Testicular pain is a common but often misunderstood issue that can affect men of all ages. While occasional discomfort may be minor, persistent or recurring pain can significantly impact daily life, sexual function, and overall well-being. Men experiencing this type of pain often feel uncertain about its cause, which can increase stress and anxiety.
Understanding the potential causes of testicular pain and exploring effective, non-invasive treatment options is essential for long-term relief. One promising approach is pelvic floor physical and occupational therapy, which targets underlying dysfunctions in the muscles and nerves of the pelvic region. PHRC specializes in pelvic pain rehabilitation, providing tailored care for men dealing with chronic or acute testicular discomfort. Early intervention can prevent the condition from worsening and improve quality of life.
Understanding Testicular Pain
What is Testicular Pain?
Testicular pain can manifest in different ways, and understanding the type of pain you’re experiencing is important for proper diagnosis and treatment. Pain may be acute, appearing suddenly and intensely, or chronic, lingering for weeks or months. In some cases, the pain may not originate directly in the testicles but is instead referred pain, meaning it comes from another area such as the pelvis, groin, or lower abdomen.
Pain can vary in intensity, from a dull ache that comes and goes to sharp, stabbing sensations that interfere with movement or daily activities. Men often hesitate to seek medical care, but addressing pain early is crucial, as it can indicate underlying infections, injuries, or nerve dysfunction that may worsen if left untreated.
Why Addressing Testicular Pain Matters
Ignoring testicular pain can have both physical and emotional consequences. Chronic discomfort may:
- Limit mobility and daily activities, making routine tasks challenging
- Affect sexual performance or result in erectile dysfunction
- Cause psychological stress, anxiety, or depression due to prolonged discomfort
Addressing testicular pain proactively allows for timely intervention, which can prevent long-term complications and reduce the risk of chronic pelvic or nerve-related issues. Men who seek care from pelvic floor specialists often find significant improvement in pain management and overall quality of life.
Common Causes of Testicular Pain
Testicular pain can result from a wide range of issues, from infections to nerve or muscle dysfunction. Identifying the underlying cause is essential for selecting the most effective treatment.
Injury or Trauma
Physical injury is one of the most straightforward causes of testicular pain. Common triggers include:
- Sports-related injuries or sudden impacts to the groin
- Falls or accidents that place pressure on the scrotum
- Heavy lifting or abrupt movements that strain the pelvic region
- Heavy lifting or abrupt movements that strain the pelvic region
Even minor trauma can lead to lingering discomfort if not managed properly, and repeated injury can exacerbate nerve irritation and muscle tension.
Infection and Inflammation
Infections in the reproductive or urinary system are a frequent source of testicular pain. Some common conditions include:
- Epididymitis: Inflammation of the epididymis, often caused by bacterial infections
- Orchitis: Inflammation of the testicles, sometimes linked to viral infections such as mumps
- Sexually transmitted infections (STIs): Can contribute to swelling, tenderness, and discomfort
Prompt diagnosis and treatment with antibiotics or antiviral therapy, combined with supportive care, are critical to prevent long-term complications such as infertility.
It is important to have a medical evaluation to rule out the common causes. If symptoms persist, pelvic floor and girdle and lumbar factors may be in play.
Varicocele and Hydrocele
Structural issues within the scrotum can also cause chronic pain:
- Varicocele: Enlarged veins in the scrotum, sometimes described as feeling like a “bag of worms,” can cause aching and heaviness
- Hydrocele: Fluid accumulation around the testicle may result in pressure, swelling, and discomfort
While these conditions are not always dangerous, they can interfere with daily life and may require medical or surgical intervention if persistent.
Hernias and Other Structural Issues
Certain structural conditions can create referred pain in the testicles:
- Inguinal hernias: Occur when tissue from the abdomen protrudes into the groin, creating tension or pressure on nearby nerves
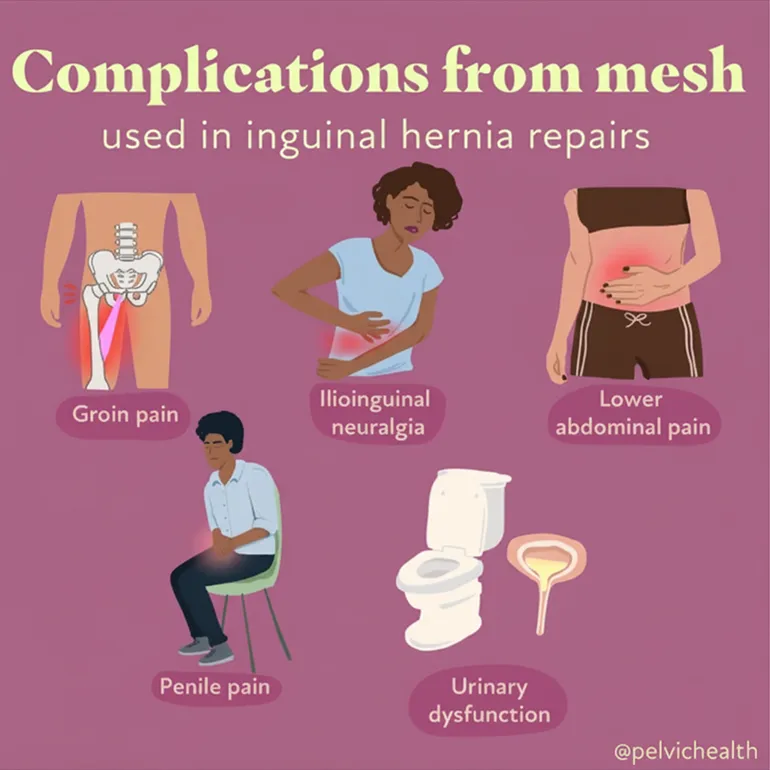
- Other anatomical abnormalities: Can place strain on pelvic muscles and nerves, indirectly causing testicular pain
Recognizing these causes is essential, as some may require medical evaluation or corrective surgery in addition to therapeutic intervention.
