If you live in Silverlake and have been struggling with testicular pain, it’s important to understand that the cause may not be what you expect. Many men discover that their pain originates from pelvic floor dysfunction, lower back nerve irritation, or circulation problems within the pelvic region rather than infection.
Because these symptoms can closely mimic prostatitis, men are frequently prescribed antibiotics that fail to deliver any meaningful relief. When the underlying problem is muscular or neurological, antibiotics are ineffective and the discomfort persists.
Pelvic floor physical and occupational therapy in Silverlake offers an evidence-based approach to resolving these issues. Treatment focuses on improving muscular control, reducing nerve sensitivity, and restoring balanced coordination between the pelvic floor and core muscles. This comprehensive method helps relieve testicular pain and supports long-term pelvic health without unnecessary medication.
What are the Causes of Testicular Pain?
There are several potential causes of testicular pain, the most common being associated with lumbar pathology, vascular pathology, and pelvic floor pathology.
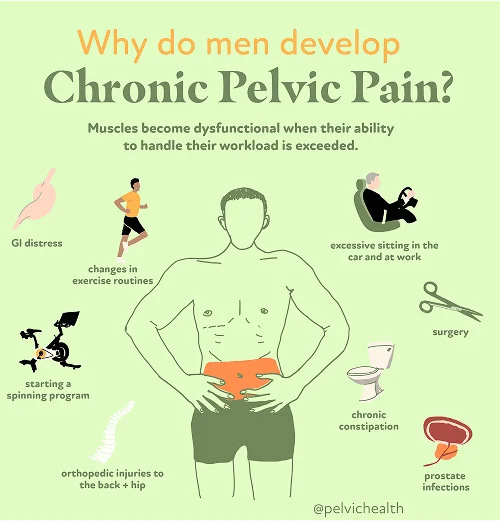
- Lumbar pathology: The nerve roots responsible for testicular sensation stem from the lower spine. When a lumbar disc becomes herniated, arthritis develops, or inflammation irritates a spinal nerve, pain may be perceived in the testicle even though the true source of discomfort is in the back.
- Vascular pathology: Circulation problems such as varicoceles, torsion of the spermatic cord, or pooling of blood within the veins can generate heaviness, aching, or occasional stabbing pain in the testicular area.
- Pelvic floor pathology: The muscles forming the base of the pelvis can tighten, weaken, or spasm, producing irritation of nearby nerves and pain that feels internal but actually stems from dysfunction within the pelvic floor muscles.
Additional causes of testicular pain can include:
- Surgical trauma (vasectomy, benign prostatic hyperplasia (BPH) interventions, prostatectomy)
- Biomechanical or structural dysfunction (hip dysfunction, piriformis syndrome, scoliosis, leg length discrepancy)
- Excessive exercise or changes to exercise routine
- Excessive sitting
- Chronic constipation and straining
- Jelqing and/or attempts at gential enhancement or foreskin regeneration
- In rare cases, bladder, prostate, or sexually transmitted infections after successful resolution of infection
- The majority of men with pelvic pain (including testicular pain), with or without urinary or bowel complaints, have pelvic floor dysfunction
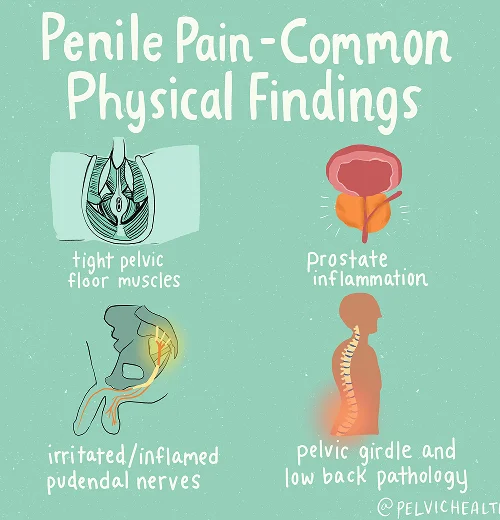

