The tailbone (also known as the coccyx) is often dismissed by some as a vestige of our prehistoric ancestors. Whether or not that is true, this is a bone that we need to examine further in order to appreciate. Not only is it a major attachment site for the pelvic floor muscles, but it can also become a huge source of discomfort if injured. More often than not a patient will tell me that they hurt their tailbone and went to see a doctor, only to be given a donut cushion and sent on their way. This is not the way to effectively manage and resolve tailbone pain, but I am getting ahead of myself…
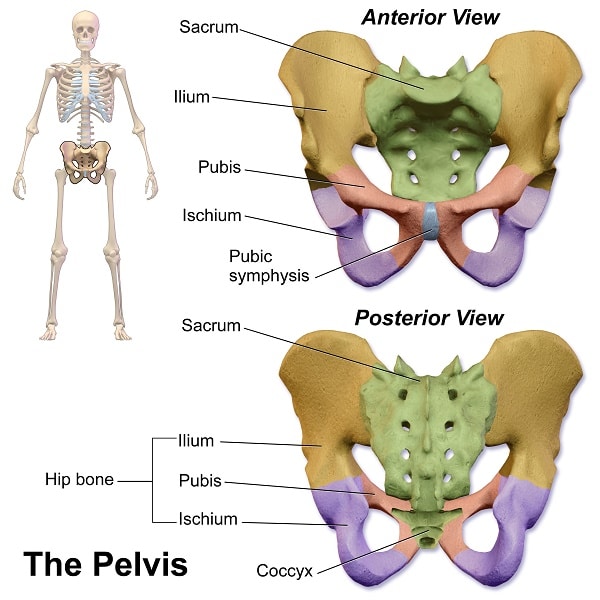
First, let’s learn the anatomy: The coccyx extends off of a large triangular bone at the base of the spinal column called the sacrum. It is made up of 3 to 5 bony segments which are connected to each other by ligaments, joint capsules, and fascia. There is a nerve that runs through the coccyx called the sacrococcygeal nerve which innervates the skin above the coccyx and sacrum. The tailbone serves as a bony attachment site for the entire deep layer of pelvic floor muscles (levator ani) and some of the superficial layer muscles (urogenital diaphragm) as well.
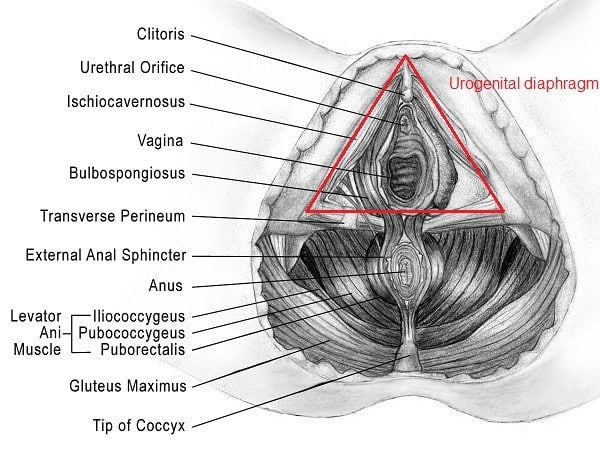
(Check out these blogs for a more in depth look at pelvic anatomy: male/female)
The tailbone is dynamic- as we contract our pelvic floor muscles the tailbone is flexing and extending in response. When we sit (especially when we slouch (and who doesn’t)) the tailbone becomes a weight bearing structure and when we have a bowel movement (or a more extreme scenario: give birth) the tailbone has to extend to allow evacuation through the pelvic canals (vagina and rectum).
Tailbone pain often feels dull and achy in the area between the gluteal cleft and above the anus but can also become sharp in certain situations (e.g sitting, sit to stand, lying on back). Bowel movements, penetrative sex, and orgasm can also be a source of aggravation for the tailbone. In my experience, I often find that people start having symptoms of tailbone pain but don’t seek medical attention right away because they figure that it should eventually pass…and sometimes it does. However, since the tailbone is a common attachment site for so many of our pelvic floor muscles it never really gets a break; therefore tailbone issues can develop into a persistent situation that can have a substantial effect on quality of life.
Here are some common causes of tailbone pain (coccydynia):
- A direct blow to the tailbone (i.e. fall, contact sports)
- Childbirth: during delivery, the baby’s head is positioned against the coccyx, and the pressure created during labor and pushing can result in injury to the tailbone and its surrounding structures. In rare cases, the coccyx can fracture.
- Repetitive/prolonged stress against the coccyx (i.e. cycling, rowing, prolonged sitting)
- Sometimes, the cause of coccyx pain is unknown (also known as idiopathic coccydynia)
- Less common causes of coccydynia includes bone spurs, cysts, compression of nerve roots, remote spinal injuries, local infections, and tumors. These should all be ruled out by a physician, especially if there is no clear mechanism of injury.
