Table of Contents
-
.
-
.
-
.
-
.
-
.
-
.
-
.
-
.
-
.
When Should I See a Pelvic Floor Physical and Occupational Therapists?
-
.
Endometriosis and pelvic floor and girdle dysfunction are two conditions that often go hand in hand. In fact, research shows that up to 90% of people with endometriosis also experience pelvic floor and girdle dysfunction.
This overlap between two different conditions can exist because visceral (aka organ) pain from endometriosis lesions cause the pelvic floor and girdle muscles to involuntarily guard via the visceral-somatic reflex and tighten over time. Additionally, pain associated with menstruation may result in voluntary guarding. As those muscles become more tense or uncoordinated, pelvic floor and girdle dysfunction develops, creating somatic (muscular) pain that persists even beyond endometriosis flare-ups or treatment. Additionally, both conditions share symptoms like pelvic pain, discomfort with exercise or intimacy, and muscle tightness. Many people with biopsy-confirmed endometriosis understandably think all of their symptoms stem from the disease which can result in a missed therapeutic target of the pelvic floor and girdle muscles.
At PHRC, our team of pelvic floor physical and occupational therapists specializes in helping people navigate this overlap, identifying the role of the pelvic floor in endometriosis-related pain and creating pelvic floor therapy treatment plans that bring relief and restore function.
What is Endometriosis?
Endometriosis is a long-term inflammatory condition influenced by estrogen in which endometrial tissue (similar to the uterine lining) grows outside the uterus. These growths can develop on the ovaries, fallopian tubes, bladder, bowel, and pelvic walls, leading to irritation, scarring, and adhesions. The condition affects about 1 in 10 people assigned female at birth. While painful periods (dysmenorrhea) and infertility are the symptoms most often linked to the disease, many individuals also experience a wide range of other symptoms, often alongside overlapping pain conditions and pelvic floor disorders.
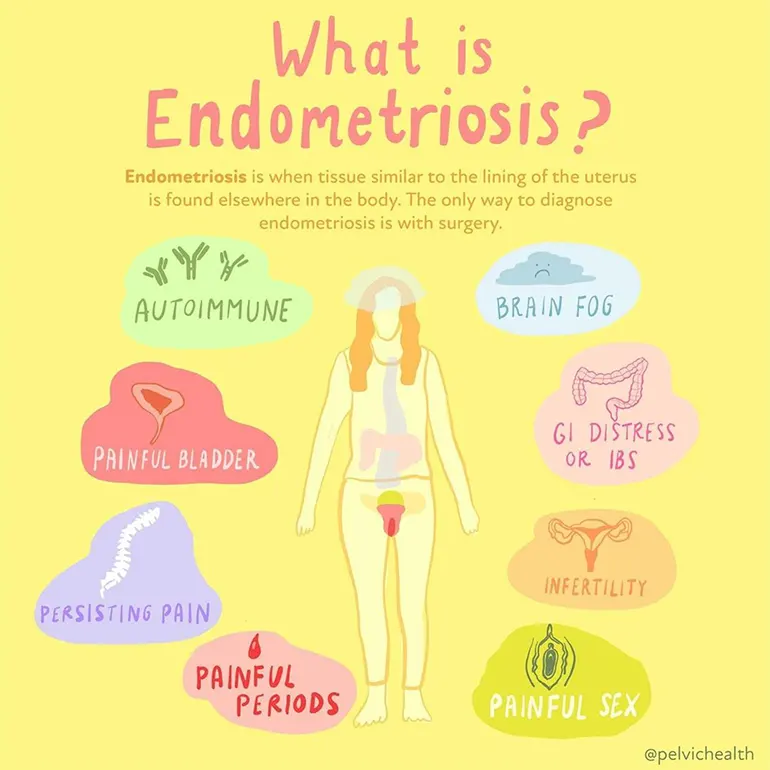
Symptoms of Endometriosis
The symptoms of endometriosis can vary. You might have only mild endometriosis symptoms or no symptoms at all. It’s important to note that the severity of symptoms does not correlate with the severity of the condition. For example, someone with advanced endometriosis might experience only mild discomfort, while another person with a mild, surgically confirmed case could feel severe abdominal and pelvic pain.
