By: Melinda Fontaine, DPT, PHRC Walnut Creek
Lube is great! It adds moisture and decreases friction, but how do you pick from the multitude of different personal lubes on the market? Which one is the safest? Goop recently asked the same questions in response to watching an episode of Grace and Frankie in which Frankie makes her own lube. I have noticed a number of my patients can have very strong reactions to lubes including pain infection and fertility issues. Let’s take a look at what we are putting in our bodies.
What’s the Difference Between Moisturizers and Lubricants?
It’s all based on how long it is intended to stay in the body. Vaginal moisturizers are made to stay in the body for longer than 60 minutes, and are applied every 1-3 days to alleviate dryness. Vaginal moisturizers are classified as Medical Devices by the Medicines and Healthcare products Regulatory Agency because they last so long, which means they have been tested for safety and efficacy. They last so long because they contain polymers to adhere water to the vaginal lining. Lubricants are made to be used short term during sex. Some may be better than others for various activities.
Which Lube can I use with condoms or toys?
Lubricants may be water-, silicone-, mineral oil-, or plant-based. Water-based lubricants are non-staining, easy to wash off, and safe to use with all condoms and toys. Silicone-based lubricants are thicker and tend to hang around longer, so they are preferred by women who are past menopause or don’t want their lube to disappear too quickly. However, silicone-based lube required soap and water to get off and should not be used on silicone toys because it will basically dissolve the toy. Oil-based lubricants are least likely to irritate vaginal or anal tissues but cannot be used with condoms because they will break, and should not be used with toys because it will coat them in oil and prevent them from ever getting clean. Plant based-lubes, such as aloe vera are generally considered safe.
Can I Get an Infection from Lube?
Products, such as KY Jelly, Replens, Gynol II, and Astroglide leave you vulnerable to infection because they kill the good bacteria, lactobacilli, that keep you healthy. You may have noticed that everyone is talking about probiotics to replenish the good bacteria in our gut. Our vaginas and rectums also have good bacteria that play a vital role in our health. An important type of good bacteria called lactobacillus maintains a good pH in the vagina and prevents bacterial vaginosis. Low estrogen levels (as occur post menopause, postpartum, and after prolonged use of oral contraceptives) also reduce the vaginal pH and can lead to infection. Healthy vaginal pH is 3.8-4.5, and rectal pH is about 7.0. A good lube would have a pH value similar to your tissues or slightly higher.
What is Osmolality and What Does it Have to Do with Lube?
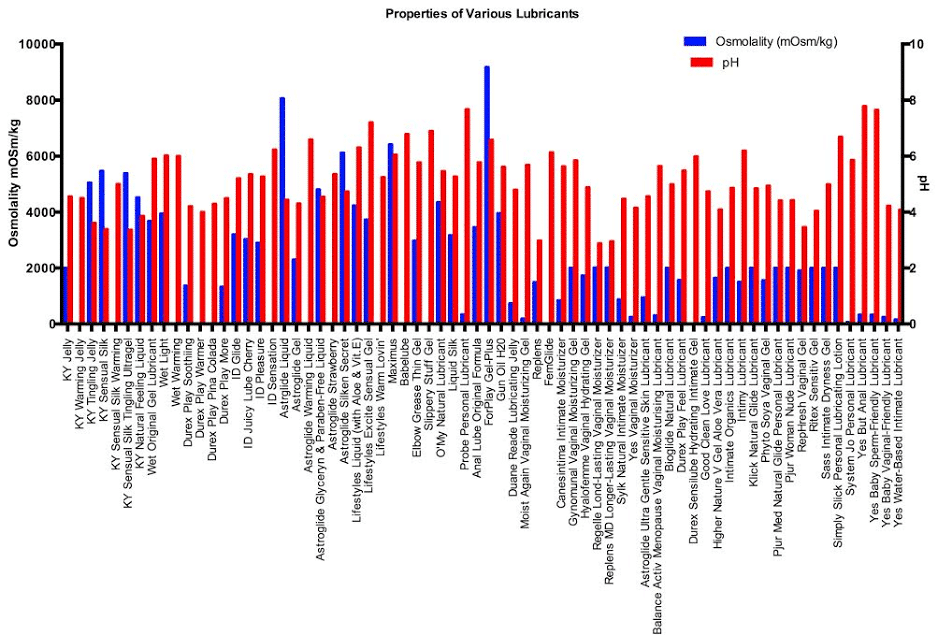
Osmolality is the concentration, or how many solutes are present in the lube. Products with high osmolality lead to damage of the tissues lining the vagina or rectum, causing irritation and leaving the tissues vulnerable to infection². The World Health Organization (WHO) recommends osmolalities of less than 380 mOsm/kg, or at most 1200 mOsm/kg. For example, Astroglide Liquid has an osmolality of 8064 and should be avoided. Lubes with osmolalities less than 316 mOsm/kg showed no adverse effects and include Good Clean Love, Slippery Stuff, Sliquid, Babelube, Probe, and Femglide. Silicone-, Plant, and Oil-based lube are also less likely to irritate, but their osmolality cannot be measured. See the figure for some common water-based lubricants with their osmolalities and pH values³.