If you have had, or are currently experiencing, tailbone pain you can understand how troublesome it can be to deal with. It is not a part of our body that can be easily avoided and it can be difficult to access. One reason that tailbone pain can present and persist is due to pelvic girdle/sacroiliac joint bony alignment/misalignment. As we learned earlier, the tailbone forms a joint with the sacrum and becomes an attachment point for many pelvic structures. Not only can problems stemming from the sacroiliac joint give the illusion of tailbone pain, but two of our strongest pelvic ligaments (the sacrospinous and sacrotuberous ligaments) originate just above the sacrococcygeal joint (where the sacrum meets the tailbone) and can cause perceived tailbone pain when irritated.
Another reason that this symptom can become such a difficult-to-treat issue is because of relationship of the pelvic floor muscles and their physiological function. In a situation where we’ve had a direct blow to the tailbone, like a fall, there is likely a build up of inflammation in and around the bone causing a deep bruise feeling. And every time the pelvic floor muscles contract, they are tugging on the tailbone causing further irritation. This irritation then alerts the brain that there are injurious stimuli, which then cause the pelvic floor muscles to over-engage, become hypertonic, and develop trigger points. Thus, begins the vicious cycle of muscle dysfunction due to pain, a pattern that then leads to more muscle dysfunction and pain.
There are also cases in which the tailbone pain occurs either gradually or suddenly with no obvious cause. This can be due to tight pelvic floor muscles that are tight for any number of reasons: stress, previous injury, desk job, a combination of these, et cetera. It is in cases like this that the pelvic floor muscles become tight, which then pull on the tailbone and present as tailbone pain. In these cases, the tailbone is often not even painful to palpation, however if you were to palpate one of the adjacent pelvic floor muscles attaching to the coccyx (e.g. coccygeus, iliococcygeus, pubococcygeus) there is tenderness, hypertonus, and trigger points that may even directly reproduce the “tailbone” pain. This is a very common presentation that we see at PHRC.
So, I want to lay out some ideas on what to do if you are experiencing tailbone pain:
Rest: Minimize situations where you are going to be taxing the tailbone (sitting, standing for long periods, cycling). Use a cushion for sitting and try lying on your side or face down to allow plenty of blood flow to travel through the area. Here are some links to my favorite cushions:
Ice: Especially if you recently sustained a direct blow injury to the tailbone. Ice helps to constrict the blood vessels in the area and reduce inflammation. Heat is something you can also use but if it is within the first 2 weeks of injury stick with ice to flush the inflammation away from the injury site.*
Anti-inflammatories: This one you have to first discuss with your physician, but taking anti- inflammatory medication can be a huge help to interrupt the inflammatory cycle.
Roll: Use a tennis ball and roll some of the larger hip muscles-these muscles can tighten up in the presence of tailbone pain and cause further reduction of blood flow and pain. The best way to start with this is to lean back against a wall and place a tennis ball between your buttock and the wall. Gently use your bodyweight to apply pressure and roll on the tennis ball looking for sore spots. When you find a sore spot, hold and breathe until you feel a decrease in soreness intensity.
Schedule with a pelvic floor physical and occupational therapists: Because the pelvic floor muscles are so often involved with tailbone pain, it is important to schedule with a pelvic floor physical and occupational therapists sooner rather than later. Here are two previous blog posts on what to expect from a good pelvic floor physical and occupational therapy session.
**A common misconception that we hear regularly, is that the tailbone may be “out of place” or that it needs to be adjusted. It is true that tight pelvic floor muscles can have such a strong influence on the tailbone that they can actually pull it into a lateral bend, however, the root of the problem in this situation stills lies with the pelvic floor muscles. There are specific instances where the tailbone position may be affected due to a direct blow or childbirth and that is best identified through X-ray imaging. In these cases the tailbone may heal in the new position and will need to be assessed by your practitioner.
Tailbone pain is unfortunately one issue that can be mismanaged and overlooked within the medical community. However it can wreak absolute havoc on those of us having to deal with it on a daily basis. With these tips and resources you should have a better idea of where to start managing your tailbone pain in both the short and long term. This blog is here to give you hope that you can and will get better and you are not alone.
Additional resources:
International Pelvic Pain Society
American Physical and Occupational Therapy Association
*When using ice or heat be sure to set a timer and give your skin a break every 20 minutes
______________________________________________________________________________________________________________________________________
Are you unable to come see us in person? We offer virtual appointments!
Due to COVID-19, we understand people may prefer to utilize our services from their homes. We also understand that many people do not have access to pelvic floor physical and occupational therapy and we are here to help! The Pelvic Health and Rehabilitation Center is a multi-city company of highly trained and specialized pelvic floor physical and occupational therapistss committed to helping people optimize their pelvic health and eliminate pelvic pain and dysfunction. We are here for you and ready to help, whether it is in-person or online.
