Testicular pain can feel alarming, frustrating, and hard to explain, especially when it lingers or keeps coming back. Many men assume the issue must be an infection or a problem with the testicles themselves. In reality, testicular pain often links back to pelvic floor dysfunction, nerve irritation in the lower back, or changes in circulation and muscle coordination. Because these causes do not show up on standard tests, testicular pain often gets labeled as prostatitis, leading to repeated rounds of antibiotics that do not solve the problem.
For most men, antibiotics do not address the true source of pain. Research and clinical experience show that over 95 percent of men with chronic pelvic pain, including testicular pain, do not need antibiotics. They need care that targets how the pelvic floor muscles, core, and nervous system work together. Pelvic floor physical and occupational therapy focuses on reducing muscle tension, restoring coordination, and calming irritated nerves, which can lead to meaningful and lasting relief.
If you are unsure who to see for testicular pain, understanding the role of pelvic floor physical and occupational therapy can help you choose the right next step and avoid unnecessary treatments.
Who Should I See For Testicular Pain?
When testicular pain persists or returns without a clear cause, the right specialist is often not who most people expect. While urologists can play an important role in ruling out infection, torsion, or structural concerns, many men reach a point where tests come back normal, and symptoms continue. That is when the focus needs to shift from the testicles alone to how the pelvis, muscles, and nerves function as a system.
In these cases, a pelvic floor physical and occupational therapist is often the most appropriate provider to see. Testicular pain commonly stems from overactive or poorly coordinated pelvic floor muscles, irritation of nearby nerves, or dysfunction that develops after stress, injury, prolonged sitting, or athletic strain. Pelvic floor physical and occupational therapy addresses these underlying contributors by evaluating movement patterns, muscle tone, breathing, posture, and nerve sensitivity rather than relying on medication alone.
Seeing a pelvic floor physical and occupational therapist helps identify why the pain started, what keeps it going, and how to calm the system so symptoms improve. For many men, this approach leads to answers and relief after months or even years of frustration with treatments that never fully addressed the source of the pain.
What are the Symptoms of Testicular Pain?
The symptoms can include:
- Burning, aching, itching of the testicles
- These symptoms can also occur in the penis, scrotum, perineal, and/or anal area
In addition to testicular pain, many men also experience a combination of the following symptoms:
- Men suffering from pelvic pain often experience discomfort caused by sitting, certain types of exercises, and certain types of clothing.
- In addition to pelvic pain, men may experience urinary urgency, frequency, hesitancy, as well as a slower or diminished urinary stream.
- Pelvic pain can also cause discomfort in the penis, scrotum, and perineum, especially during or after ejaculation.
- Some men experience signs of erectile dysfunction, along with reduced ejaculation strength.
- Men may endure gastrointestinal distress, including bloating and constipation.
- Gastrointestinal symptoms can be aggravated by ejaculation, exercise, or may occur spontaneously without a clear trigger.
- These symptoms may occur intermittently or be constant over time.

What are the Causes of Testicular Pain?
Testicular pain often feels confusing because the source is not always the testicle itself. Pain can be referred from the lower back, blood vessels, or the pelvic floor muscles, which makes it harder to pinpoint without looking at the body as a whole. This is why pelvic floor physical and occupational therapy is often the right place to start, since it evaluates how the spine, muscles, nerves, and circulation work together rather than focusing on a single structure.
There are several potential causes of testicular pain, three of which are related to lumbar pathology, vascular pathology, and pelvic floor pathology.
- Lumbar pathology: The nerves that supply the testicles originate in the lower back. If a disc bulges, arthritis develops, or a lumbar nerve becomes irritated, pain can travel and be felt in the testicle even though the source is the spine.
- Vascular pathology: Blood flow issues—such as enlarged veins (varicoceles), twisting of the blood supply (torsion), or vascular congestion—can cause aching, heaviness, or sharp pain in the testicle.
- Pelvic floor pathology: The pelvic floor muscles act like a hammock supporting the pelvis. If they become tight, weak, or go into spasm, they can irritate nearby nerves and cause pain that feels like it is in the testicle, even though the muscles are the source.
Additional causes of testicular pain can include:
- Surgical trauma (vasectomy, benign prostatic hyperplasia (BPH) interventions, prostatectomy)
- Biomechanical or structural dysfunction (hip dysfunction, piriformis syndrome, scoliosis, leg length discrepancy)
- Excessive exercise or sudden changes to exercise routine
- Excessive sitting
- Chronic constipation and straining
- Jelqing and/or attempts at genital enhancement or foreskin regeneration
- In rare cases, bladder, prostate, or sexually transmitted infections—even after successful resolution of the infection
- The majority of men with pelvic pain (including testicular pain), with or without urinary or bowel complaints, have pelvic floor dysfunction
What are the Associated Diagnoses of Testicular Pain?
