Are you someone in or around Calabasas who has been bothered by testicular pain that refuses to fade? While infection might seem like the likely cause, discomfort in this area is often linked to other problems such as pelvic floor dysfunction, irritated nerves in the lower back, or poor circulation within the pelvic region.
Because the symptoms are similar to prostatitis, misdiagnosis is common. This often leads to unnecessary rounds of antibiotics that fail to help. When medication proves ineffective, it usually suggests that the pain is being caused by muscular or nerve-related issues.
Residents in Calabasas and nearby communities may find that pelvic floor physical and occupational therapy provide significant relief. These therapies focus on muscle relaxation, improved coordination, and nerve decompression. By treating the source rather than the symptom, men can experience long-term healing and restored comfort.
What are the Causes of Testicular Pain?
There are multiple possible explanations for the onset of testicular pain, many of which involve the lumbar spine, vascular circulation, or the pelvic floor muscles.
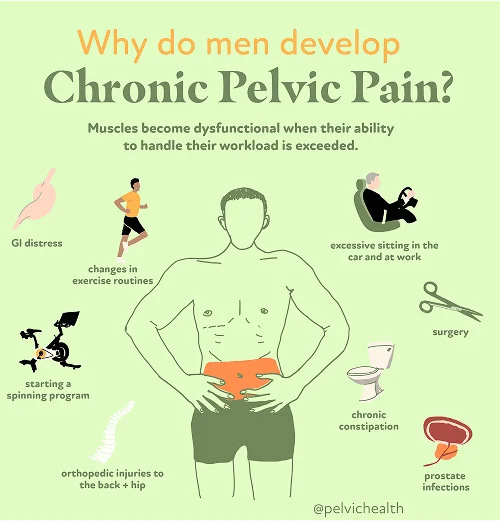
- Lumbar pathology: The nerves that extend into the testicles begin their course within the lower spine. When that area becomes irritated from conditions like spinal arthritis, nerve compression, or disc herniation, pain may radiate along the nerve pathways into the testicular region.
- Vascular pathology: Disruption in normal venous return can cause pressure or pooling within the testicular veins. This may result from conditions such as varicocele, torsion, or vascular congestion, all of which create sensations of aching or heaviness in the groin.
- Pelvic floor pathology: The pelvic floor consists of an intricate network of muscles that maintain stability for pelvic organs. When these muscles tighten or spasm excessively, they can place strain on adjacent nerves, producing referred pain that feels as if it originates from the testicle itself.
Additional causes of testicular pain can include:
- Surgical trauma (vasectomy, benign prostatic hyperplasia (BPH) interventions, prostatectomy)
- Biomechanical or structural dysfunction (hip dysfunction, piriformis syndrome, scoliosis, leg length discrepancy)
- Excessive exercise or changes to exercise routine
- Excessive sitting
- Chronic constipation and straining
- Jelqing and/or attempts at gential enhancement or foreskin regeneration
- In rare cases, bladder, prostate, or sexually transmitted infections after successful resolution of infection
- The majority of men with pelvic pain (including testicular pain), with or without urinary or bowel complaints, have pelvic floor dysfunction
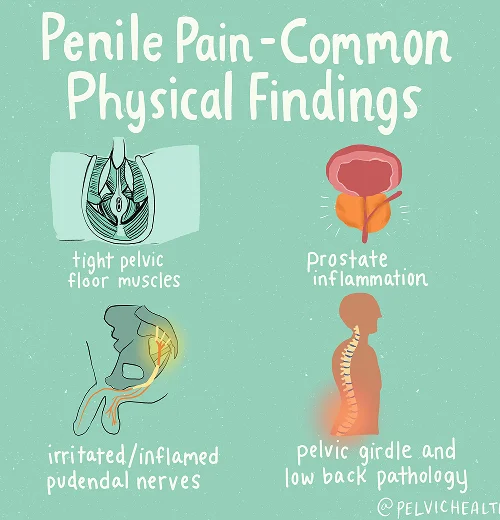

Symptoms of Testicular Pain
- The pain experienced in the testicles may feel sharp, burning, or deeply throbbing and can spread into adjacent areas.
- These sensations sometimes move toward the penis, perineum, anus, or groin.
Men suffering from these symptoms often describe related issues such as:
- Increased pelvic discomfort after sitting too long, engaging in physical work, or wearing tight clothing.
- Changes in urination including more frequent trips, urgency, and a weaker flow.
- Painful or uncomfortable sensations during ejaculation, which may affect the perineum or penis.
- Some individuals also report erectile problems or weaker ejaculation force.
- Digestive complaints such as constipation or bloating often appear simultaneously.
- These symptoms can worsen without clear triggers or follow activity and sexual release.
- Intensity varies, with flare-ups alternating with brief periods of relief.
Associated Diagnoses
The causes of testicular and pelvic pain are often interconnected, involving a mix of lumbar spine, vascular, and pelvic floor dysfunctions. Lumbar pathology may include lumbar radiculopathy or referred discomfort that stems from degenerative disc disease, arthritis, or vertebral compression. Vascular complications such as varicocele, testicular torsion, and pelvic venous congestion impede blood flow and contribute to persistent or throbbing pelvic pain. Pelvic floor pathology frequently overlaps with these conditions and is associated with Chronic Pelvic Pain Syndrome (CPPS), pudendal neuralgia, hard flaccid syndrome, and painful bladder syndrome. In many patients, dysfunction in the pelvic floor muscles becomes the central factor that maintains or amplifies discomfort produced by other structural or circulatory issues.
Diagnostic Challenges
Many men report testicular discomfort that is incorrectly attributed to prostatitis, often resulting in the use of antibiotics that are not required. In most of these cases, testing confirms that no bacterial infection exists. Medical literature has shown that more than 90 percent of men with chronic pelvic or genital pain do not actually suffer from a bacterial infection within the prostate gland.
The majority of these cases fall under the National Institutes of Health’s Category IIIa and Category IIIb designations, collectively referred to as Chronic Pelvic Pain Syndrome (CPPS). Nerve irritation from the lower spine and reduced pelvic blood flow can both mimic the same pain patterns as pelvic floor dysfunction, leading to confusion and delays in treatment.
In accordance with the National Institutes of Health’s definitions, prostatitis syndromes are grouped as follows:
- Category I: Acute bacterial prostatitis results from an immediate bacterial infection that produces intense pelvic pain, fever, and urinary difficulties.
- Category II: Chronic bacterial prostatitis involves a recurring infection within the prostate, leading to repeated urinary tract infections by the same organism.
- Category IIIa: Inflammatory chronic pelvic pain syndrome displays an immune response, marked by the presence of white blood cells in prostate-related fluids or urine samples.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome includes similar symptoms but lacks white blood cells, suggesting irritation without infection.
- Category IV: Asymptomatic inflammatory prostatitis refers to inflammation within the prostate that exists silently without discomfort or urinary complaints.

