Have you been experiencing unexplained testicular discomfort in Los Feliz? Many men don’t realise that this type of pain can stem from pelvic floor dysfunction, nerve compression in the lower back, or circulatory disturbances that affect the pelvic region. It isn’t always the result of an infection, though it is frequently mistaken for one.
In fact, testicular pain is commonly misdiagnosed as prostatitis, leading to the overuse of antibiotics that do not target the actual source of the problem. When antibiotics fail to bring relief, it often indicates that the pain is related to muscular tension or nerve irritation rather than bacteria.
Pelvic floor physical and occupational therapy in Los Feliz can help address these deeper causes. By restoring muscle coordination, reducing tension, and enhancing blood flow to the pelvic area, therapy works to correct dysfunction and eliminate discomfort. Over time, men often experience marked improvement and a better quality of life with consistent, targeted treatment.
What are the Causes of Testicular Pain?
There are several potential causes of testicular pain, particularly those involving lumbar pathology, vascular pathology, and pelvic floor pathology.
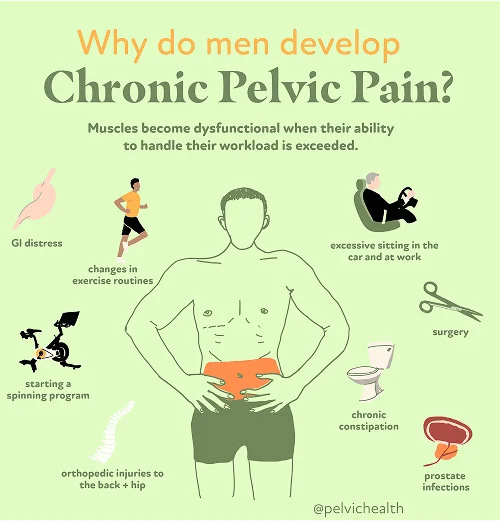
- Lumbar pathology: Nerves traveling from the lower spine to the testicles can transmit pain when a disc herniates, arthritis forms, or inflammation compresses the nerve. This results in referred pain that feels like it originates from the testicle even though the issue is within the back.
- Vascular pathology: Blood circulation problems such as enlarged veins (varicoceles), twisted blood supply (torsion), or vascular congestion can create persistent aching, pressure, or sharp pain in the testicles due to impaired blood flow.
- Pelvic floor pathology: The pelvic floor muscles support the organs in the pelvis like a sling. When these muscles become tense, weakened, or spasm, they can compress nerves and cause sensations that mimic testicular pain, even though the root cause lies in the muscles themselves.
Additional causes of testicular pain can include:
- Surgical trauma (vasectomy, benign prostatic hyperplasia (BPH) interventions, prostatectomy)
- Biomechanical or structural dysfunction (hip dysfunction, piriformis syndrome, scoliosis, leg length discrepancy)
- Excessive exercise or changes to exercise routine
- Excessive sitting
- Chronic constipation and straining
- Jelqing and/or attempts at gential enhancement or foreskin regeneration
- In rare cases, bladder, prostate, or sexually transmitted infections after successful resolution of infection
- The majority of men with pelvic pain (including testicular pain), with or without urinary or bowel complaints, have pelvic floor dysfunction
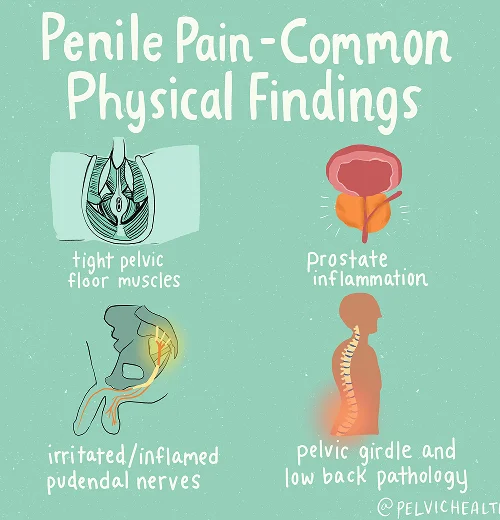