Symptoms of Testicular Pain
- Burning, tingling, or aching pain that affects one or both testicles
- This discomfort may also radiate into the penis, scrotum, perineal area, or around the anus
Alongside testicular pain, men can experience a combination of the following symptoms:
- Pelvic pain that is aggravated by long periods of sitting, vigorous exercise, or wearing snug clothing
- Urinary problems such as urgency, frequency, or a slower and less forceful urinary flow
- Pain or tightness felt in the penis, scrotum, or perineum during ejaculation
- Erectile dysfunction symptoms may occur, along with weaker or less forceful ejaculation
- Some men also experience gastrointestinal discomfort, including constipation, bloating, and cramping
- These gastrointestinal symptoms can be triggered by sexual activity, exercise, or occur on their own
- Men may find these symptoms happen sporadically or persist continuously throughout the day
Associated Diagnoses
Testicular and pelvic pain may result from several interconnected factors involving the lumbar region, vascular circulation, and pelvic floor muscles. Lumbar pathology can manifest as lumbar radiculopathy or as referred discomfort from disc injuries, vertebral joint dysfunction, or arthritis within the lower back. Vascular pathology encompasses disorders such as varicocele, testicular torsion, and pelvic venous congestion, in which restricted or irregular blood flow generates pain sensations. Pelvic floor pathology remains strongly associated with conditions like Chronic Pelvic Pain Syndrome (CPPS), pudendal neuralgia, hard flaccid syndrome, and painful bladder syndrome. In many cases, pelvic floor dysfunction serves as the unifying factor that contributes to or intensifies the pain experience, either by directly triggering symptoms or by sensitising the body to pain from other underlying disorders.
Diagnostic Challenges
When men report testicular pain, they are often misdiagnosed with prostatitis and placed on antibiotic treatment, even though laboratory findings may not indicate an active infection. Current research suggests that over 90 percent of men with pelvic or genitourinary discomfort are not suffering from bacterial prostatitis.
Instead, most fall within Category IIIa or Category IIIb of the National Institutes of Health classification, conditions grouped together as Chronic Pelvic Pain Syndrome (CPPS). At the same time, pain originating from the lower spine or circulatory system can mimic pelvic floor dysfunction, creating diagnostic confusion. This overlap can delay accurate identification of the true cause and prevent men from receiving timely, effective treatment.
According to the National Institutes of Health, prostatitis is categorized as follows:
- Category I: Acute bacterial prostatitis, typically characterized by severe pelvic pain, systemic infection, and a bacterial urinary tract infection.
- Category II: Chronic bacterial prostatitis, resulting from persistent bacterial infection in the prostate and often linked to repeated urinary infections caused by the same bacterial strain.
- Category IIIa: Inflammatory chronic pelvic pain syndrome, diagnosed when white blood cells are present in semen, expressed prostatic fluid, or the third urine sample.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome, which does not show any white blood cells in the aforementioned samples.
- Category IV: Asymptomatic inflammatory prostatitis, defined by the presence of inflammation in the prostate despite the absence of any urinary or pelvic pain symptoms.

According to the National Institutes of Health, prostatitis is categorized as follows:
- Category I: Acute bacterial prostatitis, typically characterized by severe pelvic pain, systemic infection, and a bacterial urinary tract infection.
- Category II: Chronic bacterial prostatitis, resulting from persistent bacterial infection in the prostate and often linked to repeated urinary infections caused by the same bacterial strain.
- Category IIIa: Inflammatory chronic pelvic pain syndrome, diagnosed when white blood cells are present in semen, expressed prostatic fluid, or the third urine sample.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome, which does not show any white blood cells in the aforementioned samples.
- Category IV: Asymptomatic inflammatory prostatitis, defined by the presence of inflammation in the prostate despite the absence of any urinary or pelvic pain symptoms.

Treatment for Testicular Pain
The right course of treatment depends on what is driving your symptoms. The source may be tight pelvic floor muscles, irritated nerves, or restricted blood flow affecting the pelvic area. A tailored plan will combine the most effective therapies for your specific condition.
- Pelvic floor physical and occupational therapy for pelvic floor dysfunction: This approach targets muscle relaxation and retraining. It helps to restore proper pelvic coordination and alleviate nerve irritation that often accompanies chronic pain.
- Spine and back treatment: If lumbar spine issues are responsible for your testicular discomfort, treatment may involve therapy focused on spinal stability, postural adjustments, and when necessary, medical interventions such as injections to reduce inflammation.
- Vascular-related treatment: When blood flow is limited, pelvic floor physical and occupational therapy can ease tension, improve circulation through breathing exercises and posture correction, and relieve pressure from congested veins.
- Addressing biomechanical issues: Therapy may also focus on improving hip alignment, joint movement, and muscular balance to reduce strain caused by structural imbalances or restricted mobility.
- Lifestyle adjustments: Managing daily habits, such as preventing constipation, avoiding extended periods of sitting, and gradually reintroducing physical exercise, can also help reduce strain and maintain pelvic health.
How We Can Help You with Testicular Pain
Men in Silverlake who have been coping with persistent testicular pain can benefit from an in-depth evaluation with a pelvic floor physical and occupational therapist at PHRC. During your appointment, your therapist will discuss your symptoms, review your medical history, and assess what treatments you’ve already tried. This helps determine which factors are still influencing your discomfort and how to target them more effectively.
We recognise that many Silverlake men come to PHRC after long periods of frustration and uncertainty. Our therapists understand your situation and strive to create a supportive and empathetic environment where you finally feel heard.
Your physical evaluation involves analysing the muscles, tissues, joints, and nerves that make up the pelvic region, as well as how your body moves and compensates for pain. After completing the exam, your therapist will share the findings, explain the likely causes of your pain, and set out clear goals for your recovery plan. Both short-term symptom relief and long-term improvement are prioritised.

How We Can Help You with Testicular Pain
Men in Silverlake who have been coping with persistent testicular pain can benefit from an in-depth evaluation with a pelvic floor physical and occupational therapist at PHRC. During your appointment, your therapist will discuss your symptoms, review your medical history, and assess what treatments you’ve already tried. This helps determine which factors are still influencing your discomfort and how to target them more effectively.
We recognise that many Silverlake men come to PHRC after long periods of frustration and uncertainty. Our therapists understand your situation and strive to create a supportive and empathetic environment where you finally feel heard.
Your physical evaluation involves analysing the muscles, tissues, joints, and nerves that make up the pelvic region, as well as how your body moves and compensates for pain. After completing the exam, your therapist will share the findings, explain the likely causes of your pain, and set out clear goals for your recovery plan. Both short-term symptom relief and long-term improvement are prioritised.

Most clients in Silverlake attend one to two therapy sessions per week for around 12 weeks. A personalised exercise plan is given to continue your progress at home, and your therapist ensures that your care is well-coordinated with other healthcare professionals. The PHRC Silverlake team is dedicated to helping you regain comfort, control, and peace of mind.
