By Stephanie Prendergast
Do women have a prostate? Where is the female prostate and what does it do? I have been a pelvic floor physical and occupational therapists for 17 years and, until recently, had never heard of such a structure.
Last month, Dr. Irwin Goldstein, urologist, sexual medicine enthusiast, and International Society for the Study of Women’s Sexual Health President, started an ISSWSH listserv thread titled “The Female Prostate”. This started an interesting discussion about anatomy, physiology, evolution, and ultimately, technical and political accuracy. I have a ‘thing’ for technical accuracy so I decided to write a blog post on the conversation.
Dr. Goldstein began the discussion with this email:
A colleague of mine was discussing this article (see abstract below) with a local urogynecologist – who while not disagreeing there is such an organ in a woman – was, on the other hand, quite “offended” that we use the anatomic term “female prostate”. From the MD’s perspective this was not the appropriate term for this organ in a woman. The fact is – we recently performed a literature search using the keywords “female prostate”, “Skene’s gland”, “peri-urethral gland”, and “G-spot”. Over 200 publications were found based on relevance. Categories for analysis included anatomy, physiology, embryology, pathology, neural innervation, adenomatous and cancerous changes, and orgasmic potential. More than 60 publications were included for review and analysis. Since 400 BCE scholars have proposed the existence of sexually sensitive homologous “female prostate” peri-urethral anterior vaginal wall tissue. Contemporary researchers have characterized “female prostate” exhibiting glandular and secretive elements identical to male prostate via immunohistochemical studies with prostate specific antigen (PSA), prostate specific acid phosphatase, androgen receptors, biochemical analyses of PSA and creatinine in female ejaculate as well as three-dimensional modeling and waxy casts. We concluded that the “female prostate” is embryologically and physiologically identical to male prostate. In some women, stimulation of “female prostate” via the anterior vaginal wall results in orgasm, analogous to stimulation of the anterior wall of the rectum resulting in orgasm in some men. The female prostate is not simply an incidental, vestigial organ; injury during surgical procedures may have clinical consequences, as peri-urethral anterior vaginal wall tissue possesses neurally-mediated sexually functional attributes. Despite skepticism, its existence is supported by extensive, reliable contemporary evidence.
THE QUESTION IS – TO ALL MEMBERS OF ISSWSH – DOES THE ANATOMIC USE OF THE TERM “FEMALE PROSTATE” OFFEND YOU???? I WOULD LIKE ALL COMMENTS.
Abstract
The female prostate was first described by Reijnier de Graaf in 1672, and even after several years this gland is still a matter of controversy. Part of this is because the biological function of this female gland is unclear. Moreover, when compared with the male prostate, the existence of this organ in females does not make sense, mainly when we consider that the major function of this gland is to produce a secretion that is responsible for guarantee the sperm survival and assure the reproductive success. However, even under a controversy field, we now have a lot of scientific information which enhances our knowledge of several important biological aspects of this gland. It is clear that this gland is found in some female mammals including humans, rodents, rabbits, bats and dogs. Several studies with rodents showed that the female prostate is the homologue of the male prostate, showing