Symptoms of Testicular Pain
- Burning, aching, or a dull throbbing sensation in the testicles
- This discomfort may also affect nearby areas such as the penis, scrotum, perineal region, and anal area
In addition to testicular pain, men frequently experience other related symptoms:
- Pelvic pain that increases with sitting, after certain workouts, or when wearing tight clothing
- Urinary symptoms may include urgency, frequency, hesitancy, and a noticeably weaker or slower stream
- Pain or pressure in the penis, scrotum, or perineum can occur during ejaculation
- Erectile issues may also arise, such as difficulty maintaining an erection or a reduction in ejaculation power
- Digestive complaints including bloating, constipation, or abdominal discomfort may also be present
- These gastrointestinal symptoms might be triggered by ejaculation, physical exertion, or arise unexpectedly
- The symptoms can appear intermittently or remain constant over time
Associated Diagnoses
When examining the sources of testicular and pelvic pain, lumbar, vascular, and pelvic floor abnormalities often emerge as interconnected contributors. Lumbar pathology frequently appears as lumbar radiculopathy or referred pain from degenerative disc disease and lower spinal arthritis. Vascular pathology encompasses issues like varicocele, testicular torsion, and pelvic venous congestion, where compromised circulation leads to discomfort and persistent aching sensations. Pelvic floor pathology is most notably associated with Chronic Pelvic Pain Syndrome (CPPS), pudendal neuralgia, hard flaccid syndrome, and painful bladder syndrome. Often, pelvic floor dysfunction plays a pivotal role by linking these conditions together, functioning as a central cause of pain or as a factor that amplifies the severity of symptoms originating from the lumbar spine or vascular system.
Diagnostic Challenges
Many men who experience chronic testicular discomfort are incorrectly told they have prostatitis and are treated with antibiotics, even when no signs of infection are found. Scientific studies confirm that more than 90 percent of men experiencing pelvic or genital pain symptoms do not actually have bacterial prostatitis.
These individuals often belong to the National Institutes of Health classifications of Category IIIa and Category IIIb, which are collectively identified as Chronic Pelvic Pain Syndrome (CPPS). At the same time, lower back and vascular problems can create pain patterns similar to pelvic floor dysfunction, making diagnosis more complex and sometimes delaying the start of effective care.
The National Institutes of Health categorizes prostatitis syndromes as follows:
- Category I: Acute bacterial prostatitis, associated with sudden onset of severe symptoms, systemic infection, and bacterial urinary tract infection.
- Category II: Chronic bacterial prostatitis, which develops from long-term bacterial infection in the prostate and may include recurring urinary tract infections caused by the same strain.
- Category IIIa: Inflammatory chronic pelvic pain syndrome, recognized by the detection of white blood cells in semen, expressed prostatic fluid, or the third portion of a midstream urine sample.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome, where white blood cells are not present in these samples.
- Category IV: Asymptomatic inflammatory prostatitis, involving prostate inflammation with no accompanying genitourinary symptoms.

The National Institutes of Health categorizes prostatitis syndromes as follows:
- Category I: Acute bacterial prostatitis, associated with sudden onset of severe symptoms, systemic infection, and bacterial urinary tract infection.
- Category II: Chronic bacterial prostatitis, which develops from long-term bacterial infection in the prostate and may include recurring urinary tract infections caused by the same strain.
- Category IIIa: Inflammatory chronic pelvic pain syndrome, recognized by the detection of white blood cells in semen, expressed prostatic fluid, or the third portion of a midstream urine sample.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome, where white blood cells are not present in these samples.
- Category IV: Asymptomatic inflammatory prostatitis, involving prostate inflammation with no accompanying genitourinary symptoms.

Treatment for Testicular Pain
Your treatment approach will depend largely on what is causing your symptoms. For some men, this may involve overly tight or hyperactive pelvic floor muscles, for others, it may be due to irritated nerves or issues with blood circulation in the pelvic area.
- Pelvic floor physical and occupational therapy for pelvic floor dysfunction: This form of care helps release tight or overworked muscles, retrains the way the pelvic floor coordinates with other muscle groups, and reduces irritation affecting the pelvic nerves.
- Spine and back treatment: When nerve compression or irritation in the lower spine contributes to pain, therapy often includes physical and occupational techniques, posture correction, and in certain cases, image-guided injections to relieve pressure on affected nerves.
- Vascular-related treatment: If blood flow problems are a factor, therapy can help reduce muscle tension and improve circulation through focused posture and breathing exercises, which together relieve congestion in the pelvic veins.
- Addressing biomechanical issues: Correcting the way the hips and pelvis move is also essential. Exercises and manual therapy can improve strength and mobility, restoring proper body mechanics when misalignment plays a role.
- Lifestyle adjustments: This can involve adopting bowel management techniques to prevent constipation, taking breaks from prolonged sitting, and safely resuming workouts to promote long-term pelvic stability.
How We Can Help You with Testicular Pain
Men in Los Feliz struggling with testicular pain should consider consulting a pelvic floor physical and occupational therapist who focuses on treating male pelvic health conditions. At PHRC, your initial evaluation covers your full medical history, including your symptoms, previous diagnoses, and all prior treatments to determine what has helped and what has not. This detailed review allows your therapist to create a precise and targeted plan of care.
We understand that by the time you reach us, the frustration can be overwhelming. Many men in Los Feliz have seen multiple providers before finding answers, and we take pride in offering the professional insight and compassion they have been seeking.
During your physical examination, your therapist evaluates the strength, flexibility, and function of the pelvic floor muscles, along with nearby tissues, nerves, and joints. After reviewing your results, your therapist will explain how dysfunction developed and establish measurable goals for your progress. Both immediate relief and sustainable results are key priorities in your plan.

How We Can Help You with Testicular Pain
Men in Los Feliz struggling with testicular pain should consider consulting a pelvic floor physical and occupational therapist who focuses on treating male pelvic health conditions. At PHRC, your initial evaluation covers your full medical history, including your symptoms, previous diagnoses, and all prior treatments to determine what has helped and what has not. This detailed review allows your therapist to create a precise and targeted plan of care.
We understand that by the time you reach us, the frustration can be overwhelming. Many men in Los Feliz have seen multiple providers before finding answers, and we take pride in offering the professional insight and compassion they have been seeking.
During your physical examination, your therapist evaluates the strength, flexibility, and function of the pelvic floor muscles, along with nearby tissues, nerves, and joints. After reviewing your results, your therapist will explain how dysfunction developed and establish measurable goals for your progress. Both immediate relief and sustainable results are key priorities in your plan.

The average treatment schedule includes one to two sessions each week for approximately 12 weeks. You’ll also receive a home exercise plan that reinforces what you learn during therapy. PHRC Los Feliz coordinates your recovery journey with your other healthcare providers to ensure that you receive consistent, well-rounded care.