Virtual sessions are available with PHRC pelvic floor physical and occupational therapistss via our video platform, Zoom, or via phone. The cost for this service is $75.00 per 30 minutes. For more information and to schedule, please visit our digital healthcare page.
In addition to virtual consultation with our physical and occupational therapistss, we also offer integrative health services with Jandra Mueller, DPT, MS. Jandra is a pelvic floor physical and occupational therapists who also has her Master’s degree in Integrative Health and Nutrition. She offers services such as hormone testing via the DUTCH test, comprehensive stool testing for gastrointestinal health concerns, and integrative health coaching and meal planning. For more information about her services and to schedule, please visit our Integrative Health website page.
FAQ
What are pelvic floor muscles?
The pelvic floor muscles are a group of muscles that run from the coccyx to the pubic bone. They are part of the core, helping to support our entire body as well as providing support for the bowel, bladder and uterus. These muscles help us maintain bowel and bladder control and are involved in sexual pleasure and orgasm. The technical name of the pelvic floor muscles is the Levator Ani muscle group. The pudendal nerve, the levator ani nerve, and branches from the S2 – S4 nerve roots innervate the pelvic floor muscles. They are under voluntary and autonomic control, which is a unique feature only they possess compared to other muscle groups.
What is pelvic floor physical and occupational therapy?
Pelvic floor physical and occupational therapy is a specialized area of physical and occupational therapy. Currently, physical and occupational therapistss need advanced post-graduate education to be able to help people with pelvic floor dysfunction because pelvic floor disorders are not yet being taught in standard physical and occupational therapy curricula. The Pelvic Health and Rehabilitation Center provides extensive training for our staff because we recognize the limitations of physical and occupational therapy education in this unique area.
What happens at pelvic floor therapy?
During an evaluation for pelvic floor dysfunction the physical and occupational therapists will take a detailed history. Following the history the physical and occupational therapists will leave the room to allow the patient to change and drape themselves. The physical and occupational therapists will return to the room and using gloved hands will perform an external and internal manual assessment of the pelvic floor and girdle muscles. The physical and occupational therapists will once again leave the room and allow the patient to dress. Following the manual examination there may also be an examination of strength, motor control, and overall biomechanics and neuromuscular control. The physical and occupational therapists will then communicate the findings to the patient and together with their patient they establish an assessment, short term and long term goals and a treatment plan. Typically people with pelvic floor dysfunction are seen one time per week for one hour for varying amounts of time based on the severity and chronicity of the disease. A home exercise program will be established and the physical and occupational therapists will help coordinate other providers on the treatment team. Typically patients are seen for 3 months to a year.
What is pudendal neuralgia and how is it treated?
Pudendal Neuralgia is a clinical diagnosis that means pain in the sensory distribution of the pudendal nerve. The pudendal nerve is a mixed nerve that exits the S2 – S4 sacral nerve roots, we have a right and left pudendal nerve and each side has three main trunks: the dorsal branch, the perineal branch, and the inferior rectal branch. The branches supply sensation to the clitoris/penis, labia/scrotum, perineum, anus, the distal ⅓ of the urethra and rectum, and the vulva and vestibule. The nerve branches also control the pelvic floor muscles. The pudendal nerve follows a tortuous path through the pelvic floor and girdle, leaving it vulnerable to compression and tension injuries at various points along its path.
Pudendal Neuralgia occurs when the nerve is unable to slide, glide and move normally and as a result, people experience pain in some or all of the above-mentioned areas. Pelvic floor physical and occupational therapy plays a crucial role in identifying the mechanical impairments that are affecting the nerve. The physical and occupational therapy treatment plan is designed to restore normal neural function. Patients with pudendal neuralgia require pelvic floor physical and occupational therapy and may also benefit from medical management that includes pharmaceuticals and procedures such as pudendal nerve blocks or botox injections.
What is interstitial cystitis and how is it treated?
Interstitial Cystitis is a clinical diagnosis characterized by irritative bladder symptoms such as urinary urgency, frequency, and hesitancy in the absence of infection. Research has shown the majority of patients who meet the clinical definition have pelvic floor dysfunction and myalgia. Therefore, the American Urologic Association recommends pelvic floor physical and occupational therapy as first-line treatment for Interstitial Cystitis. Patients will benefit from pelvic floor physical and occupational therapy and may also benefit from pharmacologic management or medical procedures such as bladder instillations.
Who is the Pelvic Health and Rehabilitation Team?
The Pelvic Health and Rehabilitation Center was founded by Elizabeth Akincilar and Stephanie Prendergast in 2006, they have been treating people with pelvic floor disorders since 2001. They were trained and mentored by a medical doctor and quickly became experts in treating pelvic floor disorders. They began creating courses and sharing their knowledge around the world. They expanded to 11 locations in the United States and developed a residency style training program for their employees with ongoing weekly mentoring. The physical and occupational therapistss who work at PHRC have undergone more training than the majority of pelvic floor physical and occupational therapistss and as a result offer efficient and high quality care.
