Are you in Agoura Hills and finding it difficult to get rid of persistent testicular pain? While infections are often suspected first, the root cause may actually lie elsewhere. Common contributors include pelvic floor dysfunction, nerve irritation in the lower spine, or reduced pelvic blood flow, all of which can create pain that feels deep and ongoing.
Because the symptoms are similar to prostatitis, testicular pain is frequently misdiagnosed. This often leads to antibiotic treatments that fail to bring improvement. When medication does not help, the actual issue may be muscular or nerve-related rather than infectious.
For those searching from Agoura Hills or nearby communities, pelvic floor physical and occupational therapy offer an effective, non-surgical path to recovery. These therapies help relax tight muscles, improve pelvic alignment, and decrease pressure on nerves. By focusing on the true cause, this approach encourages lasting relief and improved function.
What are the Causes of Testicular Pain?
Testicular pain is not always the result of direct testicular injury or infection. It can emerge from conditions affecting the spine, blood vessels, or pelvic muscles.
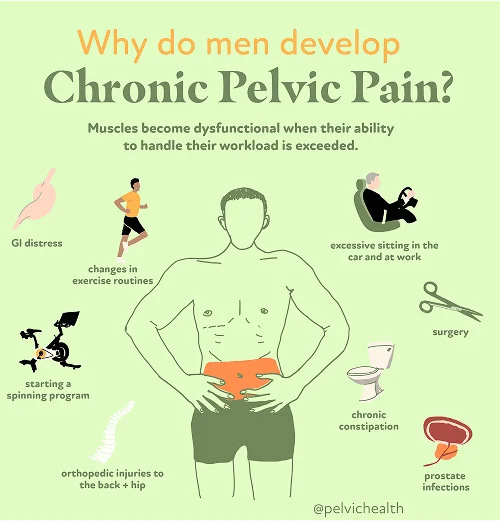
- Lumbar pathology: Since the nerves serving the testicles are anchored in the lumbar spine, any problem such as a slipped disc, osteoarthritis, or nerve inflammation in this region can send referred pain signals to the scrotum. The discomfort may therefore seem to arise from the testicle despite beginning in the lower back.
- Vascular pathology: When blood circulation through the testicular veins becomes restricted or irregular, issues like varicocele, torsion, or venous congestion can develop. These can produce heaviness, aching, or sharp bouts of pain depending on the severity of the vascular involvement.
- Pelvic floor pathology: The pelvic floor’s interconnected network of muscles provides foundational stability for the pelvis. Tension, weakness, or spasms within these muscles can irritate local nerves, sending referred sensations to the testicle even though the pain’s origin is muscular.
Additional causes of testicular pain can include:
- Surgical trauma (vasectomy, benign prostatic hyperplasia (BPH) interventions, prostatectomy)
- Biomechanical or structural dysfunction (hip dysfunction, piriformis syndrome, scoliosis, leg length discrepancy)
- Excessive exercise or changes to exercise routine
- Excessive sitting
- Chronic constipation and straining
- Jelqing and/or attempts at gential enhancement or foreskin regeneration
- In rare cases, bladder, prostate, or sexually transmitted infections after successful resolution of infection
- The majority of men with pelvic pain (including testicular pain), with or without urinary or bowel complaints, have pelvic floor dysfunction
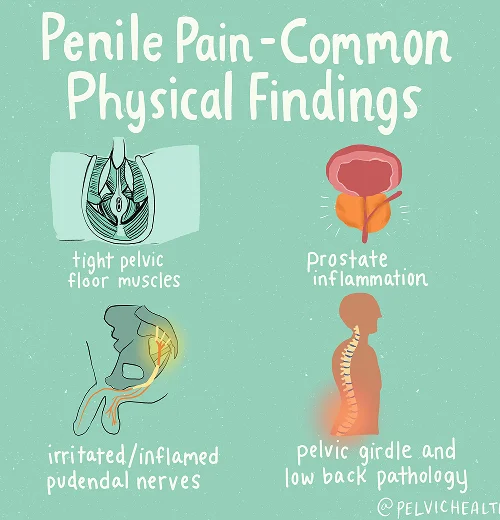

Symptoms of Testicular Pain
- Pain in the testicles may present as a burning, shooting, or cramping sensation that interferes with comfort and daily activities.
- The discomfort can radiate to adjacent areas including the penis, perineum, anus, and lower abdomen, creating a diffuse pelvic ache.
Men dealing with such pain often experience several secondary symptoms:
- Pelvic tension tends to become worse after long periods of sitting, physical exercise, or while wearing constrictive clothing.
- Frequent or urgent urination, as well as a weaker urinary stream, often accompany the condition.
- Pain during ejaculation is another characteristic symptom, sometimes felt in the penis or perineum.
- Reduced erectile function or diminished ejaculation strength may occur in conjunction with ongoing pelvic discomfort.
- Digestive issues such as constipation, fullness, or abdominal bloating frequently accompany these symptoms.
- Flare-ups of digestive distress may occur after ejaculation, workouts, or without any identifiable cause.
- The pain may fluctuate in severity, with some days significantly worse than others.
Associated Diagnoses
Testicular and pelvic pain frequently result from overlapping problems involving the lumbar spine, vascular system, and pelvic floor, all of which can interact in complex ways. Lumbar disorders, including herniated discs, arthritis, or nerve compression, often cause referred pain into the pelvic region. Vascular issues such as varicocele, testicular torsion, and pelvic venous congestion disrupt circulation and cause heaviness or aching sensations. Pelvic floor dysfunction is commonly intertwined with these issues and has known associations with Chronic Pelvic Pain Syndrome (CPPS), pudendal neuralgia, painful bladder syndrome, and hard flaccid syndrome. For many individuals, this dysfunction becomes the central mechanism that sustains or magnifies pain generated by surrounding anatomical problems.
Diagnostic Challenges
For many men, testicular pain is a recurring issue, yet it is commonly mistaken for prostatitis. This often leads to unnecessary prescriptions of antibiotics even though laboratory tests reveal no evidence of a bacterial cause. Clinical research repeatedly indicates that more than 90 percent of men who experience ongoing pelvic or genital pain do not have a bacterial infection of the prostate gland.
A significant number of these individuals fall into the National Institutes of Health categories known as IIIa and IIIb, both of which make up Chronic Pelvic Pain Syndrome (CPPS). Sometimes the discomfort is compounded by nerve irritation in the lower back or by poor blood circulation, both of which can imitate the sensations of pelvic floor dysfunction and complicate an accurate medical assessment.
According to data from the National Institutes of Health, prostatitis and its variations are grouped into the following categories:
- Category I:Acute bacterial prostatitis is characterized by intense pelvic pain, high fever, and urinary problems resulting from bacterial infection within the prostate.
- Category II: Chronic bacterial prostatitis represents a recurring infection that continues to cause discomfort and repeated urinary infections tied to one bacterial strain.
- Category IIIa: Inflammatory chronic pelvic pain syndrome demonstrates immune activity through the presence of white blood cells in semen or other prostate-related samples.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome brings ongoing pain yet does not reveal any white blood cells upon analysis.
- Category IV: Asymptomatic inflammatory prostatitis signifies inflammation that exists without any external symptoms or awareness by the patient.