Nerve or Pelvic Floor Dysfunction
Many men experience testicular pain due to underlying dysfunction in the pelvic floor muscles or nerves. Factors include:
- Tight, weak, or imbalanced pelvic floor muscles that create chronic tension
- Nerve entrapment or irritation, often involving the pudendal or genitofemoral nerves
- Referred pain from nearby muscles in the lower back, hips, or groin
These issues are often not addressed with medication alone, which is why pelvic floor physical and occupational therapy can be highly effective in restoring normal function and relieving pain.

How Pelvic Floor Physical and Occupational Therapy Can Help
Pelvic floor therapy offers a non-invasive, evidence-based approach for men experiencing testicular pain, particularly when traditional treatments have not provided relief.
What is Pelvic Floor Therapy?
The pelvic floor is a group of muscles, ligaments, and connective tissues that support the bladder, bowel, and reproductive organs. Dysfunction in this area can lead to pain, tension, and nerve irritation that may radiate to the testicles. Pelvic floor therapy includes:
- Physical therapy: Techniques that release tight muscles, improve flexibility, and restore strength
- Occupational therapy: Focuses on lifestyle adjustments, activity modifications, and ergonomics to reduce strain on the pelvic region
These therapies aim to treat the root cause of pain rather than just the symptoms.
Specific Techniques for Testicular Pain
Pelvic floor specialists use a combination of techniques tailored to each patient, including:
- Manual therapy and myofascial release: Helps reduce tension and adhesions in pelvic muscles
- Posture and ergonomics education: Guides proper body mechanics to minimize stress during daily activities
- Activity modification: Adjustments to work routines, exercise, and sitting habits to prevent flare-ups
By addressing both muscle and nerve dysfunction, therapy provides a comprehensive approach to relief.
Benefits of Therapy
Men who undergo pelvic floor therapy may experience:
- Significant reduction in testicular and pelvic pain
- Improved mobility and overall muscle function
- Enhanced sexual and urinary function
- A non-invasive, drug-free alternative to long-term medication or surgery
PHRC provides personalized pelvic pain rehabilitation programs designed to safely and effectively address chronic testicular discomfort in men.
Evidence and Success Stories
Research and clinical experience show that pelvic floor therapy can significantly reduce chronic testicular pain, particularly when caused by nerve entrapment or pelvic floor muscle dysfunction. Many men report improved quality of life, decreased reliance on pain medication, and a return to normal daily activities after completing therapy programs.
When to See a Healthcare Professional
Red Flags Requiring Immediate Attention
Some symptoms may indicate a serious underlying condition requiring urgent medical evaluation, including:
- Sudden, severe pain
- Swelling, redness, or warmth in the testicles
- Fever or chills
- Recent trauma or injury to the groin
Prompt attention can prevent serious complications and allow for early treatment of infections, hernias, or other urgent conditions.
Integrating Pelvic Floor Therapy with Medical Care
For optimal results, pelvic floor therapy should be integrated with medical care. Urologists or primary care physicians can rule out infections, hernias, or structural abnormalities, while therapists focus on restoring muscle balance and reducing nerve irritation. Collaboration between medical providers and pelvic floor specialists ensures comprehensive treatment and long-lasting relief.
Self-Care and Lifestyle Tips
Alongside therapy, certain self-care strategies can support recovery and minimize future pain.
Gentle Exercises and Stretching
- Focus on stretching the hips, lower back, and pelvic region
- Avoid high-impact or aggressive movements during flare-ups
Heat/Cold Therapy for Pain Relief
- Ice packs can reduce inflammation during acute pain episodes
- Warm compresses help relax tight muscles and improve blood flow
Activity Modification and Ergonomic Adjustments
- Adjust sitting posture or workstation setup to reduce pelvic strain
- Limit heavy lifting, sudden twisting, or prolonged sitting that aggravates symptoms
By combining therapy with these lifestyle strategies, men can achieve more sustainable relief and prevent recurrence.
The Takeaway
Testicular pain can stem from injury, infection, structural problems, or pelvic floor dysfunction, making an accurate diagnosis essential for effective treatment. Pelvic floor physical and occupational therapy offers a safe, non-invasive, evidence-based approach to reduce discomfort, restore function, and improve quality of life. Men with chronic or persistent pain can benefit from personalized therapy programs at PHRC, which target pelvic floor and nerve-related issues, with early evaluation and intervention key to achieving lasting relief and returning to normal activities.

