Have you been dealing with persistent testicular pain in Pasadena? Many men are surprised to learn that discomfort in this area is not always caused by a direct injury or infection. In many cases, testicular pain can stem from pelvic floor dysfunction, nerve irritation originating from the lower back, or even circulatory issues that restrict proper blood flow.
Unfortunately, testicular pain is often misdiagnosed as prostatitis, which leads to unnecessary rounds of antibiotics that fail to address the real cause of discomfort. When antibiotics are ineffective, the underlying issue is frequently muscular or neurological rather than bacterial.
Pelvic floor physical and occupational therapy in Pasadena provides a more targeted and effective approach. Through specialized techniques that help restore pelvic floor coordination, strengthen supportive muscles, and improve circulation, these therapies can relieve pain and correct dysfunction over time. Many men find lasting improvement once the root muscular and nerve issues are properly treated.
What are the Causes of Testicular Pain?
There are several potential causes of testicular pain, three of which are related to lumbar pathology, vascular pathology, and pelvic floor pathology.
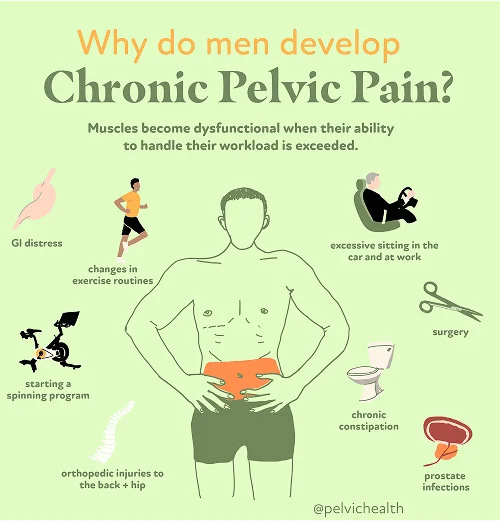
- Lumbar pathology: The nerves that send signals to the testicles originate in the lower portion of the spine. When a disc bulges, arthritis forms, or a lumbar nerve becomes compressed or irritated, the resulting pain can travel downward and feel as though it is coming from the testicle, even though the true source lies within the lower back.
- Vascular pathology: Circulatory problems such as enlarged veins (varicoceles), a twisting of the blood vessels (torsion), or congestion within the veins can all create sensations of heaviness, aching, or sharp pain within the testicular region.
- Pelvic floor pathology: The pelvic floor muscles function as a supportive sling beneath the pelvis. When these muscles become tense, weakened, or begin to spasm, they can irritate nerves that transmit pain signals to the testicle, leading to discomfort that seems internal but actually stems from muscular dysfunction.
Additional causes of testicular pain can include:
- Surgical trauma (vasectomy, benign prostatic hyperplasia (BPH) interventions, prostatectomy)
- Biomechanical or structural dysfunction (hip dysfunction, piriformis syndrome, scoliosis, leg length discrepancy)
- Excessive exercise or changes to exercise routine
- Excessive sitting
- Chronic constipation and straining
- Jelqing and/or attempts at gential enhancement or foreskin regeneration
- In rare cases, bladder, prostate, or sexually transmitted infections after successful resolution of infection
- The majority of men with pelvic pain (including testicular pain), with or without urinary or bowel complaints, have pelvic floor dysfunction
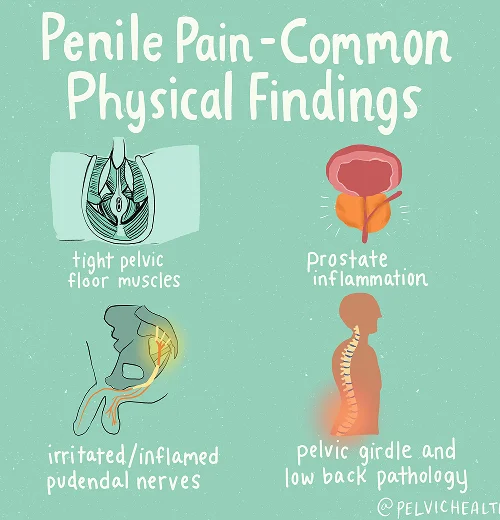

