Are you experiencing lingering testicular pain while living in or near San Diego? Although infection might seem like the logical explanation, pain in this area can actually stem from pelvic floor dysfunction, irritated nerves in the lower back, or poor blood circulation throughout the pelvic muscles.
Because these symptoms can mimic prostatitis, testicular discomfort is often treated incorrectly with antibiotics. When those medications bring little relief, it is usually a sign that the problem is rooted in the muscles or nerves instead of an infection.
If you are in San Diego and exploring alternatives, pelvic floor physical and occupational therapy can provide meaningful results. These non-invasive treatments help release tension, balance muscle coordination, and restore pelvic strength. Addressing the root cause promotes long-term recovery and greater comfort.
What are the Causes of Testicular Pain?
Testicular discomfort may be triggered by multiple physiological systems, including issues rooted in the lumbar spine, vascular circulation, or pelvic floor muscular function.
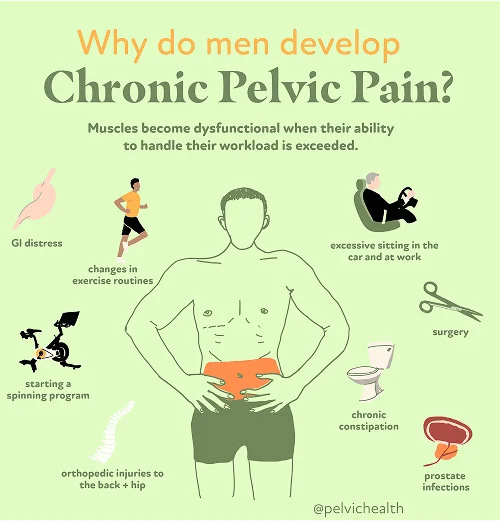
- Lumbar pathology: Because the testicular nerves originate in the lower back, disorders such as lumbar disc protrusion, degenerative spinal changes, or nerve compression can lead to referred pain. This means that the discomfort is perceived in the testicle even though the true problem is within the spinal column.
- Vascular pathology: When venous flow in the pelvic region becomes compromised, conditions such as varicoceles, torsion, or venous congestion may arise. These vascular abnormalities can produce sensations of dull throbbing, dragging heaviness, or intermittent sharp pain around the testicular area.
- Pelvic floor pathology: The pelvic floor is composed of layered muscles that provide foundational support to the pelvis. When muscle tension, weakness, or spasm develops, it can irritate sensitive pelvic nerves, sending referred pain signals to the testicle. Many men interpret this discomfort as coming from the testicle itself, even though it actually originates from the muscles below the pelvis.
Additional causes of testicular pain can include:
- Surgical trauma (vasectomy, benign prostatic hyperplasia (BPH) interventions, prostatectomy)
- Biomechanical or structural dysfunction (hip dysfunction, piriformis syndrome, scoliosis, leg length discrepancy)
- Excessive exercise or changes to exercise routine
- Excessive sitting
- Chronic constipation and straining
- Jelqing and/or attempts at gential enhancement or foreskin regeneration
- In rare cases, bladder, prostate, or sexually transmitted infections after successful resolution of infection
- The majority of men with pelvic pain (including testicular pain), with or without urinary or bowel complaints, have pelvic floor dysfunction
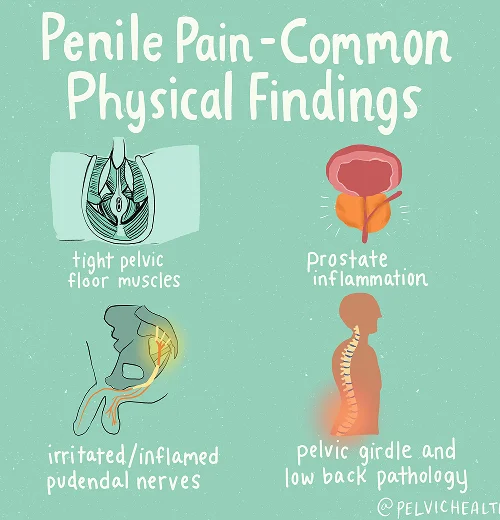

