Table of Contents
-
.
-
.
-
.
-
.
-
.
-
.
-
.
-
.
-
.
When Should I See a Pelvic Floor Physical and Occupational Therapists?
-
.
Persistent pelvic pain, bladder discomfort, painful sex, and persistent inflammation are symptoms many people live with for years before receiving clear answers. These symptoms are common, but they’re often misunderstood, misdiagnosed, or minimized.
New research and clinical observations are shedding light on an overlooked contributor to this pain: mast cells.
Mast Cell Activation Syndrome (MCAS) and endometriosis share overlapping pathways of inflammation, immune system dysfunction, and hormonal influence. Together, they can actually amplify pain and create complex patterns that affect multiple body systems.
At the Pelvic Health and Rehabilitation Center, we recognize that managing these interconnected conditions requires a deeper understanding of how the immune system, hormones, and the pelvic floor interact, and how physical and occupational therapy can help restore balance and function. In this article, we’ll share more about MCAS and endometriosis, how these two conditions are connected, and the treatment available.
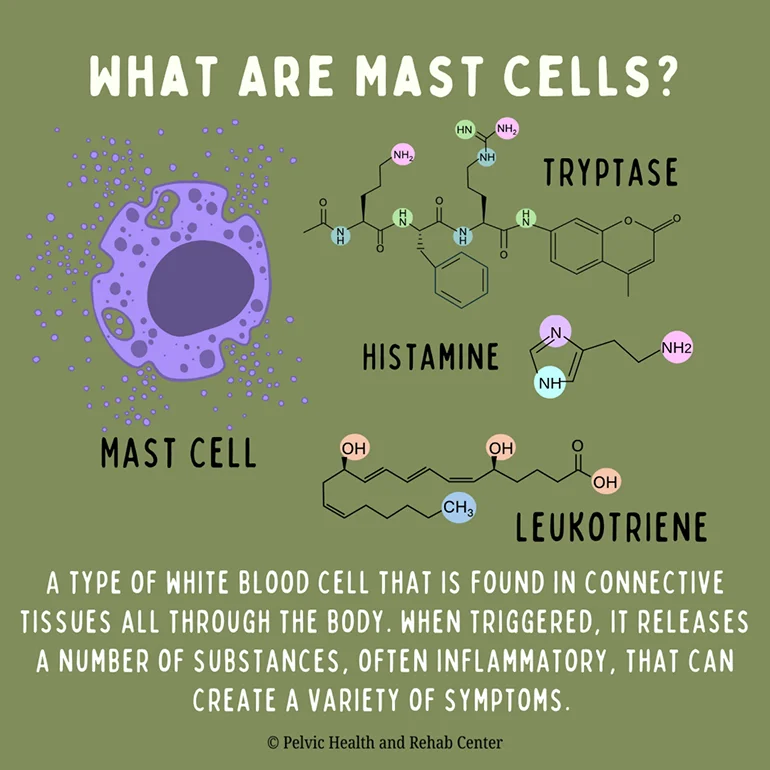
What are Mast Cells?
Mast cells are part of the immune system and are most concentrated in tissues that interact with the outside environment, such as the respiratory and digestive tracts, the genitourinary system, the skin, and connective tissue. When triggered, these cells release chemical mediators like histamine, leukotrienes, and tryptase—among many others.
Most people associate mast cells with allergies, but research shows they also contribute to chronic inflammation, pain, and tissue remodeling.
What is Mast Cell Activation Syndrome?
Mast Cell Activation Syndrome (MCAS) occurs when mast cells become overly reactive and release excessive amounts of inflammatory mediators. This overactivation can affect multiple body systems and cause a wide range of symptoms. MCAS is distinct from mastocytosis, which involves an increased number of mast cells, and from typical allergic reactions.