In accordance with the National Institutes of Health’s definitions, prostatitis syndromes are grouped as follows:
- Category I: Acute bacterial prostatitis results from an immediate bacterial infection that produces intense pelvic pain, fever, and urinary difficulties.
- Category II: Chronic bacterial prostatitis involves a recurring infection within the prostate, leading to repeated urinary tract infections by the same organism.
- Category IIIa: Inflammatory chronic pelvic pain syndrome displays an immune response, marked by the presence of white blood cells in prostate-related fluids or urine samples.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome includes similar symptoms but lacks white blood cells, suggesting irritation without infection.
- Category IV: Asymptomatic inflammatory prostatitis refers to inflammation within the prostate that exists silently without discomfort or urinary complaints.

Treatment for Testicular Pain
Depending on what is truly behind your symptoms, whether related to tight pelvic floor muscles, irritation of nerves that travel through the lower back, or reduced blood circulation in the pelvis, your care plan may consist of multiple therapeutic strategies aimed at rebalancing muscle tone and optimizing pelvic function. These therapies help promote circulation, relieve tension, and improve how the body supports the pelvic organs.
- Pelvic floor physical and occupational therapy for pelvic floor dysfunction: This therapy emphasizes calming the pelvic muscles, retraining them for proper movement, and reducing nerve hypersensitivity. Over time, consistent treatment restores strength, coordination, and overall comfort.
- Spine and back treatment: When the root cause of your pain lies within the lower spine, therapy often includes spinal mobilization, postural correction, and core stabilization. Occasionally, guided injections are added to control inflammation around compressed nerves.
- Vascular-related treatment: Poor circulation can make pain worse, so therapy often targets improved breathing patterns, muscle relaxation, and upright posture to help oxygenate tissues and ease venous congestion.
- Addressing biomechanical issues: When misalignment limits movement in your hips or pelvis, corrective exercises and manual adjustments improve joint mobility, enhance posture, and decrease strain on nearby muscles.
- Lifestyle adjustments: Therapists may guide you in breaking long sitting habits, improving digestive function, and gradually reintroducing physical activity to maintain your progress between sessions.
How We Can Help You with Testicular Pain
If you are from Calabasas and searching for solutions to ongoing testicular pain, a pelvic floor physical and occupational therapist may provide the expertise you need. At PHRC, our process begins with an in-depth evaluation of your medical history, prior diagnoses, and previous treatments. This detailed conversation allows us to understand your experience and identify what may be driving your pain.
Many men in the Calabasas community come to us after years of frustration, having tried medications or procedures that did not bring relief. Our therapists are known for their empathy and commitment to providing clarity, ensuring that each client leaves the first appointment with a sense of direction and renewed hope.
During your physical exam, your therapist assesses pelvic floor strength, flexibility, and nerve sensitivity, while also studying how your body moves during daily activities. Once this evaluation is complete, your therapist reviews the findings, explains what may be contributing to your symptoms, and helps establish short- and long-term recovery goals.

How We Can Help You with Testicular Pain
If you are from Calabasas and searching for solutions to ongoing testicular pain, a pelvic floor physical and occupational therapist may provide the expertise you need. At PHRC, our process begins with an in-depth evaluation of your medical history, prior diagnoses, and previous treatments. This detailed conversation allows us to understand your experience and identify what may be driving your pain.
Many men in the Calabasas community come to us after years of frustration, having tried medications or procedures that did not bring relief. Our therapists are known for their empathy and commitment to providing clarity, ensuring that each client leaves the first appointment with a sense of direction and renewed hope.
During your physical exam, your therapist assesses pelvic floor strength, flexibility, and nerve sensitivity, while also studying how your body moves during daily activities. Once this evaluation is complete, your therapist reviews the findings, explains what may be contributing to your symptoms, and helps establish short- and long-term recovery goals.

Treatment is typically scheduled one to two times per week for about 12 weeks, supported by customized home exercises. Your PHRC therapist maintains open communication with your medical team to keep care consistent and coordinated. Our mission is to guide you toward long-lasting relief and a better quality of life.
