Tailbone pain, or coccydynia, is a condition that can affect anyone, yet it is often misunderstood or misdiagnosed. Many people assume that the discomfort is temporary or simply the result of sitting too long. However, tailbone pain can be persistent, disruptive, and sometimes linked to an underlying issue that often goes unrecognized: pelvic floor dysfunction.
Pelvic floor dysfunction involves problems with the muscles, ligaments, and connective tissues that support the pelvis and tailbone. These muscles play a critical role in stabilizing the coccyx and lower spine, meaning dysfunction can directly contribute to persistent tailbone pain. Understanding this connection is crucial for lasting relief.
At PHRC, experts in pelvic floor physical and occupational therapy specialize in treating both tailbone pain and pelvic floor dysfunction. Their personalized programs aim to address the root causes of pain rather than merely treating symptoms, offering patients a pathway to improved function, comfort, and long-term pelvic health.
What is Tailbone Pain (Coccydynia)?
Tailbone pain is localized discomfort at the very bottom of the spine, just above the buttocks. For many, it can feel sharp, aching, or throbbing, and may worsen when sitting, standing, or performing certain activities. While trauma is a commonly recognized cause, other contributing factors often go unnoticed.

Common Symptoms of Tailbone Pain:
- Pain while sitting, especially on hard surfaces
- Discomfort or sharp pain when transitioning from sitting to standing
- Pain during bowel movements or sexual activity
- Occasional swelling or tenderness around the coccyx

Common Causes of Tailbone Pain:
- Trauma or Falls: A fall directly onto the coccyx can bruise, fracture, or dislocate the tailbone. Even minor injuries can lead to persistent pain if not properly addressed.
- Repetitive Strain: Activities such as cycling, rowing, or prolonged sitting can put continuous pressure on the coccyx, gradually causing pain.
- Childbirth: Vaginal delivery can stretch or put pressure on the tailbone and pelvic muscles, sometimes resulting in long-term discomfort.
- Poor Posture: Slouching or sitting improperly over time places excessive stress on the coccyx and surrounding muscles.
- Idiopathic Causes: In some cases, tailbone pain occurs without any obvious cause, making diagnosis and treatment more challenging.
While addressing obvious triggers like trauma is important, persistent tailbone pain often requires exploring deeper musculoskeletal and pelvic factors, including pelvic floor dysfunction.

Understanding Pelvic Floor Dysfunction
The pelvic floor is a complex group of muscles and connective tissues that support the bladder, uterus or prostate, rectum, and lower spine. When these muscles do not function correctly, either becoming too tight, too weak, or poorly coordinated, it can lead to pelvic floor dysfunction (PFD).
Pelvic floor dysfunction is frequently associated with urinary, bowel, or sexual health issues. However, it can also contribute to musculoskeletal problems, including pain in the lower back, hips, and coccyx. Many people remain unaware that pelvic floor issues may be causing or worsening their tailbone pain.