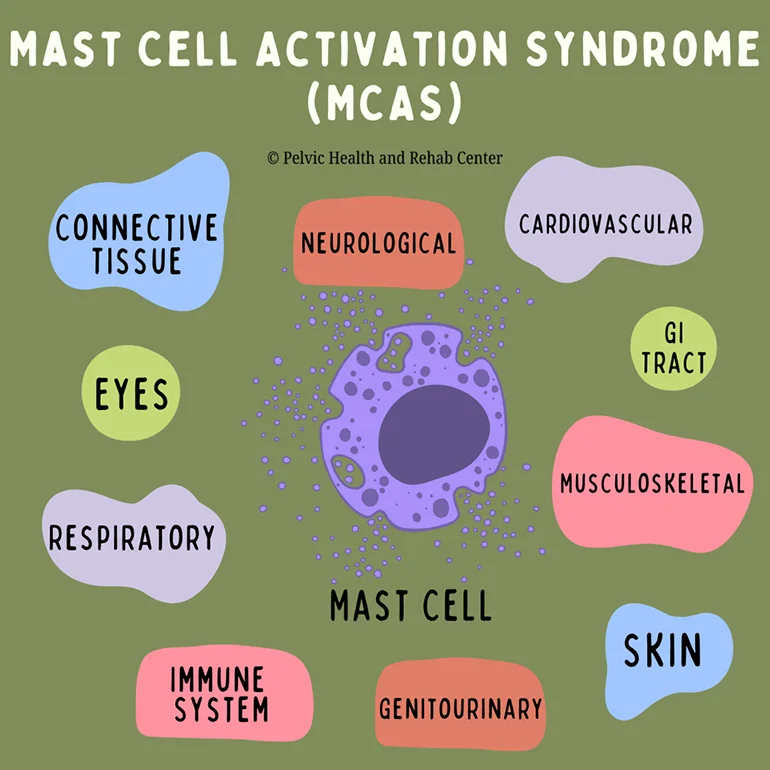
Mast Cells and the Body Systems They Affect
A very thorough article by Dr. Lawrence Afrin and colleagues (2020) reviewed the diagnosis of MCAS, and we’ve summarized various symptoms specific to each body system below. MCAS can affect nearly every organ system in the body. Persistent activation of mast cells results in a wide range of symptoms, which can make the condition hard to identify. Below are some of the main systems affected:
- Skin: Flushing, itching, rashes, dermatographism (skin writing), and hives.
- Eyes: Irritated or often dry eyes, episodic difficulty focusing, lid tremors/tic.
- Gastrointestinal: Nausea, abdominal pain, bloating, reflux, constipation, or diarrhea.
- Genitourinary: Bladder pain, urinary frequency, interstitial cystitis, vaginal pain (vulvodynia), and menstrual irregularities.
- Neurological: Headaches, dizziness, nerve pain, brain fog, memory issues, and sensory hypersensitivities.
- Cardiovascular: Heart palpitations, blood pressure swings, and lightheadedness or fainting.
- Respiratory: Shortness of breath, wheezing, cough, and sinus congestion.
- Musculoskeletal/Connective tissue: Muscle and joint pain, hypermobility (especially in conditions like Ehlers-Danlos Syndrome).
- Endocrine and Immune: Hormonal imbalances, thyroid dysfunction, and increased susceptibility to allergies and infections, hypersensitivity reactions, impaired healing
Many patients experience a very long diagnostic journey due to the broad impact MCAS can have on the body and how it often mimics or overlaps with many other disorders.
What is Endometriosis?
Endometriosis is a persistent inflammatory disease influenced by estrogen that affects roughly one in ten people assigned female at birth. It involves the growth of tissue similar to the uterine lining outside the uterus. While painful periods (dysmenorrhea) and infertility are the most recognized symptoms, many experience a variety of other overlapping pain conditions. About 90 percent of those with endometriosis live with pelvic pain, and pelvic floor physical and occupational therapists play an important role in its management and treatment.
