may benefit from seeking a professional assessment with a pelvic floor physical and occupational therapist who specializes in men’s pelvic health. At PHRC, every evaluation begins with a detailed conversation about your health history, previous diagnoses, and the treatments you may have already tried. This allows our team to identify potential underlying causes of your pain and map out a personalized plan of care.
Many men from the Los Angeles area reach out to us after years of frustration and limited progress. Our therapists understand how discouraging that journey can be, which is why they take time to listen carefully and explain every step of your treatment process. We focus on providing a clear, organized plan that gives you direction and confidence.
During your physical examination, your therapist will assess the strength and tone of your pelvic floor muscles, nearby tissues, and joints, while also observing how your movements and posture may contribute to discomfort. Once the evaluation is complete, your therapist will review your findings with you, explain how your pain developed, and help set achievable short- and long-term goals to guide your recovery.

Most men attend therapy sessions one to two times per week over a span of approximately 12 weeks. Between visits, you will receive customized home exercises to promote faster healing and improved results. Your PHRC therapist will also coordinate with your broader healthcare team, ensuring that your care remains consistent and effective. Our goal is to help you experience genuine relief and restore your quality of life.