According to data from the National Institutes of Health, prostatitis and its variations are grouped into the following categories:
- Category I:Acute bacterial prostatitis is characterized by intense pelvic pain, high fever, and urinary problems resulting from bacterial infection within the prostate.
- Category II: Chronic bacterial prostatitis represents a recurring infection that continues to cause discomfort and repeated urinary infections tied to one bacterial strain.
- Category IIIa: Inflammatory chronic pelvic pain syndrome demonstrates immune activity through the presence of white blood cells in semen or other prostate-related samples.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome brings ongoing pain yet does not reveal any white blood cells upon analysis.
- Category IV: Asymptomatic inflammatory prostatitis signifies inflammation that exists without any external symptoms or awareness by the patient.

Treatment for Testicular Pain
Depending on what contributes most to your discomfort, whether it is tightness in the pelvic floor, irritation of nerves branching from the lower back, or decreased blood circulation to key tissues, your therapist may suggest a comprehensive program that blends various forms of treatment to restore healthy pelvic function. These interventions aim to reduce tension, enhance stability, and encourage proper movement patterns.
- Pelvic floor physical and occupational therapy for pelvic floor dysfunction: Designed to calm overactive muscles and promote relaxation, this therapy targets both the muscular and nerve components of pelvic pain. By enhancing coordination between the pelvic floor and core, patients experience improved control and noticeable pain reduction over time.
- Spine and back treatment: When nerve compression in the lower back contributes to pelvic discomfort, treatment will focus on spinal mobility, strength, and alignment. Targeted therapy and posture training can relieve pressure on affected nerves, while guided injections may reduce lingering inflammation.
- Vascular-related treatment: If limited blood flow is contributing to your pain, pelvic therapy aims to ease tightness, stimulate circulation, and alleviate pressure in congested pelvic veins through proper posture and breathing control. Improved blood movement supports tissue healing.
- Addressing biomechanical issues: Restricted hip or pelvic movement can put strain on surrounding muscles. Corrective exercises, mobility drills, and manual techniques are used to restore alignment, increase flexibility, and minimize unnecessary pelvic tension.
- Lifestyle adjustments: Modifications often include minimizing prolonged sitting, maintaining healthy bowel habits, and engaging in gradual movement routines. These adjustments reduce irritation and help prevent future flare-ups.
How We Can Help You with Testicular Pain
If you are from the Agoura Hills area and are struggling with testicular pain that will not fade, it may be time to meet with a pelvic floor physical and occupational therapist who specializes in men’s pelvic health. PHRC begins each consultation with a complete review of your medical background, previous diagnoses, and symptom history. This process allows our clinicians to identify underlying factors contributing to your discomfort and to determine the most effective treatment path forward.
We frequently work with men in Agoura Hills who feel frustrated after years of limited results. Our team focuses on empathy, communication, and education, taking time to build a clear and achievable treatment plan that restores confidence and understanding.
During your assessment, your therapist examines muscle tone, pelvic alignment, and nerve sensitivity, and observes how specific movement patterns may contribute to pain. Once the evaluation is complete, you will discuss your results in detail, learn about the causes of your pain, and set goals for recovery.

How We Can Help You with Testicular Pain
If you are from the Agoura Hills area and are struggling with testicular pain that will not fade, it may be time to meet with a pelvic floor physical and occupational therapist who specializes in men’s pelvic health. PHRC begins each consultation with a complete review of your medical background, previous diagnoses, and symptom history. This process allows our clinicians to identify underlying factors contributing to your discomfort and to determine the most effective treatment path forward.
We frequently work with men in Agoura Hills who feel frustrated after years of limited results. Our team focuses on empathy, communication, and education, taking time to build a clear and achievable treatment plan that restores confidence and understanding.
During your assessment, your therapist examines muscle tone, pelvic alignment, and nerve sensitivity, and observes how specific movement patterns may contribute to pain. Once the evaluation is complete, you will discuss your results in detail, learn about the causes of your pain, and set goals for recovery.

Therapy sessions usually take place one to two times each week over the course of about three months. Between sessions, you will be given simple home exercises to maintain progress. Your PHRC therapist will collaborate closely with your healthcare providers to ensure a unified treatment approach. Our goal is to help you finally experience comfort and a renewed sense of well-being.
