If you are in Oceanside and dealing with ongoing testicular pain that has not improved, it may surprise you to learn that infections are not always responsible. Many men experience discomfort caused by pelvic floor dysfunction, nerve irritation from the lower spine, or restricted pelvic circulation.
Because these symptoms mirror prostatitis, it is common for men to be misdiagnosed and treated with antibiotics that do not provide lasting relief. When medication fails to work, the issue is often muscular or neurological instead of bacterial.
Men throughout Oceanside who are seeking relief may find that pelvic floor physical and occupational therapy is a smart solution. These treatments aim to relax overactive muscles, restore proper movement patterns, and relieve pressure on nerves. By focusing on the underlying issue, this approach promotes true and lasting comfort.
What are the Causes of Testicular Pain?
Testicular pain can arise from several underlying factors that commonly involve the lumbar spine, the vascular system, or the pelvic floor.
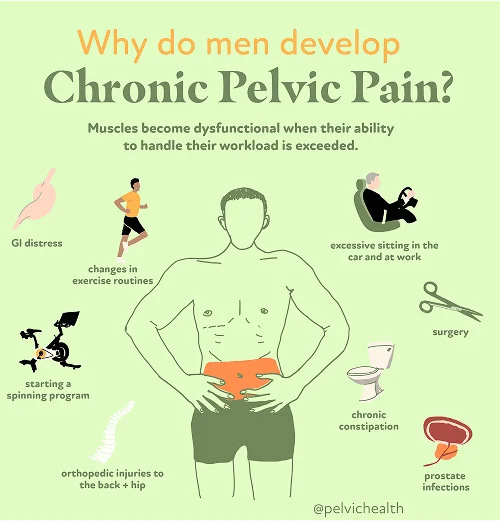
- Lumbar pathology: The nerve roots that connect to the testicles stem from the lower segments of the spine. When a condition such as lumbar arthritis, disc herniation, or nerve impingement occurs, it can send pain signals along these neural pathways. The result is referred pain that appears to come from the testicle despite beginning in the back.
- Vascular pathology: Circulatory problems like varicoceles, torsion of the testicular structures, or venous congestion interrupt normal blood flow. This disturbance can cause persistent aching, heaviness, or at times sudden, severe pain in one or both testicles.
- Pelvic floor pathology: The muscles of the pelvic floor play a vital role in supporting organs and maintaining core stability. When these muscles become overactive, weak, or develop trigger points, they can irritate surrounding nerves. The resulting pain often radiates into the testicle, creating a misleading impression that the source lies within the scrotum rather than the pelvic muscles themselves.
Additional causes of testicular pain can include:
- Surgical trauma (vasectomy, benign prostatic hyperplasia (BPH) interventions, prostatectomy)
- Biomechanical or structural dysfunction (hip dysfunction, piriformis syndrome, scoliosis, leg length discrepancy)
- Excessive exercise or changes to exercise routine
- Excessive sitting
- Chronic constipation and straining
- Jelqing and/or attempts at gential enhancement or foreskin regeneration
- In rare cases, bladder, prostate, or sexually transmitted infections after successful resolution of infection
- The majority of men with pelvic pain (including testicular pain), with or without urinary or bowel complaints, have pelvic floor dysfunction
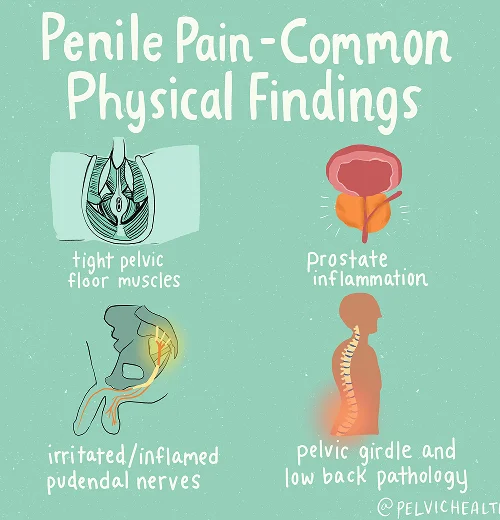