How many years of experience do we have?
Stephanie and Liz have 24 years of experience and help each and every team member become an expert in the field through their training and mentoring program.
Why PHRC versus anyone else?
PHRC is unique because of the specific focus on pelvic floor disorders and the leadership at our company. We are constantly lecturing, teaching, and staying ahead of the curve with our connections to medical experts and emerging experts. As a result, we are able to efficiently and effectively help our patients restore their pelvic health.
Do we treat men for pelvic floor therapy?
The Pelvic Health and Rehabilitation Center is unique in that the Cofounders have always treated people of all genders and therefore have trained the team members and staff the same way. Many pelvic floor physical and occupational therapistss focus solely on people with vulvas, this is not the case here.
Do I need pelvic floor therapy forever?
The majority of people with pelvic floor dysfunction will undergo pelvic floor physical and occupational therapy for a set amount of time based on their goals. Every 6 -8 weeks goals will be re-established based on the physical improvements and remaining physical impairments. Most patients will achieve their goals in 3 – 6 months. If there are complicating medical or untreated comorbidities some patients will be in therapy longer.


Comments
Thanks so much for this site. There is very, very little information on pelvic physical therapy. Do you know any resource I can use to find good PTs near me? I live in the Chicagoland area.
Hello Daniel,
Kotarinos Physical Therapy is located in Chicago. Anyone of their therapists would be qualified to treat you.
All my best,
Stephanie
Hi my name is narcy I fell on my tailbone skating but I have had a x-ray and CAT scan and they can’t figure out why I’m still hurting and they gave me a donut and sent me home . I’m still have pain till this day. I got hurt a few days after Christmas what should I Do?
Hello,
We recommend being evaluated by a pelvic floor physical therapist,. You can use the link below to find one in your area.
https://pelvicguru.com/2016/02/13/find-a-pelvic-health-professional/
Regards,
Admin
Hi, i have been suffering from coccyx pain and looks like it’s due to misaligned pelvis. Started after giving birth. I have had an coccyx manipulation and i was pain free for 4 months but it’s back again. What excercise do you recommend for this issue.
Author Allison Romero says:
“I would recommend being evaluated by a pelvic floor physical therapist to assess the cause of the recurrence of coccyx pain.” You can use the below link to find a physical therapist in your area.
https://pelvicguru.com/2016/02/13/find-a-pelvic-health-professional/
Do you know any Pelvic Physical Therapists in Fairfield county Connecticut?
Hi Joan,
Please use the below link to find a pelvic floor physical therapist in your area.
https://pelvicguru.com/2016/02/13/find-a-pelvic-health-professional/
Regards,
Admin
I had a xray of my tail bone because the last two weeks it’s been hurting. About 12 years again I fell in a boat and fracture my tail bone. Never had problems until now. I had the xray done and the doctor called and said my tailbone was flexing and i need to see a orthopaedic doctor. What does that mean. Flexing tailbone
Stephanie Prendergast, MPT says:
This means that your coccyx is bent at an angle that can cause pain at the joint. It may be like this from the fracture, because of a joint problem, a muscle problem, or a combination of all of the above.
After total hysterectomy, I have excruciating tailbone pain, but also cramps, stomach aches, burning sensation inside rectum and anal area (inside), also severe constipation, and I feel sick all over. Cannot have bowel movements with constantly taking laxatives.
I don’t know what I have, have had every test in the book for IBS, etc.
Does tailbone pain cause all of this. I also have a hiatal hernia that causes me indigestion, take prilosec. Gastro dr. doesn’t know what to do any more. Colorctal dr. said to have P.T.
I feel so sick and need to know if tailbone pain can cause all of this.
Thank you.
EMM
Stephanie Prendergast, MPT says:
“Hi EMM,
It is possible that the hysterectomy led to pelvic floor dysfunction and/or pudendal neuralgia versus it being a tailbone injury itself. It makes sense for you to see a pelvic floor physical therapist specializing in pelvic pain to get evaluated.”
Hi there,
I had a bad fall in Jan 2016 and was pregnant at the time, have since had my little boy who is 7months old. The pain from my coccyx got worse so I had an X-ray which showed a misaligned coccyx and pelvis. I’ve had Physio therapy (which seems to have made the pain worse). I’d love to Excersize to get rid of my baby tummy but it hurts. What can I do to stop the pain.
Many thanks
Angela
Hi Angela,
It sounds like you may have a pelvic floor disorder. Unfortunately we cannot make specific recommendations without evaluating you. We would be happy to evaluate you in one of our locations or you can use our website to find a pelvic floor physical therapist in your area that can help.
Regards,
Admin
It is very painful for me to sit. My doctor took x-rays of my tail bone and told me my pain is coming from where my pelvic bone meets my tail bone. All I know is that both sides of my butt feel bruised and is painful. The doctor just referred me to a rehab, I’m waiting to hear from them. He told me if rehab doesn’t work, the next step would be to have a shot in the pelvic bone on each cheek. I have purchased three different types of donut cushions to sit on and they hurt unless I align my butt a special way. Do you have any suggestions that might help me?