What Else Could Be in My Lube?
Parabens, glycols, microbicides, and preservatives in many personal lubricants and moisturizers are also concerning. Most lubricants list the ingredients on the package, so you can find out what is in your lube. Parabens are preservatives and are similar to the female sex hormone, estrogen. It has been suggested that they may disrupt the endocrine system function in both sexes, and they have been detected in breast tumors. Glycols are molecules responsible for maintaining moisture, so they are used in many lubes, such as Durex Play Feel, ID Glide, and Pjur Woman Nude. Too much glycol can lead to vulnerability to herpes simplex virus 2, bacterial vaginosis, and yeast infections¹. The WHO advises that glycerol should be less than 9.9% mass fraction and propylene glycol should be less than 8.3% mass fraction³. Nonoxynol-9 is a compound added to lubes, such as Gynol II, for contraception because it kills sperm. It also damages the vaginal and rectal lining and increases risk for herpes and HIV². Chlorhexidine is a preservative associated with a 100-fold increased susceptibility to chlamydia¹ and is in KY Jelly and Astroglide.
How Does Lube Affect Fertility?
Some products, such as Astroglide, KY Jelly, and Replens, make it hard for little swimmers to swim, while sperm-friendly lubes (Pre-Seed and Yes Baby) have no effect². Low pH and high osmolality decrease sperm motility. The best conditions for sperm survival is pH 7.2-8.5 and osmolality 270-360 mOsm/kg. Interestingly, studies done on couples trying to conceive did not find a difference in fertility between couples who did and did not use lube¹.
What Lube Do you Recommend for People with Pelvic Pain?
Lubes that cause damage and irritation to the lining of the vagina or rectum can create pelvic pain or make existing pain worse.
- Pure coconut oil or aloe vera are the least irritating, but remember oil cannot be used with condoms.
- Silicone-based lubes without the above listed preservatives would be my second choice for someone with pelvic pain and can be used with condoms.
- Of the water-based lubes tested, Good Clean Love, Slippery Stuff, and Sliquid Organic are the safest.
- For couples trying to conceive, I recommend Yes Baby Sperm-Friendly Lubricant.
- For, anal play, a lube should have a higher pH, so I would choose Yes But Anal Lube.
- Lastly, in order to avoid tissue damage and infection, everyone should steer clear of the ever popular KY Jelly and Astroglide.
Every person has different preferences and tolerances, so experiment a little to find out what works for you. If you are plagued by recurrent infections or chronic pain, it might be worthwhile as Dr. Maggie Ney suggests, to take a break from all lubricant to see if it improves.
______________________________________________________________________________________________________________________________________
Are you unable to come see us in person? We offer virtual physical and occupational therapy appointments too!
In addition to virtual consultation with our physical and occupational therapistss, we also offer integrative health services with Jandra Mueller, DPT, MS. Jandra is a pelvic floor physical and occupational therapists who also has her Master’s degree in Integrative Health and Nutrition. She offers services such as hormone testing via the DUTCH test, comprehensive stool testing for gastrointestinal health concerns, and integrative health coaching and meal planning. For more information about her services and to schedule, please visit our Integrative Health website page.
Do you enjoy or blog and want more content from PHRC? Please head over to social media!
Like us on Facebook,
Subscribe to our YouTube Channel,
and follow us on Twitter, Instagram, Tik Tok and Pinterest!
References
FAQ
What are pelvic floor muscles?
The pelvic floor muscles are a group of muscles that run from the coccyx to the pubic bone. They are part of the core, helping to support our entire body as well as providing support for the bowel, bladder and uterus. These muscles help us maintain bowel and bladder control and are involved in sexual pleasure and orgasm. The technical name of the pelvic floor muscles is the Levator Ani muscle group. The pudendal nerve, the levator ani nerve, and branches from the S2 – S4 nerve roots innervate the pelvic floor muscles. They are under voluntary and autonomic control, which is a unique feature only they possess compared to other muscle groups.
What is pelvic floor physical and occupational therapy?
Pelvic floor physical and occupational therapy is a specialized area of physical and occupational therapy. Currently, physical and occupational therapistss need advanced post-graduate education to be able to help people with pelvic floor dysfunction because pelvic floor disorders are not yet being taught in standard physical and occupational therapy curricula. The Pelvic Health and Rehabilitation Center provides extensive training for our staff because we recognize the limitations of physical and occupational therapy education in this unique area.
What happens at pelvic floor therapy?