Symptoms of Testicular Pain
- Men suffering from testicular discomfort frequently describe sensations that are sharp, aching, or burning in nature.
- These sensations can extend into the penis, scrotum, or perineum, sometimes creating a widespread pelvic ache.
Other symptoms often accompany this condition and help in clinical assessment:
- Pelvic pain that intensifies with sitting or physical exertion.
- Urinary problems including frequent urination and decreased flow strength.
- Pain during ejaculation that may affect the scrotal and perineal regions.
- Some may experience erectile difficulties or weakened ejaculation force.
- Digestive symptoms such as bloating and constipation often arise simultaneously.
- These gastrointestinal problems might flare up after activity or appear randomly.
- The discomfort tends to come and go, varying in duration and strength.
Associated Diagnoses
Discomfort in the testicular and pelvic regions often results from overlapping dysfunctions involving the lumbar spine, blood vessels, and pelvic floor. Lumbar pathology can manifest as lumbar radiculopathy or radiating pain caused by disc injuries, spinal arthritis, or nerve compression. Vascular conditions, including varicocele, testicular torsion, and pelvic venous congestion, interfere with proper circulation and can cause chronic aching or heaviness. The pelvic floor itself frequently contributes to the problem and is closely tied to conditions such as Chronic Pelvic Pain Syndrome (CPPS), pudendal neuralgia, painful bladder syndrome, and hard flaccid syndrome. For many individuals, tension or weakness in the pelvic floor acts as a key factor that either initiates discomfort or worsens pain driven by other structural or vascular abnormalities.
Diagnostic Challenges
Testicular pain is a condition frequently reported by men, but it is often mistakenly associated with prostatitis. In such cases, antibiotics are prescribed without clear evidence of bacterial infection. Scientific reviews consistently demonstrate that over 90 percent of men who experience persistent pelvic or genital pain do not have a bacterial infection of the prostate gland.
Most of these individuals are classified under the National Institutes of Health’s Category IIIa or Category IIIb, both of which describe types of Chronic Pelvic Pain Syndrome (CPPS). Furthermore, irritation of spinal nerves and restricted blood circulation can imitate similar patterns of pelvic pain, complicating accurate diagnosis and slowing treatment.
As described by the National Institutes of Health, prostatitis syndromes are divided into the following groups:
- Category I: Acute bacterial prostatitis refers to an infection of the prostate that causes severe pain, fever, and urinary symptoms directly resulting from bacterial invasion.
- Category II: Chronic bacterial prostatitis is a longer-term condition where the prostate remains infected, producing repeated urinary infections by the same type of bacteria.
- Category IIIa: Inflammatory chronic pelvic pain syndrome is confirmed when testing reveals white blood cells in seminal or prostate fluid samples, showing clear signs of inflammation.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome shares the same discomfort and pain but lacks any visible inflammatory cells in laboratory results.
- Category IV: Asymptomatic inflammatory prostatitis features inflammation of the prostate tissue found during tests, even though the patient experiences no symptoms or pain.

As described by the National Institutes of Health, prostatitis syndromes are divided into the following groups:
- Category I: Acute bacterial prostatitis refers to an infection of the prostate that causes severe pain, fever, and urinary symptoms directly resulting from bacterial invasion.
- Category II: Chronic bacterial prostatitis is a longer-term condition where the prostate remains infected, producing repeated urinary infections by the same type of bacteria.
- Category IIIa: Inflammatory chronic pelvic pain syndrome is confirmed when testing reveals white blood cells in seminal or prostate fluid samples, showing clear signs of inflammation.
- Category IIIb: Noninflammatory chronic pelvic pain syndrome shares the same discomfort and pain but lacks any visible inflammatory cells in laboratory results.
- Category IV: Asymptomatic inflammatory prostatitis features inflammation of the prostate tissue found during tests, even though the patient experiences no symptoms or pain.

Treatment for Testicular Pain
Depending on the main factor contributing to your pain, whether it involves overly tense pelvic floor muscles, irritated nerves stemming from the lower back, or poor blood flow that limits oxygen supply to tissues, your therapy plan may include a strategic mix of modalities that work together to rebuild normal pelvic function. This might include relaxation exercises, specialized stretches, and gentle manual therapy that improves how your muscles and nerves interact.
- Pelvic floor physical and occupational therapy for pelvic floor dysfunction: This therapy helps the pelvic muscles learn to relax and contract correctly again, alleviating irritation and promoting natural coordination. Over time, the approach reduces pain intensity and improves comfort during movement.
- Spine and back treatment: When the pain source lies in the lower back, your program may include targeted spine therapy, posture work, and sometimes guided injections to decrease swelling around sensitive nerves.
- Vascular-related treatment: For issues tied to poor blood flow, pelvic therapy incorporates exercises and breathing techniques that improve circulation and relieve pressure in congested veins, promoting healing and comfort.
- Addressing biomechanical issues: Imbalances in hip movement can contribute to strain. Focused exercises help correct these mechanical issues, increase flexibility, and restore a healthier balance in the pelvic region.
- Lifestyle adjustments: Therapists often provide practical guidance for easing constipation, staying active in moderation, and avoiding extended sitting to reduce irritation and maintain progress.
How We Can Help You with Testicular Pain
If you are based in San Diego and struggling with ongoing testicular pain, professional evaluation by a pelvic floor physical and occupational therapist could provide the answers you have been searching for. At PHRC, we begin every assessment with a detailed conversation about your health history, previous treatments, and current symptoms. This allows us to uncover the true cause of your condition.
Many San Diego residents come to us after years of frustration and uncertainty. Our compassionate therapists focus on listening and creating a clear, step-by-step plan that helps you feel supported and informed throughout your recovery.
During your evaluation, your therapist will carefully examine the muscles and nerves surrounding your pelvis while observing your body’s natural movement patterns. Afterward, you will receive a full explanation of your findings and set achievable goals for both short-term improvement and long-term relief.

How We Can Help You with Testicular Pain
If you are based in San Diego and struggling with ongoing testicular pain, professional evaluation by a pelvic floor physical and occupational therapist could provide the answers you have been searching for. At PHRC, we begin every assessment with a detailed conversation about your health history, previous treatments, and current symptoms. This allows us to uncover the true cause of your condition.
Many San Diego residents come to us after years of frustration and uncertainty. Our compassionate therapists focus on listening and creating a clear, step-by-step plan that helps you feel supported and informed throughout your recovery.
During your evaluation, your therapist will carefully examine the muscles and nerves surrounding your pelvis while observing your body’s natural movement patterns. Afterward, you will receive a full explanation of your findings and set achievable goals for both short-term improvement and long-term relief.

Therapy sessions typically occur once or twice a week for about 12 weeks. You will also be given individualized home exercises to promote faster healing. Your PHRC therapist coordinates care with your entire medical team to ensure a smooth recovery journey. Our mission is to help you experience lasting relief and improved well-being.