Hi Connie,
We recommend seeing a pelvic floor physical therapist so they can evaluate you. Please use the link below to find a provider in your area.
https://pelvicguru.com/2016/02/13/find-a-pelvic-health-professional/
Regards,
Admin
Hi there! I am currently experiencing tailbone pain. It has bothered me for 2 months without subsiding even with taking a week or two off. I usually run 5 miles a day, 3 times per week no problem. Lately my tailbone pain keeps me at 3 miles or less and very slow. I had twins with no problem 16 years ago. Delivery was a vaginal birth no complications. Very physically fit in the time in between. I also lift heavy. I have gone to my doctor and he is having me do an x-ray because he did to push on my tailbone and said that if I had a ligament problem that I would have jumped when he touched it. No my pain is not so much when I touch my tailbone but around the tailbone area you need my tailbone and my bowel movements have moved to from one city to a little bit all day. My doctor has said that that could be because I am nervous. I’m not the nervous type anyhow I’m just wondering what suggestions you have for me and if I should demand an MRI or a CAT scan to rule out any cancer or tumor, cyst ext. also do you know a specialist who can help me in Denver?
Thank you!
Tammy
Hi Tammy,
We recommend Hollie Neujahr, located in Denver, her number is (303) 260-5092.
Regards,
Admin
I had a direct hit an my buttock last year and took a rest for 1 month. The pain started in my ass just below the waist to the right to be exact. Pain is literally haunting me when I ride bike and and standing for long time using ice packs sometimes what should I do ?
Hi Rohith,
It sounds like you may have a pelvic floor disorder. Unfortunately we cannot make specific recommendations without evaluating you. We would be happy to evaluate you in one of our locations or you can use our website to find a pelvic floor physical therapist in your area that can help.
Regards,
Admin
I just had surgery on Feb 28th 2017 for prolapse of my bowel, bladder and vagina. The surgeons used my own ligaments to suspend my organs. The surgery was performed laparoscopically and vaginal. I am just over two weeks post op and i have thus incredible sharp pain in my tailbone accompanied by rectal bleeding which i have never had before. I did call the office and their response was just to ice it. I’m concerned, do you have any suggestions on what maybe causing me such pain? Thank you!
Hi Lynn,
It sounds like you may have a pelvic floor disorder. Unfortunately we cannot make specific recommendations without evaluating you. We would be happy to evaluate you in one of our locations or you can use our website to find a pelvic floor physical therapist in your area that can help.
Regards,
Admin
I fell and have a central cord syndrome injury my tail bone hurts to sit on it! Also when I go to bathroom an sit oncomode I feel like it is a sharp bone at my tailbone!
Hi Jane,
We recommend being evaluated by a pelvic floor physical therapist. Please use the link below to find one in your area.
https://pelvicguru.com/2016/02/13/find-a-pelvic-health-professional/
Regards,
Admin
About a month ago I fell directly on my tailbone onto cement pavers. I was in alot of pain for about two weeks and couldn’t sit what so ever..the hardest part being and still existing when trying to get up from the sitting position. I went to the ER and was the X-ray’s do not clearly show my coccyx bone but show everything else intact my doctor has said nothing can be done for me and just to buy a donut pillow and it may take a long time to heal. I am still experiencing sharp pain when I sit and I know this sound strange but I seem to only be able to defacate ..shortly after having intercourse. It will be days in between. Is this normal?
It sounds like you may have a pelvic floor disorder. Unfortunately we cannot make specific recommendations without evaluating you. We would be happy to evaluate you in one of our locations or you can use our website to find a pelvic floor physical therapist in your area that can help.
Regards,
Admin
I’ve been having low back pain for nearly two years now. It’s keeping me from working and many of the things I love. It’s also keeping me really depressed. I’ve done everything I know–doctors, chiro, massage, PT, injections, etc. I get lots of popping in different places in the low back/butt/sacrum area. I can sometimes do it by squeezing my butt and pelvic floor muscles, but other times it just won’t pop, and I’m just uncomfortable/miserable for days until it finally does. Some of them are quite jarring and they are almost always relieving. It usually happens after I’ve been sitting for a while. I can’t sit in a chair for more than 30 minutes without experiencing distracting discomfort. Bending, especially while bearing weight, is uncomfortable, and sometimes causes sharp pain. My right pelvic bone pokes forward more than my left one, and I know the ball of my right femur isn’t sitting correctly in the hip cavity. The two lowest discs are bulging. My low low back is often inflamed. Nothing I do seems to help, and I feel hopeless about it ever healing. Can you help?
Hi Holly,
It sounds like you may have a pelvic floor disorder. Unfortunately we cannot make specific recommendations without evaluating you. We would be happy to evaluate you in one of our locations or you can use our website to find a pelvic floor physical therapist in your area that can help.