During an evaluation for pelvic floor dysfunction the physical and occupational therapists will take a detailed history. Following the history the physical and occupational therapists will leave the room to allow the patient to change and drape themselves. The physical and occupational therapists will return to the room and using gloved hands will perform an external and internal manual assessment of the pelvic floor and girdle muscles. The physical and occupational therapists will once again leave the room and allow the patient to dress. Following the manual examination there may also be an examination of strength, motor control, and overall biomechanics and neuromuscular control. The physical and occupational therapists will then communicate the findings to the patient and together with their patient they establish an assessment, short term and long term goals and a treatment plan. Typically people with pelvic floor dysfunction are seen one time per week for one hour for varying amounts of time based on the severity and chronicity of the disease. A home exercise program will be established and the physical and occupational therapists will help coordinate other providers on the treatment team. Typically patients are seen for 3 months to a year.
What is pudendal neuralgia and how is it treated?
Pudendal Neuralgia is a clinical diagnosis that means pain in the sensory distribution of the pudendal nerve. The pudendal nerve is a mixed nerve that exits the S2 – S4 sacral nerve roots, we have a right and left pudendal nerve and each side has three main trunks: the dorsal branch, the perineal branch, and the inferior rectal branch. The branches supply sensation to the clitoris/penis, labia/scrotum, perineum, anus, the distal ⅓ of the urethra and rectum, and the vulva and vestibule. The nerve branches also control the pelvic floor muscles. The pudendal nerve follows a tortuous path through the pelvic floor and girdle, leaving it vulnerable to compression and tension injuries at various points along its path.
Pudendal Neuralgia occurs when the nerve is unable to slide, glide and move normally and as a result, people experience pain in some or all of the above-mentioned areas. Pelvic floor physical and occupational therapy plays a crucial role in identifying the mechanical impairments that are affecting the nerve. The physical and occupational therapy treatment plan is designed to restore normal neural function. Patients with pudendal neuralgia require pelvic floor physical and occupational therapy and may also benefit from medical management that includes pharmaceuticals and procedures such as pudendal nerve blocks or botox injections.
What is interstitial cystitis and how is it treated?
Interstitial Cystitis is a clinical diagnosis characterized by irritative bladder symptoms such as urinary urgency, frequency, and hesitancy in the absence of infection. Research has shown the majority of patients who meet the clinical definition have pelvic floor dysfunction and myalgia. Therefore, the American Urologic Association recommends pelvic floor physical and occupational therapy as first-line treatment for Interstitial Cystitis. Patients will benefit from pelvic floor physical and occupational therapy and may also benefit from pharmacologic management or medical procedures such as bladder instillations.
Who is the Pelvic Health and Rehabilitation Team?
The Pelvic Health and Rehabilitation Center was founded by Elizabeth Akincilar and Stephanie Prendergast in 2006, they have been treating people with pelvic floor disorders since 2001. They were trained and mentored by a medical doctor and quickly became experts in treating pelvic floor disorders. They began creating courses and sharing their knowledge around the world. They expanded to 11 locations in the United States and developed a residency style training program for their employees with ongoing weekly mentoring. The physical and occupational therapistss who work at PHRC have undergone more training than the majority of pelvic floor physical and occupational therapistss and as a result offer efficient and high quality care.
How many years of experience do we have?
Stephanie and Liz have 24 years of experience and help each and every team member become an expert in the field through their training and mentoring program.
Why PHRC versus anyone else?
PHRC is unique because of the specific focus on pelvic floor disorders and the leadership at our company. We are constantly lecturing, teaching, and staying ahead of the curve with our connections to medical experts and emerging experts. As a result, we are able to efficiently and effectively help our patients restore their pelvic health.
Do we treat men for pelvic floor therapy?
The Pelvic Health and Rehabilitation Center is unique in that the Cofounders have always treated people of all genders and therefore have trained the team members and staff the same way. Many pelvic floor physical and occupational therapistss focus solely on people with vulvas, this is not the case here.
Do I need pelvic floor therapy forever?
The majority of people with pelvic floor dysfunction will undergo pelvic floor physical and occupational therapy for a set amount of time based on their goals. Every 6 -8 weeks goals will be re-established based on the physical improvements and remaining physical impairments. Most patients will achieve their goals in 3 – 6 months. If there are complicating medical or untreated comorbidities some patients will be in therapy longer.


Comments
My pelvic physiotherapist recommends Zestra. It’s great because it is lubido enhancing and works well as a water based nontoxic lubricant in menopausal women with history of vulvar vedtibulitis abd chronic pelvic pain.
A local naturopath says coconut oil can disrupt vaginal flora, so does not recommend it.
Any comments?
Author Melinda Fontaine says:
“Coconut oil has some anti-microbial properties, so yes, it can disrupt vaginal flora. Each person will respond differently, so for some people, coconut oil will work great. If you are having difficulties with vaginal flora, try stopping all lube for a while to see if that is contributing.”
since using coconut oil I have been free of yeast infections, which previously I’d suffered form regularly.
Thanks Melinda,
Such an informative and enlightening article written with great data and a fun sense of humor…. love it !
Katie Beckham
Really enjoyed this write-up. Was wondering if I could include the graph you’ve created in a presentation?
Hi Lianne,
Yes!
Thank you will share with my patients
I found this article extremely helpful. Thank you. It has made me reconsider my own clinical practice & the advice I sometimes give. Thank you!
Victoria