Symptoms of Testicular Pain
- Burning, aching, and itching sensations in the testicles
- These uncomfortable symptoms may also occur in the penis, scrotum, perineal, or anal region
In addition to testicular pain, many men also experience a combination of the below symptoms:
- Men struggling with pelvic pain often notice discomfort when sitting for long periods, engaging in specific types of exercise, or wearing tighter clothing that puts pressure on the pelvic area
- Along with pelvic pain, men may experience urinary urgency, frequency, hesitancy, as well as discomfort and a weaker or slower urinary stream
- During ejaculation, men often feel pain or tightness in the penis, scrotum, or perineum
- Some men may notice erectile dysfunction, including difficulty maintaining an erection or a noticeable decrease in ejaculation strength
- Gastrointestinal distress, bloating, and constipation may also occur
- Symptoms of gastrointestinal discomfort can worsen with physical activity, ejaculation, or sometimes appear without any identifiable trigger
- These symptoms can present either intermittently or persist on a more constant basis
Associated Diagnoses
Lumbar, vascular, and pelvic floor conditions often overlap and contribute to clinically recognised causes of testicular and pelvic pain. Lumbar pathology can present as lumbar radiculopathy or referred pain that originates from disc injuries or degenerative arthritis in the lower back region. Vascular pathology refers to problems such as varicocele, testicular torsion, or pelvic venous congestion, all of which involve impaired or altered blood flow that leads to discomfort and pain. Pelvic floor pathology, on the other hand, is commonly associated with Chronic Pelvic Pain Syndrome (CPPS), pudendal neuralgia, hard flaccid syndrome, and painful bladder syndrome. Frequently, pelvic floor dysfunction serves as the key connection among these conditions, either being the primary cause of the pain or acting as a compounding factor that heightens symptoms from other areas of the body.
Diagnostic Challenges
Many men who experience testicular pain are mistakenly diagnosed with prostatitis and are given antibiotics, even when there is no bacterial infection present. Clinical studies have repeatedly demonstrated that over 90 percent of men who report pelvic or genitourinary discomfort do not actually suffer from bacterial prostatitis.
In reality, the majority of these men fall under the National Institutes of Health (NIH) classifications of Category IIIa or Category IIIb, both of which are part of a broader condition known as Chronic Pelvic Pain Syndrome (CPPS). Additionally, issues originating from the lower back or vascular system can further complicate the picture, as these conditions often mimic the symptoms of pelvic floor dysfunction. This overlap can cause confusion during diagnosis and result in significant delays in identifying the true cause of pain and starting the most appropriate treatment.
The National Institutes of Health recognizes several distinct classifications of prostatitis syndromes:
- Category I: Acute bacterial prostatitis, which presents with intense prostatitis symptoms, signs of systemic infection, and a sudden bacterial urinary tract infection.
- Category II: Chronic bacterial prostatitis, a long-term infection of the prostate that may or may not present noticeable symptoms but is commonly associated with recurrent urinary tract infections caused by the same bacterial strain.
- Category IIIa: Inflammatory chronic pelvic pain syndrome, which is identified by the presence of white blood cells in semen, expressed prostatic secretions, or the third midstream urine sample.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome, where no white blood cells are found in semen or prostatic secretions.
- Category IV: Asymptomatic inflammatory prostatitis, which involves inflammation of the prostate even though the patient does not report any genitourinary symptoms.

The National Institutes of Health recognizes several distinct classifications of prostatitis syndromes:
- Category I: Acute bacterial prostatitis, which presents with intense prostatitis symptoms, signs of systemic infection, and a sudden bacterial urinary tract infection.
- Category II: Chronic bacterial prostatitis, a long-term infection of the prostate that may or may not present noticeable symptoms but is commonly associated with recurrent urinary tract infections caused by the same bacterial strain.
- Category IIIa: Inflammatory chronic pelvic pain syndrome, which is identified by the presence of white blood cells in semen, expressed prostatic secretions, or the third midstream urine sample.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome, where no white blood cells are found in semen or prostatic secretions.
- Category IV: Asymptomatic inflammatory prostatitis, which involves inflammation of the prostate even though the patient does not report any genitourinary symptoms.

Treatment for Testicular Pain
The appropriate treatment for your pain depends on the underlying cause. Whether your discomfort is due to overactive pelvic muscles, nerve irritation, or problems related to circulation, a structured and comprehensive plan can address these contributing factors effectively.
- Pelvic floor physical and occupational therapy for pelvic floor dysfunction: This treatment releases tightness in the muscles, retrains coordination within the pelvic area, and reduces irritation in the nerves to restore comfort and improve daily movement.
- Spine and back treatment: When spinal nerve involvement plays a role, therapy includes physical and occupational work focused on improving posture, strengthening the lower back, and potentially using injections to calm affected nerves.
- Vascular-related treatment: For men experiencing blood flow issues, pelvic floor therapy can promote better circulation by reducing muscular guarding and teaching breathing and posture habits that decrease venous pressure.
- Addressing biomechanical issues: Correcting how the hips, pelvis, and core work together is vital. Therapists use strengthening and mobility exercises to restore balance and reduce mechanical strain that may worsen pain.
- Lifestyle adjustments: Making steady, sustainable changes, such as managing bowel habits, reducing sitting time, and carefully returning to exercise, helps support long-term recovery and prevent flare-ups.
How We Can Help You with Testicular Pain
Men in Pasadena who are struggling with testicular pain can benefit from a comprehensive evaluation with a pelvic floor physical and occupational therapist who specialises in male pelvic pain. At PHRC, your evaluation includes a detailed review of your medical history, symptoms, previous diagnoses, and any prior treatments. The therapist takes time to understand how effective your previous approaches have been and what may still be contributing to your discomfort.
Our Pasadena team understands how discouraging it can be to experience testicular pain that has persisted for months or even years. Many of the men who visit us are frustrated and looking for real, lasting answers after multiple unsuccessful attempts at treatment.

How We Can Help You with Testicular Pain
Men in Pasadena who are struggling with testicular pain can benefit from a comprehensive evaluation with a pelvic floor physical and occupational therapist who specialises in male pelvic pain. At PHRC, your evaluation includes a detailed review of your medical history, symptoms, previous diagnoses, and any prior treatments. The therapist takes time to understand how effective your previous approaches have been and what may still be contributing to your discomfort.
Our Pasadena team understands how discouraging it can be to experience testicular pain that has persisted for months or even years. Many of the men who visit us are frustrated and looking for real, lasting answers after multiple unsuccessful attempts at treatment.

During the physical examination, your therapist assesses your pelvic floor muscles, soft tissues, joints, nerves, and overall movement patterns. Once this evaluation is complete, the therapist will walk you through the findings, explaining how muscular or nerve dysfunction may be linked to your pain. An individualised treatment plan is then created with both short-term and long-term recovery goals.
Typically, pelvic floor physical and occupational therapy sessions are scheduled one to two times each week over a 12-week period. You will also receive a home exercise plan that supports your in-person work, and your therapist will coordinate care with other members of your healthcare team. At PHRC Pasadena, we are committed to helping you heal, restore comfort, and finally find relief from your symptoms.