If I have gotten a coccygectomy due to 3 years of idiopathic tailbone pain is there any hope for my pelvic floor or has it been ruined forever? I had hypertonic pelvic floor muscles before surgery. I worked with PT for a year before getting the surgery. Sadly the surgery didn’t help pain, it actually increased pain in my rectal area. Please let me know what you think.
Stephanie Prendergast, MPT says:
Hi Megan, getting better is always possible. Continue to work with your pelvic floor physical therapy and she will help you figure it out.
Hi, all of a sudden 6months ago my tailbone started to hurt. then, my ractum started to hurt, then I started to get constant pressure on my rectun which making me feel like running to washroom. Sometime nothing happens when I go.
So far palvic and tailbone MRI came normal. Prostate little swell, I am living with so many medication yet nothing helping.
Can you please kindly advise. Thank you for your time.
Sincerely,
Sariorsheab
Hello Sariorsheab,
It sounds like you may have a pelvic floor disorder. Unfortunately we cannot make specific recommendations without evaluating you. We would be happy to evaluate you in one of our locations or you can use our website to find a pelvic floor physical therapist in your area that can help.
Regards,
Admin
I have scoliosis and a scoliosis phyiotherapist set exercises which involved tightening the pelvic floor. Eventually this became so painful that it was difficult just to walk. A pelvic floor therapist has diagnosed overtight pelvic floor muscles but has also given exercises that start with tightening the pelvic floor. It should be ever so slightly but even this results in immediate pain. Can you suggest an alternative regime for learning to relax pelvic floor muscles?
Hi Maureen,
It sounds like you may have a pelvic floor disorder. Unfortunately we cannot make specific recommendations without evaluating you. We would be happy to evaluate you in one of our locations or you can use our website to find a pelvic floor physical therapist in your area that can help.
Regards,
Admin
I have had tailbone pain for 9 months now. It has taken me a while to figure out it was my tailbone since it started after removal of L5-S1 pedicle screws that were loose. Im now fused from L4-S1.. My spine surgeon says it has nothing to do with surgery and I don’t know what to do. My pcp gave me corticosteroid injections..no help. Cray did not show a fracture..any ideas?
Hi Bridget,
It sounds like you may have a pelvic floor disorder. Unfortunately we cannot make specific recommendations without evaluating you. We would be happy to evaluate you in one of our locations or you can use our website to find a pelvic floor physical therapist in your area that can help.
Regards,
Admin
Hi I have an extended tailbone, it never used to be a problem but it has been causing me a lot of pain for at least 5 months now, it hurts when i do simple things like sit up in bed in the morning and to get in and out of cars, I have searched all over the internet and can’t seem to find anything that will give me a better understanding?
Hi Jen,
It sounds like you may have a pelvic floor disorder. Unfortunately we cannot make specific recommendations without evaluating you. We would be happy to evaluate you in one of our locations or you can use our website to find a pelvic floor physical therapist in your area that can help.
Regards,
Admin
I have had tailbone pain for 4 months. It happened after I was lifting weights. I am seeing a pelvic pt right now and she is helping with trigger point and massaging the ligaments. I also hurt my lower back. If I do a bridge pose and descend vertebrae by vertebrae I feel fluid or air or some sort of sensation roll to the bottom of my tailbone. No one really knows what that could be. It’s not painful but just makes me nervous. My pelvic floor is also stuck in a cycle of inflammation. When you treat patients with just a ligament problem how long does it usually take to heal since there was no injury to the actual bone. Also when I go to the chiropractor to get my back/ sacrum adjusted my pelvic floor blows up. Do you have any idea why that would be? Also is it commen to have sacrum pain with all these other symptoms? Sorry for the novel thank you!
Stephanie Prendergast says:
Hi Katy,
Unfortunately it is hard to make recommendations or answer your questions without evaluating you. As a general rule of thumb you should feel a little better each week. It is common for tailbone and ligament issues to be associated with tight external hip rotators and this can also cause sacral pain. The back and pelvic floor can also refer pain to the sacrum. These are also great questions for your pelvic floor PT, she should be able to provide you with more specific answers based on your objective findings and her assessment.
After giving birth to my daughter the next day at the hospital my tailbone starts to hurt. They gave me norco and Motrin but the pain didn’t go away. Three days later I went to urgent care and they did xray but the X-ray showed my tailbone is normal. But up till now I’ve been having pain I don’t know what to do. My ob is not coming back till sept. And my doctor is fully book and won’t see me till September. It hurts when I put pressure and sitting and standing up and it get worst at night.
Hi Cris,
It sounds like you may have a pelvic floor disorder. Unfortunately we cannot make specific recommendations without evaluating you. We would be happy to evaluate you in one of our locations or you can use our website to find a pelvic floor physical therapist in your area that can help.