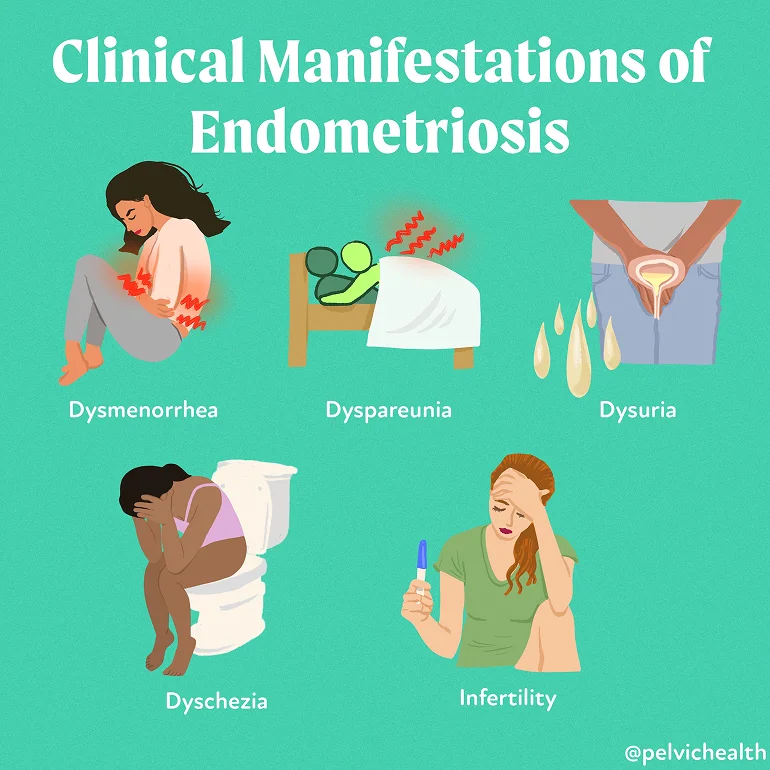
Symptoms of Endometriosis
The symptoms of endometriosis vary from person to person; however, some common signs include:
- Painful periods (dysmenorrhea): Those with endometriosis often experience severe cramping, abdominal pain, and lower back pain during their menstrual cycles.
- Pelvic pain: Pelvic pain may occur not only during menstruation but also before or after it. The severity of pain can range from mild to debilitating.
- Pain during intercourse (dyspareunia): Endometriosis can cause pain during or after sexual intercourse, which may be felt deep within the pelvis.
- Pain during urination or bowel movements: Some experience pain while urinating or having a bowel movement, particularly during their periods.
- Excessive bleeding: Heavy menstrual bleeding (menorrhagia) or bleeding between periods (metrorrhagia) can be symptoms of endometriosis.
- Infertility: Endometriosis is a common cause of infertility, as it can lead to the formation of adhesions and scar tissue that can interfere with the normal function of reproductive organs.
- Fatigue: Many report experiencing persistent fatigue and low energy levels.
- Digestive issues: Endometriosis can cause gastrointestinal symptoms such as bloating, constipation, diarrhea, and nausea, particularly around menstruation.
- Irritative bladder symptoms: Those with endometriosis often experience simultaneous urinary urgency, frequency, and pain in the absence of infection.
Because the symptoms can be subtle or seemingly unrelated, pelvic floor dysfunction often goes undiagnosed for years, leaving patients with persistent pain and frustration. A targeted evaluation by a trained pelvic health specialist is essential for identifying the problem and creating an effective treatment plan.