Symptoms of Testicular Pain
- The discomfort associated with testicular pain can vary widely, from burning sensations to dull aches that linger.
- This pain can reach into the penis, anus, and lower pelvic structures, affecting mobility and comfort.
Additional symptoms frequently present themselves alongside the pain:
- Increased pelvic tension during long sitting periods or physical exertion.
- Urinary frequency, urgency, or slow urinary stream.
- Ejaculation pain that radiates through the penis and scrotum.
- Occasional erectile weakness or reduced ejaculation force.
- Digestive issues such as bloating and constipation are also common.
- These digestive troubles often appear without clear cause or may follow physical stress.
- Symptoms can persist or appear intermittently throughout the day or week.
Associated Diagnoses
Testicular and pelvic pain can originate from a combination of problems affecting the lumbar spine, vascular system, and pelvic floor, all of which may interact and worsen each other’s impact. Lumbar conditions often present as nerve irritation or referred pain that develops from herniated discs, arthritic changes, or spinal compression in the lower back. Vascular conditions such as varicocele, testicular torsion, and pelvic venous congestion disrupt blood flow and lead to aching or throbbing sensations in the pelvic region. The pelvic floor is frequently involved, with links to Chronic Pelvic Pain Syndrome (CPPS), pudendal neuralgia, painful bladder syndrome, and hard flaccid syndrome. In many cases, dysfunction in this muscle group becomes the primary source that perpetuates or heightens pain throughout the surrounding structures.
Diagnostic Challenges
A large number of men experience ongoing testicular pain, which is frequently misdiagnosed as prostatitis. Often, antibiotics are administered unnecessarily since no bacterial infection can be identified. Clinical findings indicate that more than 90 percent of men suffering from pelvic or genital pain do not actually have a bacterial prostate infection.
These cases are most often categorized under the National Institutes of Health’s Category IIIa and IIIb, both subtypes of Chronic Pelvic Pain Syndrome (CPPS). In many cases, the discomfort is aggravated by irritation of the lumbar nerves or restricted circulation, which can mimic the same discomfort linked to pelvic floor dysfunction and delay effective treatment.
The National Institutes of Health provides the following classification system for prostatitis syndromes:
- Category I: Acute bacterial prostatitis is a sudden and painful infection of the prostate, presenting with intense discomfort, fever, and urinary symptoms resulting from bacterial contamination.
- Category II: Chronic bacterial prostatitis represents a recurring or persistent bacterial infection that continues to cause inflammation and repeated urinary tract infections linked to the same microorganism.
- Category IIIa: Inflammatory chronic pelvic pain syndrome includes immune cell activity within prostate fluids, semen, or post-massage urine, indicating an inflammatory response.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome mimics the symptoms of Category IIIa but shows no presence of white blood cells, suggesting a noninfectious origin of pain.
- Category IV: Asymptomatic inflammatory prostatitis involves silent inflammation in the prostate discovered incidentally, without the patient reporting pain or urinary disturbances.

The National Institutes of Health provides the following classification system for prostatitis syndromes:
- Category I: Acute bacterial prostatitis is a sudden and painful infection of the prostate, presenting with intense discomfort, fever, and urinary symptoms resulting from bacterial contamination.
- Category II: Chronic bacterial prostatitis represents a recurring or persistent bacterial infection that continues to cause inflammation and repeated urinary tract infections linked to the same microorganism.
- Category IIIa: Inflammatory chronic pelvic pain syndrome includes immune cell activity within prostate fluids, semen, or post-massage urine, indicating an inflammatory response.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome mimics the symptoms of Category IIIa but shows no presence of white blood cells, suggesting a noninfectious origin of pain.
- Category IV: Asymptomatic inflammatory prostatitis involves silent inflammation in the prostate discovered incidentally, without the patient reporting pain or urinary disturbances.

Treatment for Testicular Pain
Depending on what is causing your discomfort, whether the issue is muscular tightness, nerve compression along the lower spine, or impaired circulation that restricts blood flow to the pelvic region, your treatment plan may involve multiple methods that collectively aim to normalize the way your pelvic floor functions. This individualized plan often blends manual techniques, movement retraining, and neuromuscular re-education to bring your body back into healthy alignment.
- Pelvic floor physical and occupational therapy for pelvic floor dysfunction: Using evidence-based methods, this therapy retrains the pelvic muscles to contract and relax properly, which helps release built-up tension and restore comfort. Nerve irritation also decreases as muscle coordination improves.
- Spine and back treatment: For individuals with lumbar nerve compression, the plan may feature physical therapy that focuses on posture correction, core support, and mobility training. Guided injections can sometimes complement therapy for inflammation relief.
- Vascular-related treatment: When vascular flow is reduced, therapy techniques like controlled breathing and posture correction encourage better circulation and reduce stress on pelvic veins.
- Addressing biomechanical issues: Problems related to alignment or restricted hip motion are corrected through exercises that strengthen and balance the muscles. Restoring full mobility reduces tension throughout the pelvic area.
- Lifestyle adjustments: Adjusting daily habits like sitting time, diet, and activity levels supports healing and prevents future flare-ups of pain or tightness.
How We Can Help You with Testicular Pain
Men searching from Oceanside who have been dealing with chronic testicular pain may find relief through specialized pelvic floor physical and occupational therapy. At PHRC, we always begin with a detailed discussion of your symptoms, prior diagnoses, and any treatments that have been attempted. This helps our team pinpoint the possible sources of pain and outline an effective plan for care.
Many of our Oceanside clients arrive after years of uncertainty, having tried multiple treatments that failed to deliver results. Our therapists understand this frustration and take the time to listen carefully, offering a treatment roadmap that makes the process feel structured and achievable.
During the physical evaluation, your therapist examines muscle tone, pelvic stability, and nerve sensitivity while noting how movement patterns contribute to discomfort. After completing the assessment, your therapist explains your results in detail and develops a goal-oriented plan for recovery.

How We Can Help You with Testicular Pain
Men searching from Oceanside who have been dealing with chronic testicular pain may find relief through specialized pelvic floor physical and occupational therapy. At PHRC, we always begin with a detailed discussion of your symptoms, prior diagnoses, and any treatments that have been attempted. This helps our team pinpoint the possible sources of pain and outline an effective plan for care.
Many of our Oceanside clients arrive after years of uncertainty, having tried multiple treatments that failed to deliver results. Our therapists understand this frustration and take the time to listen carefully, offering a treatment roadmap that makes the process feel structured and achievable.
During the physical evaluation, your therapist examines muscle tone, pelvic stability, and nerve sensitivity while noting how movement patterns contribute to discomfort. After completing the assessment, your therapist explains your results in detail and develops a goal-oriented plan for recovery.

Therapy usually takes place once or twice per week for around 12 weeks, with home exercises provided to accelerate progress. Your PHRC therapist will also work alongside your healthcare providers to ensure a coordinated plan of care. Our focus is to help you restore comfort and improve your overall quality of life.