Regards,
Admin
Well, I broke my tailbone years ago and after having X-rays done, it showed I had broken my coccyx (nonunion). The doctor at the time (1998) said he would remove it because it was “like a tooth and I didn’t need). BTW…most painful surgery ever! I guess they shaved the bone and they said that was causing a lot of the pain! Helped a little but never got rid of pain, but I am sure my doctor in Mississippi didn’t do a lot of these surgeries so he wasn’t some kind of coccyx specialist. In 2007, pain increased and I lost all mobility at my waist to bend and twist. I no longer can work because I have tremendous amounts of pain and I can only sit and stand for 2 hours before having to lie on my sides. All the doctors I saw around here for the past ten years said they didn’t see a problem at all. Now I am seeing a pain mgt doctor in Houston, TX and he said that I have the spine of a 85 yr old lady, even though I am 45 yrs old. My l4/l5 are crushed and I have si joints that slip which most doctors have told me that is not happening! I am now starting to have the worst stabbing pain a little down from where my coccyx was and over an inch or two to the right. It feels like nerves are being pinched at times and my hips move so much that in Aquatic therapy they aligned them on first visit but my right si joint started really hurting after about 3 weeks and when the therapist checked my hips were out of alignment again. She put kinso tape on me which helped tremendously, but the night the tape came off I felt aomething slip in the right si joint and the pain was excruciating again! Any ideas or suggestions?
Stephanie Prendergast, MPT says:
Hi Gwen,
I am sorry to hear of your trouble. My suggestions are to form a team of medical professionals that can help you manage your symptoms and start to get better. This should include a pelvic floor physical therapist, a pain management doctor, and possibly a physiatrist. An interdisciplinary approach can help you mange your symptoms and recover.
Hi,
I have been experienceing tail bone pain for months and I think it is due to a winter ice fall coupled with sitting for studying. I saw a doctor and they recommended a cushion. I have been using for two weeks and have refrained from biking.
A few days ago my hip was tight walking and then I went to stretch it. Stretching it hurt like a muscle cramp and then it hurt to walk. I went to the clinic and they diagnosed me with Trochantric Bursitis. I’m on crutches for the week and my time sitting has sky rocketed. I take my cushion with me and use it but my tail bone is unhappy. They think my legs are a tad uneven.
I am wondering if these injures could be related?
Stephanie Prendergast, MPT says:
Hi Helga,
Trochanteric bursitis and tailbone pain can be cause by hypertonic hip external rotators and pelvic floor dysfunction. These issues are treatable and we recommend that you see a pelvic floor physical therapist.
I have pain in my right side to tail bone to plvis i have hard stool and gass stucked .after hard stool or exseetion i had increese my pain .after log time sitting had increased my pain.what cani do sugesset me which dr shold i go
Hi Bhawna,
Please use the link below to find a pelvic floor physical therapist in your area.
https://pelvicguru.com/2016/02/13/find-a-pelvic-health-professional/
Regards,
Admin
Thanks so much for this post! I am researching more about damaged coccyx symptoms. I have had low back pain and incredibly tight hips for most of my adult life (now 31) and it has grown worse over the past few years. I kept telling my GP how painful it was and she wouldn’t look further in to it. I tried acupuncture, osteo, yoga and aqua therapy and *finally* took myself to a chiropractor. He took x-rays and found my coccyx has been dislocated for 20 years. I am going back to my GP for a referral to a pelvic floor specialist and looking forward to finding ways to help ease what has always felt like a heavy weight and numbing around my lower torso.
I am wondering if coccyx damage can affect menstruation?
Stephanie Prendergast, MPT says:
Hi Ruby,
Coccyx fractures do not affect menstruation.
I sat for very long times programming for years. I started getting numbness down both feet. I went to back doctors and nobody can find anything. In trying to isolate, I see when I flex and kegal that’s when it hurts around my tailbone. The tightness of muscle down into my feet feel like a rubber band tightening when I stretch. Can you recommend a doctor in Greenville, SC
Hi Dennis,
Please use the link below to find a pelvic floor physical therapist in your area.
https://pelvicguru.com/2016/02/13/find-a-pelvic-health-professional/
Regards,
Admin
I had a bilateral si joint fusion a year ago. Following that I suffered pain in my tailbone, tolerable but still bothersome. I recently had l4-l5 fused and my tailbone pain is debilitating. I can’t sit or lay flat on my back. I had l5-s1 fused many years ago. My spine ortho is at a loss while my pain management doc seems to think the pain is soo bad because the tailbone is now taking all the stress that the fusions don’t. I am at a complete loss. I have never injured my tailbone. Now they are suggesting injections there to relieve some of the pain. Any ideas??? Thanks in advance
Stephanie Prendergast says:
Hi Melissa,
A pelvic floor physical therapist should be able to help and you may also want to consider discussing ganaglion impar injections with your physician. Both of these treatment modalities can help.