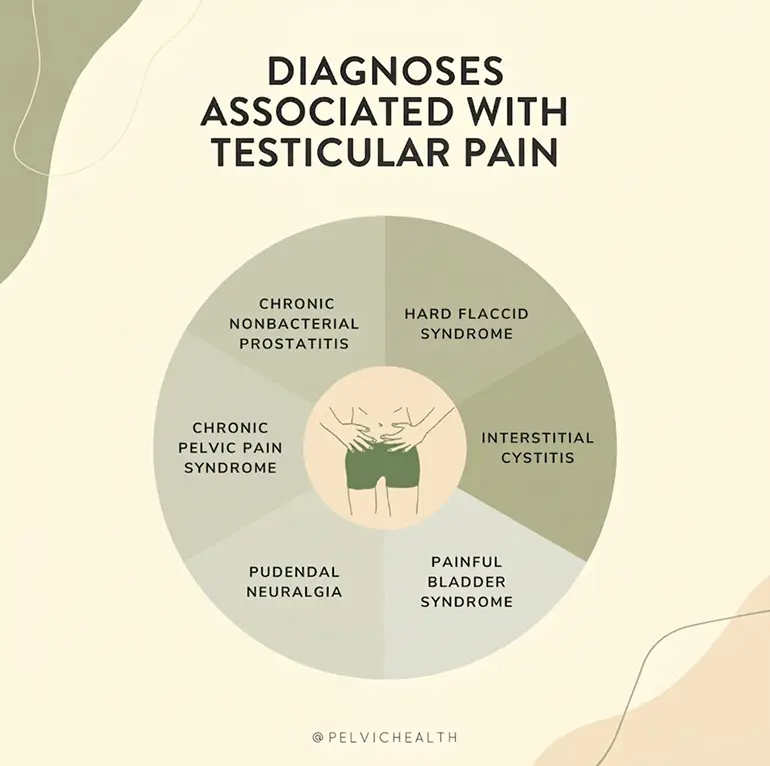
Lumbar, vascular, and pelvic floor pathologies can all connect to recognized diagnoses of testicular and pelvic pain. Lumbar pathology may appear as lumbar radiculopathy or referred pain from disc injury and arthritis in the lower back. Vascular pathology includes conditions such as varicocele, testicular torsion, or pelvic venous congestion, where altered blood flow creates pain signals. Pelvic floor pathology is most closely tied to Chronic Pelvic Pain Syndrome (CPPS), pudendal neuralgia, hard flaccid syndrome, and painful bladder syndrome. In many cases, pelvic floor dysfunction acts as the underlying link, either driving the pain directly or amplifying symptoms from other systems.
What are the Diagnostic Challenges?
Testicular pain can easily send men down the wrong treatment path. Many receive a diagnosis of prostatitis and leave with antibiotics, even when testing shows no active infection. Large bodies of research show that the vast majority of men with pelvic or genitourinary pain do not have a bacterial prostate condition driving their symptoms.
Most of these cases fall under Chronic Pelvic Pain Syndrome, specifically NIH categories IIIa and IIIb, where pain stems from muscle tension, nerve sensitivity, and dysfunction rather than infection. At the same time, irritation from the lumbar spine or vascular changes can closely resemble pelvic floor-related pain, making the picture even harder to sort out. This overlap frequently delays accurate diagnosis and keeps men cycling through treatments that never address the real source of their pain.
The National Institute of Health Classification of prostatitis syndromes is:
Category I: Acute bacterial prostatitis, which is associated with severe prostatitis symptoms, systemic infection, and acute bacterial urinary tract infection.
Category II: Chronic bacterial prostatitis, which is caused by chronic bacterial infection of the prostate with or without prostatitis symptoms and usually with recurrent urinary tract infections caused by the same bacterial strain
Category IIIa: Inflammatory chronic pelvic pain syndrome (white blood cells in semen and/or expressed prostatic secretions and/or third midstream bladder specimen)
Category IIIb: Noninflammatory chronic pelvic pain syndrome (no white blood cells in semen and/or expressed prostatic secretions)
Category IV: Asymptomatic inflammatory prostatitis, which is categorized by prostate inflammation in the absence of genitourinary tract symptoms
What is the Treatment for Testicular Pain?
Depending on the cause of your symptoms (this can be from tight/overactive pelvic floor muscles, nerve irritation, or blood flow issues), your treatment can include the below. At PHRC, our team of pelvic floor physical and occupational therapists can help treat your symptoms.
- Pelvic floor physical and occupational therapy for pelvic floor dysfunction: Helps release tight muscles, retrain coordination, and calm nerve irritation in the pelvis.
- Spine and back treatment: Physical and occupational therapy, posture correction, and sometimes injections if lumbar nerve irritation is the source of testicular pain.
- Vascular-related treatment: Pelvic floor therapy can reduce muscle guarding, improve circulation through posture and breathing techniques, and decrease pressure on congested veins.
- Addressing biomechanical issues: Therapy and targeted exercises to improve hip function, mobility, and overall body mechanics when structural problems contribute to pain.
- Lifestyle adjustments: Managing constipation, limiting prolonged sitting, and gradually returning to exercise to reduce pelvic strain.
As mentioned, over 95% of men with chronic pelvic pain (including testicular pain) often do not need antibiotics but instead need treatment for pelvic floor dysfunction.
PHRC: How We Can Help You with Testicular Pain
Men dealing with testicular pain often find clarity through an evaluation with a pelvic floor physical and occupational therapist who treats pelvic pain. At PHRC, your pelvic floor physical and occupational therapist takes time to understand your full story. This includes reviewing your symptoms, prior diagnoses, and any treatments you have tried, along with what helped and what did not.
By the time many men reach us, frustration has already built up. We recognize how disruptive and discouraging ongoing testicular pain can feel, especially after months or years of unanswered questions.
Your physical exam focuses on how your body moves and functions as a whole. Your pelvic floor physical and occupational therapist assesses muscles, joints, connective tissue, nerves, and movement patterns that can contribute to pain. After the exam, your therapist walks through the findings with you and explains how these factors connect to your symptoms. From there, they outline a clear treatment plan with short and long-term goals tailored to your needs.
Most people attend pelvic floor physical and occupational therapy one to two times per week for about 12 weeks. Your care also includes a home program that supports progress between visits. Throughout treatment, your pelvic floor physical and occupational therapist coordinates with other providers on your care team so you can move forward with a plan focused on real recovery and lasting relief.