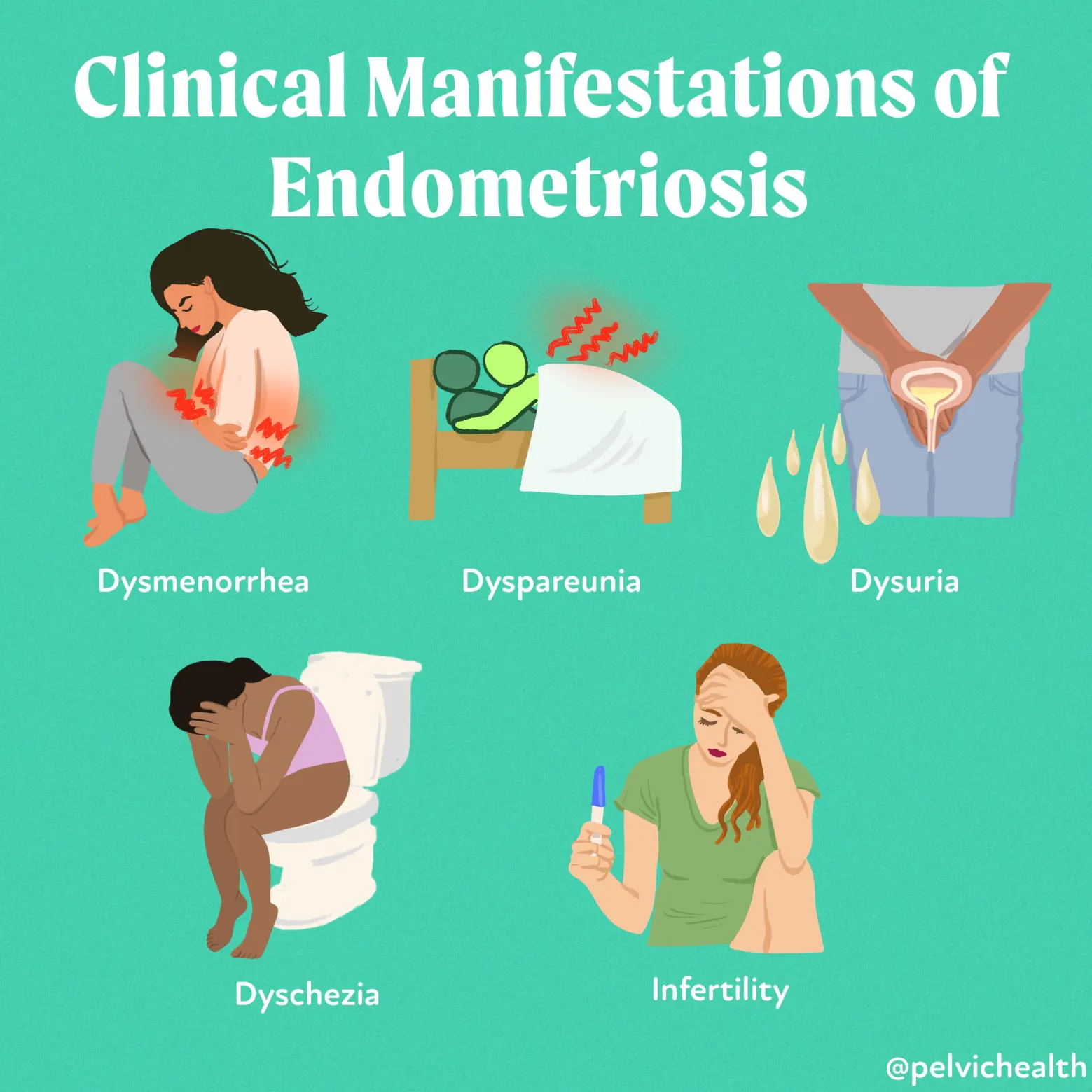
Some common symptoms people experience include:
- Painful periods (dysmenorrhea): Those with endometriosis often experience severe cramping, abdominal pain, and lower back pain during their menstrual cycles.
- Pelvic pain: Pelvic pain may occur not only during menstruation but also before or after it. The severity of pain can range from mild to debilitating.
- Pain during intercourse (dyspareunia): Endometriosis can cause pain during or after sexual intercourse. This can sometimes be felt deep within the pelvis.
- Pain during urination or bowel movements: Some experience pain while urinating or having a bowel movement, particularly during their periods.
- Excessive bleeding: Heavy menstrual bleeding (menorrhagia) or bleeding between periods (metrorrhagia) can be symptoms of endometriosis.
- Infertility: Endometriosis is a common cause of infertility as it can lead to adhesions and scar tissue that interfere with normal reproductive organ function.
- Fatigue: Many report chronic fatigue and low energy levels.
- Digestive issues: Can include bloating, constipation, diarrhea, and nausea, especially around menstruation.
- Irritative bladder symptoms: Urinary urgency, frequency, and pain without infection are common.
What is pelvic floor and girdle dysfunction?
The pelvic floor is a group of muscles and connective tissues that span the base of your pelvis. These pelvic muscles support the bladder, bowel, and, in women, the uterus. They play a very important role in controlling bladder and bowel movements, sexual function, and maintaining pelvic stability. The pelvic girdle muscles attach to the bony pelvis and can be accessed exteriorly. These muscle groups work together under normal circumstances and often become problematic together in dysfunctional situations.