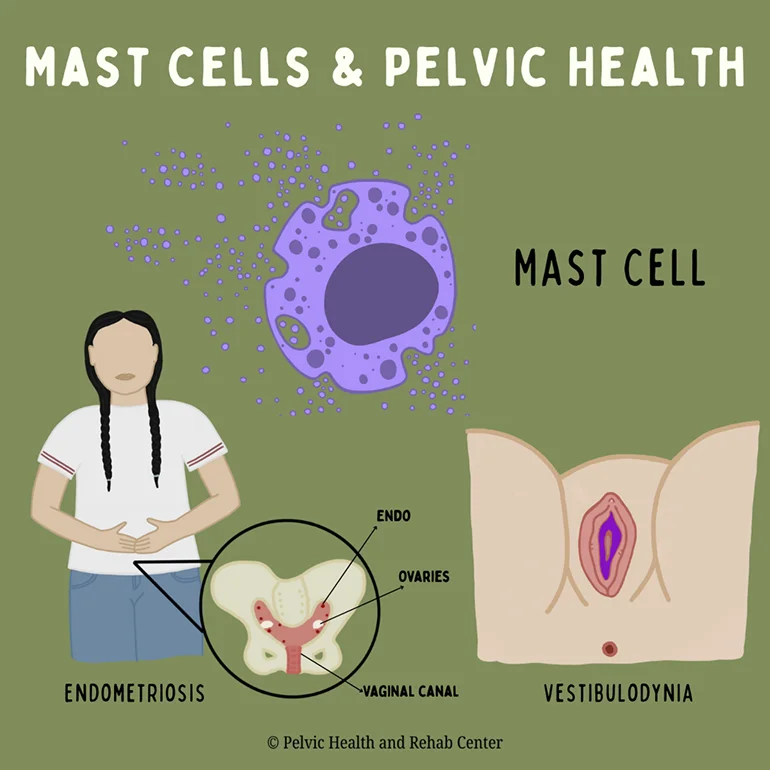
Mast Cells and Endometriosis: The Overlap
Endometriosis lesions can attract mast cells, which release inflammatory mediators that heighten pain, promote tissue changes, and worsen the disease. Estrogen, which fuels endometriosis, also activates mast cells, creating a cycle where hormones and immune cells reinforce each other’s effects. This ongoing communication between mast cells and endometrial tissue amplifies inflammation, nerve growth, and pain sensitivity throughout the pelvis.
This overlap helps explain why hormonal treatments alone, such as birth control, often fall short. While they can regulate estrogen, they don’t address the immune and inflammatory components driven by mast cell activity.
Recognizing the role of mast cells broadens the therapeutic approach, opening the door to treatments that calm inflammation, reduce nerve irritation, and support overall pelvic function through modalities like pelvic floor physical and occupational therapy.
Treatment: How We Can Help You
If you’re living with ongoing pelvic pain, painful sex, bladder discomfort, vulvar burning, muscle tightness, or other symptoms and haven’t found clear answers, you’re not alone. At PHRC, we specialize in treating complex pelvic pain. Our team understands how mast cell activation, endometriosis, hormonal influences, and musculoskeletal dysfunction can interact to create chronic pain and inflammation. While research on mast cell–related conditions continues to evolve, our team is experienced in helping patients find relief through an integrated approach.
1. Comprehensive Evaluation
We start with a detailed assessment to identify the factors driving your symptoms and design a treatment plan that addresses your unique needs.
2. Manual Therapy
Our therapists incorporate pelvic floor physical and occupational therapy through hands-on techniques to release fascial and muscular restrictions, calm overactive nerves, improve blood flow, and promote tissue healing.
3. Therapeutic Exercise
You’ll learn individualized exercises that strengthen, lengthen, and balance your pelvic floor and surrounding muscles to support long-term recovery.
4. Patient Education
We’ll teach you how to manage flares, reduce triggers, and use self-care strategies to maintain progress beyond your therapy sessions.
5. Assessment and Plan
Based on your history and clinical findings, we identify and address all contributing pain generators. Treatment might include manual therapy, exercise, education, and collaboration with other specialists such as mental health providers, pain management experts, or endometriosis surgeons.
6. Multidisciplinary Care Planning
Because endometriosis and MCAS are complex, we coordinate with your broader care team—pelvic pain specialists, allergists, and surgeons—to create a cohesive plan that supports your overall well-being.
Take Control of Your Pelvic Health Today
Don’t let endometriosis and MCAS hold you back any longer. Discover the benefits of our specialized pelvic floor physical and occupational therapy services and take the first step toward a healthier, happier future. Contact us today to schedule your initial pelvic floor therapy consultation and begin your journey to relief and recovery.