Symptoms of Pelvic Floor Dysfunction:
- Difficulty controlling bladder or bowel movements, including urgency, frequency, or incontinence
- Pain or discomfort during sexual activity
- Muscle tightness, spasms, or weakness in the pelvic region
- Lower back, hip, or tailbone pain that persists despite rest or conventional treatment
Because the symptoms can be subtle or seemingly unrelated, pelvic floor dysfunction often goes undiagnosed for years, leaving patients with persistent pain and frustration. A targeted evaluation by a trained pelvic health specialist is essential for identifying the problem and creating an effective treatment plan.
The Missing Link: How Pelvic Floor Dysfunction Contributes to Tailbone Pain
The connection between tailbone pain and pelvic floor dysfunction lies in the anatomy of the pelvis and surrounding muscles. The coccyx is attached to various pelvic floor muscles, ligaments, and connective tissues. When these structures are not functioning optimally, the coccyx may experience abnormal tension or pressure, leading to pain.
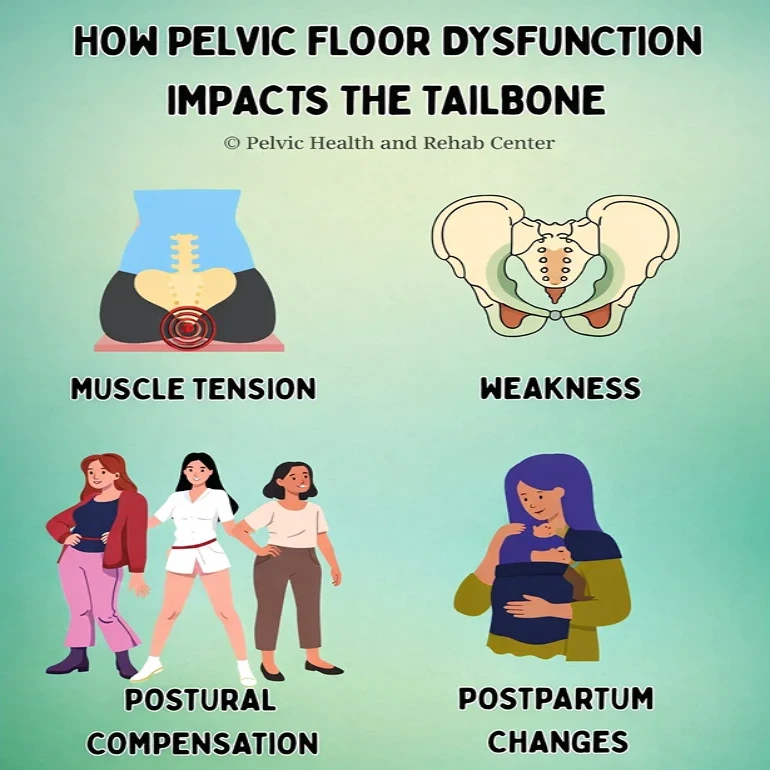
How Pelvic Floor Dysfunction Impacts the Tailbone:
- Muscle Tension: Overactive pelvic floor muscles can pull on the coccyx, causing sharp or persistent pain that may worsen when sitting or standing.
- Weakness: Underactive or weak pelvic floor muscles fail to stabilize the pelvis properly, placing additional stress on the tailbone and surrounding structures.
- Postural Compensation: When the pelvic floor is dysfunctional, individuals may unconsciously adjust their posture or movement patterns, inadvertently increasing coccyx strain.
- Postpartum Changes: Pregnancy and childbirth can stretch, weaken, or injure pelvic floor muscles, making the coccyx more susceptible to pain over time.
This relationship explains why traditional remedies like cushions, pain medication, or rest may provide only temporary relief. Addressing pelvic floor dysfunction is often the key to long-term improvement and the reduction of tailbone pain.
Diagnosing the Connection
Identifying pelvic floor dysfunction as a contributor to tailbone pain requires a detailed evaluation that goes beyond standard imaging or surface-level assessments.
What a Pelvic Health Physical and Occupational Therapist Will Assess:
- Medical History and Symptom Review: Understanding prior injuries, childbirth history, and activity levels.
- Physical Examination: Assessing pelvic floor muscles, coccyx mobility, hip alignment, and posture.
- Movement Analysis: Observing how sitting, standing, and walking affect coccyx position and pelvic stability.
- Muscle Function Testing: Evaluating strength, flexibility, and coordination of the pelvic floor muscles.
At PHRC, pelvic health specialists are trained to identify subtle dysfunctions that may be causing tailbone pain. Through a combination of hands-on assessment and evidence-based techniques, therapists develop a personalized treatment plan targeting the root cause rather than just managing symptoms.
Treatment Options and Strategies
Treatment for tailbone pain related to pelvic floor dysfunction focuses on relieving pain, restoring function, and addressing the underlying muscle imbalances. One of the most effective approaches is pelvic floor physical and occupational therapy, which targets the root causes of discomfort through specialized exercises and techniques.
At PHRC, therapists provide personalized pelvic floor physical and occupational therapy programs designed to:
- Relax overactive or tight pelvic floor muscles
- Strengthen weak or underactive muscles
- Restore proper coordination and function of the pelvic floor
This targeted therapy helps reduce tailbone pain, improve mobility, and support long-term pelvic health.
Pain Management Strategies:
- Heat or cold therapy to soothe inflammation and reduce discomfort
- Cushions or ergonomic seating for prolonged sitting
- Activity modification to avoid repetitive strain or pressure on the tailbone
When to Seek Medical Consultation:
- Persistent or worsening pain despite therapy
- Tailbone injury or suspected fracture
- Severe bowel, bladder, or nerve dysfunction
PHRC provides comprehensive treatment programs that integrate these strategies, helping patients achieve lasting relief from tailbone pain while improving overall pelvic floor health.
Self-Care and Preventive Measures
Alongside professional therapy, self-care practices can support recovery and prevent future tailbone pain.
- Daily Pelvic Floor Exercises: Gentle exercises to strengthen or relax pelvic muscles and improve coordination.
- Sitting Posture Tips: Use supportive cushions, sit with feet flat on the floor, and avoid slouching.
- Core Strengthening: Engage in exercises that support the lower back, hips, and pelvis.
- Mindful Movement: Avoid prolonged sitting and incorporate gentle stretches throughout the day.
- Lifestyle Adjustments: Maintain hydration, manage body weight, and incorporate ergonomic principles into daily routines.
By combining professional therapy with consistent self-care, patients can enhance the effectiveness of treatment and reduce the likelihood of recurrent tailbone pain.
When to Seek Professional Help
While mild tailbone discomfort may improve with home care, persistent or worsening pain should be evaluated by a professional. Signs that indicate the need for specialized assessment include:
- Severe or sharp pain that interferes with daily activities
- Numbness, tingling, or weakness in the legs
- Urinary or bowel dysfunction
- Recent trauma or injury to the tailbone
Early intervention by a pelvic health physical and occupational therapist can prevent persistent pain, restore mobility, and improve quality of life. The team at PHRC offers expert evaluations and personalized treatment plans to address both tailbone pain and pelvic floor dysfunction effectively.
The Takeaway
Tailbone pain is often linked to pelvic floor dysfunction, a connection that is frequently overlooked. Understanding this relationship allows for targeted treatment that addresses the root cause rather than just the symptoms. Consulting a pelvic health specialist, such as the team at PHRC, can provide personalized pelvic floor physical and occupational therapy programs to relieve pain, restore function, and improve overall pelvic health, helping patients achieve lasting relief and regain control of their daily lives.
Frequently Asked Questions
What causes tailbone pain after sitting for long periods?
Prolonged sitting can compress the coccyx and increase tension in the pelvic floor muscles, especially if they are tight, weak, or imbalanced.
Can pelvic floor dysfunction cause tailbone pain in men?
Yes. Pelvic floor dysfunction can affect both men and women, causing coccyx pain due to muscle tension, weakness, or postural changes.
How long does pelvic floor therapy take to relieve tailbone pain?
Improvement varies depending on severity and consistency of therapy, but many patients experience noticeable relief within a few weeks to several months.
Are there exercises I can do at home to help with tailbone pain?
Yes. Gentle pelvic floor stretches, core strengthening, and posture correction exercises can complement professional therapy and help reduce discomfort over time.