When these muscles are too tight, weak, or uncoordinated, it can lead to many issues collectively referred to as pelvic floor and girdle dysfunction. In addition to pain, symptoms include urinary, bowel and sexual dysfunction.
Symptoms of Pelvic Floor and Girdle Dysfunction
Pelvic floor and girdle dysfunction can manifest in a wide range of symptoms, which generally fall into four categories: urinary, bowel, sexual dysfunction, and musculoskeletal pelvic pain.
- Urinary urgency, frequency, hesitancy, and pain in the absence of infection
- Weak urinary stream
- Leaking urine (incontinence)
- Urethra and bladder pain
- Pain before, during, or after urination
- Nocturia (nighttime urination)
- Pediatric bed wetting (nocturnal enuresis)
- Straining to evacuate stool
- Adult and pediatric constipation
- Need for excessive toilet paper
- Fecal and/or gas leakage and incontinence
- Hemorrhoids and fissures
- Pain before, during, or after bowel movements
- Anal/rectal pain, burning, or itching
- Discoloration in the penis/scrotum/perineum
Female Sexual Symptoms Can Include:
- Inability or decreased ability to lubricate
- Pain upon vaginal penetration, with deep penetration only, and/or continuous pain with penetration
- Clitoral pain, hypersensitivity to touch
- Pain and/or burning after sexual contact
- Inability to orgasm, diminished orgasm
- Urinary incontinence during sexual activity
- Climacturia (incontinence with orgasm)
Female Pelvic Pain Symptoms Can Include:
- Burning, itching, aching, or other types of pain in the vulva, vagina, perineal, and/or anal area
- Pain with intercourse, hypersensitivity when wearing pants and/or underwear, and pain with sitting
- Exercise may provoke or exacerbate symptoms
- Abdominal bloating, gastrointestinal distress, and constipation
- Symptoms can be provoked (with penetrative intercourse or tampon insertion) or unprovoked and spontaneous
- Symptoms can be intermittent or constant
Understanding the Overlap Between Endometriosis and Pelvic Floor and Girdle Dysfunction
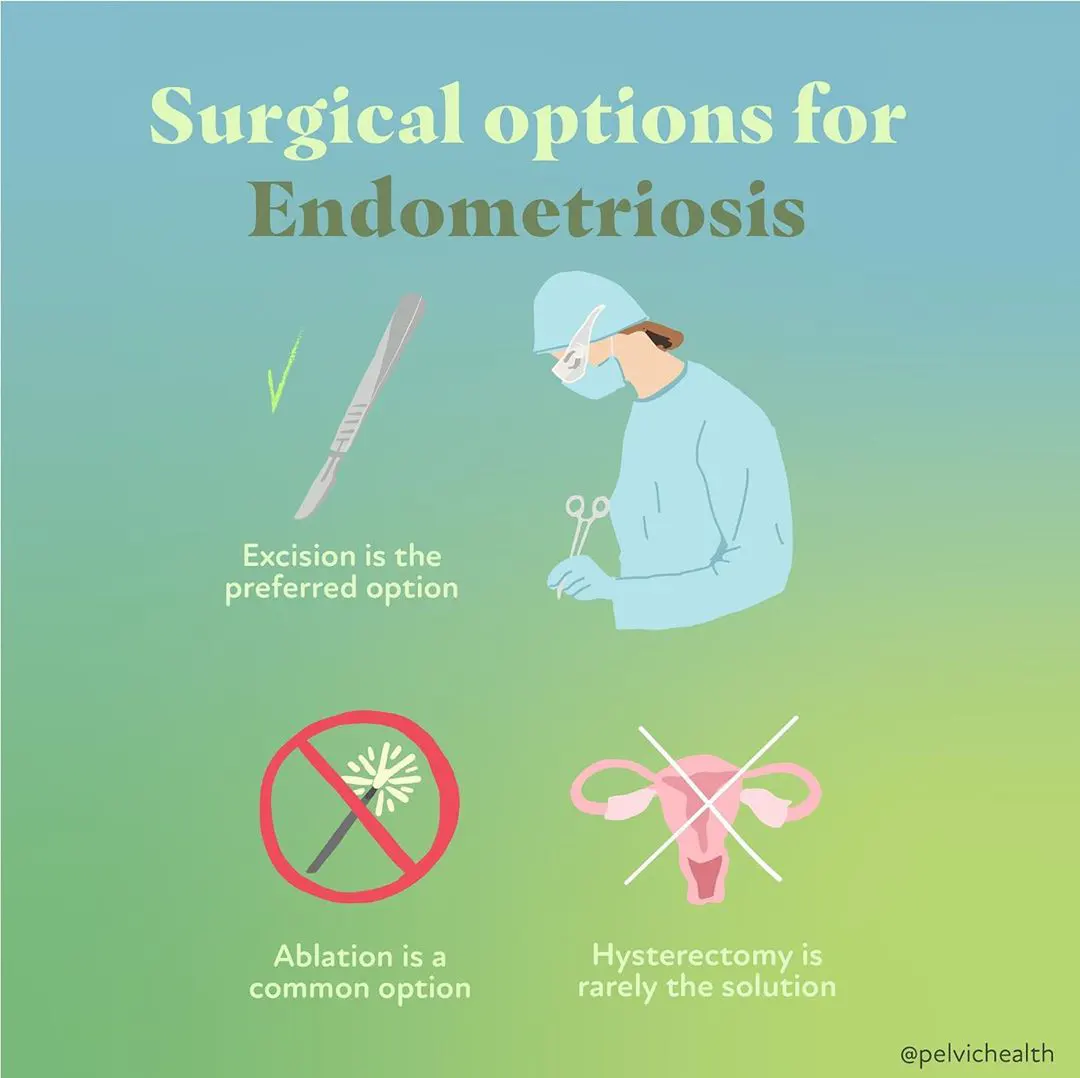
Diagnosing endometriosis can be very challenging, especially since its symptoms often resemble those of other pelvic and abdominal conditions. The gold standard for diagnosis and treatment is laparoscopic surgery with excision of lesions.
But even with surgery, many people continue to experience pelvic pain. That’s because endometriosis and pelvic floor and girdle dysfunction frequently feed into one another:
- Chronic inflammation and pain from endometriosis can cause the pelvic floor muscles to tighten in a protective response
- Over time, this guarding develops into pelvic floor and girdle dysfunction, which brings its own set of symptoms and cannot be resolved with surgery
- The two conditions often look alike, making it difficult to separate one from the other
- This cycle explains why many people with endometriosis also experience pelvic floor and girdle dysfunction
- Central Nervous System Dysregulation