I fractured my tailbone back in June and my Dr. said it hasn’t even started healing yet. Is there a reason why? And should I be concerned about it? The pain seems to be getting worse and it’s messing with my sciatic nerve making it harder for me to walk.
Hi Tona,
It sounds like you may have a pelvic floor disorder. Unfortunately we cannot make specific recommendations without evaluating you. We would be happy to evaluate you in one of our locations or you can use our website to find a pelvic floor physical therapist in your area that can help.
Regards,
Admin
Hello I have been experiencing tailbone pain for the past few weeks and it’s getting worse and worse I’m not sure if it’s the tailbone or around it bit I don’t have health insurance so I can’t go see a Dr. I did not get this from falling, I don’t remember the last time I fell on my butt, and it’s definitely not from childbirth since I’m a guy that would be a little difficult. However I did just get off of a long days trip about 2 weeks ago and that’s when I felt the pain. Please help
Hi Joseph,
It sounds like you may have a pelvic floor disorder. Unfortunately we cannot make specific recommendations without evaluating you. We would be happy to evaluate you in one of our locations or you can use our website to find a pelvic floor physical therapist in your area that can help.
Regards,
Admin
I am in a lot of pain with my Cox’s area. It’s a very burning pain all the time. It is extremely painful when I go from laying to sitting position to get out of bed. I scream in pain every time. The bone hurts when it’s pressed on
Could you tell me what steps should I take?
It sounds like you may have a pelvic floor disorder. Unfortunately we cannot make specific recommendations without evaluating you. We would be happy to evaluate you in one of our locations or you can use our website to find a pelvic floor physical therapist in your area that can help.
Hello! I fell down a full flight of stairs about a week ago, and had significant bruising and swelling. The swelling has gone down now, but I am experiencing a very sharp shooting pain when I sit certain ways and when I press down on the bone under the area. I had initially thought that this was a fractured tailbone, but the pain is only on one side of my butt and not the middle. It is on the very top of my butt, where my lower back and butt meet. I’m trying to just let it heal on it’s own, but I can’t help but worry that it could be something serious. Do you know what this bone/area might be?
Hi Liz,
It sounds like you may have a pelvic floor disorder. Unfortunately we cannot make specific recommendations without evaluating you. We would be happy to evaluate you in one of our locations or you can use our website to find a pelvic floor physical therapist in your area that can help.
Regards,
Admin
Hey, I recently was playing soccer and got tripped by the goalie and I went flying about 4 feet in the air did a flip and landed directly on my tailbone and I can feel the bone is out of place/ kinda sticking out or maybe it’s just swollen. I have most of the symptoms for tailbone injury but I don’t have some of them. It hurts a lot to sit down. I could use some help. Thank you
It sounds like you may have a pelvic floor disorder. Unfortunately we cannot make specific recommendations without evaluating you. We would be happy to evaluate you in one of our locations or you can use our website to find a pelvic floor physical therapist in your area that can help.
8 months ago I had a sudden loss of flexibility in my groin and hip flexor, followed by constant tailbone pain. I have gone to multiple doctors and they say I am a mystery. I have had X-rays and MRIs and they do not see anything. Are these two problems related? Could this be a pelvic floor issue? Do you recommend any doctors or therapists in Southern Indiana?
It sounds like you may have a pelvic floor disorder. Unfortunately we cannot make specific recommendations without evaluating you. We would be happy to evaluate you in one of our locations or you can use our website to find a pelvic floor physical therapist in your area that can help.
Hi About 2 weeks ago I was just warming up and flexing before I went for a bath, I just bend down trying to touch my feet, I felt sudden snap on my lower back, with severe pain, took Aleve, went to doctor X Ray was done, nothing serious took naproxen. 3 days after the incident I started getting tailbone pain, within a week lower back pain was completely gone, now only tailbone pain remained, I am a male tailbone pain become severe every time I had an orgasm/Ejaculation. And I get the feeling of going to the loo but nothing comes. Both stool and urine is fine no constipation.
When I wake up in the morning I feel normal and zero pain as I walk and start doing work the pain becomes severe. Got X-ray for Coccyx nothing wrong too. No sudden Injury either.
Hello,
My situation is a bit weird. Around three years ago I started having very bad tailbone pain that started out of nowhere. After taking anti inflammatory, using a donut pillow and sort of resting my pain subsided. However, my pain recently came back again and it seems to be way worse (about 3 months ago). I also seem to have SI joint dysfunction and have been seen by several chiropractors/orthopedic surgeons who tell me my hips are misaligned and that inflammation is whats causing most of my pain. I am wondering if my tail bone pain is related to my SI joint dysfunction. Interestingly enough, it seems to hurt the most when I do certain exercises in which I squeeze my butt or when I cough. Anybody you would recommend me seeing? I live in Houston. Thanks!
Hi Paola,
We recommend you being evaluated by a pelvic floor pt. Please use the following to help locate one in your area https://pelvicguru.com/directory/