Because multiple pain generators can exist at the same time (endometriosis lesions, muscle tension, nerve irritation, or overlapping bladder and bowel issues), removing lesions alone may not bring full relief. This is where a pelvic floor physical and occupational therapist can help.
Treatment for Endometriosis and Pelvic Floor and Girdle Dysfunction
On average, people wait 7 to 10 years before receiving an endometriosis diagnosis, and this long delay often allows pain to become deeply ingrained. Treatments with the goal of reducing symptoms (without addressing the underlying issues/weaknesses) can sometimes temporarily ease endometriosis-related pain but don’t necessarily provide long-term relief.
Since as many as 90% of those with endometriosis also experience pelvic pain or pelvic floor and girdle dysfunction, working with a pelvic floor physical and occupational therapist is an important part of addressing the bigger picture. Managing endometriosis isn’t only about treating the lesions themselves—it requires looking at all sources of pain to achieve the best results.
When you come to PHRC for your first visit, your pelvic floor physical and occupational therapist will begin by reviewing your medical history (including pelvic surgeries, childbirth, or chronic health conditions) to see how they connect to your current symptoms. If you’re dealing with urinary frequency, bowel changes, painful sex, or musculoskeletal pelvic pain, this conversation helps map out a clear direction for your care.

Next, your pelvic floor physical and occupational therapist will perform a pelvic floor evaluation. This includes evaluating muscles, tissues, and nerves for tightness, weakness, or imbalance, and checking how well your muscles coordinate during basic functions like urination, bowel movements, and sexual activity.
Based on these findings, we’ll create a personalized treatment plan. This might involve exercises to strengthen or relax the pelvic floor, manual therapy to release tension, or strategies that support muscle coordination. For urinary leakage, for example, your pelvic floor physical and occupational therapist might focus on bladder retraining and pelvic floor control, while bowel-related symptoms might call for relaxation techniques and improved muscle regulation.
Experiencing chronic pain can be frustrating, especially when you’ve been dealing with symptoms for a long time without help. Our team at PHRC is here to restore your pelvic floor function and reduce your pain.
Find Relief From PHRC
At PHRC, our goal is to provide compassionate and comprehensive care to help you manage and overcome pain from pelvic floor and girdle dysfunction, endometriosis, and other pelvic health conditions. By understanding the underlying causes and providing targeted treatments, our goal is to improve your quality of life and restore your health.
We also recognize the challenges some people might face in accessing in-person care, which is why we offer virtual sessions through telehealth after your initial consultation. These sessions allow for continuity of care and accessibility for those unable to travel to one of our clinics.