strong macroscopic and microscopic similarities with the ventral lobe of males. Besides these aspects, there are several studies reporting that diseases such as cysts, hyperplasia, and carcinoma may affect the female prostate. Therefore, although diseases involving the female prostate are rare, the susceptibility of this organ to develop lesions must be considered, especially in our recent years in which the exposure to endocrine-disrupting chemicals has greatly increased. Finally, further studies will be necessary to enhance our understanding about this gland, mainly of the developmental, evolutionary, and biological functions. (reference: Biancardi MF1, Dos Santos FC1, de Carvalho HF2, Sanches BD2, Taboga SR3. Female Prostate: historical, developmental, and morphological perspectives. Cell Biol Int. 2017 Mar 4. doi: 10.1002/cbin.10759. [Epub ahead of print])
A brief anatomy refresher may be useful:
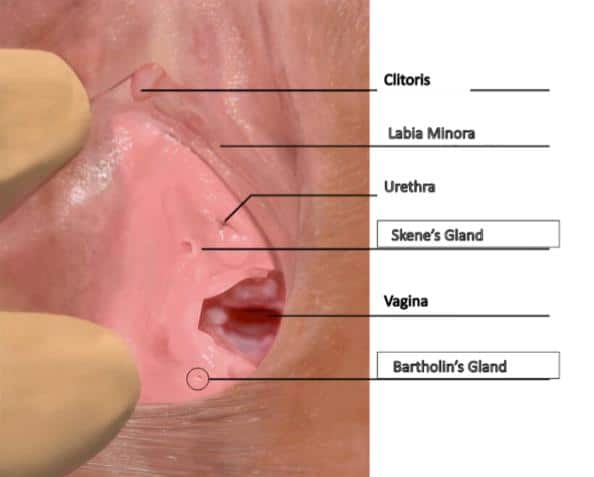
- Skene’s glands and the prostate gland have the same embryologic origin, they differentiate as mother nature dictates into anatomy specific to females and males, respectively
- Skene’s glands exist in women the anterior vaginal wall and secrete fluid that lubricates the urethra and vulva
- Skene’s glands may be responsible for female ejaculation
- Skene’s gland secretions contains prostatic acid phosphatase, prostate-specific antigen, and PDE5
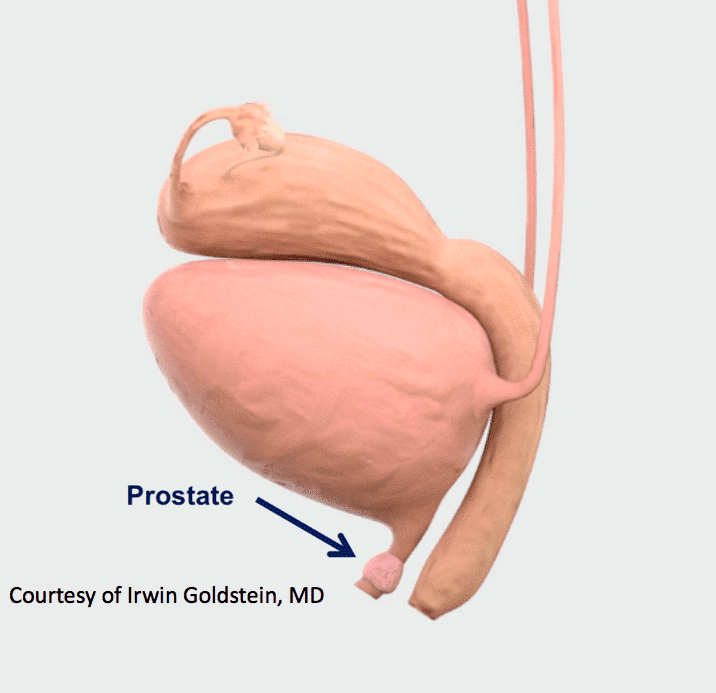
- The prostate gland exists in men below the urinary bladder and surrounds the urethra
- The prostate is responsible for reproductive success by secreting and alkaline fluid to protect sperm, its fluid makes up 30% of the composition of semen along with spermatozoa from the vas deferens and seminal vesicle fluid
- Prostate secretions include proteolytic enzymes, prostatic acid phosphatase, beta-microseminoprotein, and prostate-specific antigen
- The prostate contains smooth muscle to help with ejaculate propulsion
Obviously Skene’s glands and the prostate gland are not identical twins or even fraternal twins. However, they are somewhat homologous structures despite different physiological functions. Would it be technically accurate to consider them siblings?
Wikipedia insightfully adds the clitoris is homologous to the penis, however, the clitoris is not a penis. Um, thanks.
I spent some time pondering if it is technically accurate to call Skene’s glands the Female Prostate, thereby losing site of the original question. Is it offensive to call Skene’s glands ‘the female prostate’?
Here is what a few ISSWSH members had to say:
Barry R. Komisaruk, Ph.D.:
I think it is clear from all the evidence that the “female prostate” is, strictly biologically speaking, homologous with the “male prostate”. We could consider calling it “the prostate”, without the sexual modifier. We don’t attribute a sexual modifier to other organs, e.g., rectum, bladder, appendix, so perhaps we should not for the prostate, either. The fact that the possible function of the prostate in women is not known should not be a reason to provide it with a sexual modifier; the possible function of male nipples is not known, either, and we don’t use a sexual modifier for that body component. Are we ready to call it “the prostate” in women as well as in men?
Tarek Khalife, MD FACOG:
If I remember correctly and according to the presentation that you shared on one, or probably all, of the ISSWSH meetings, the female analogous organ to the male prostate was not just the Skene and peri-urethral glands, but also the vestibular glands scattered around the vestibule area. I hope I did not get that wrong!!
As a male, it does not offend me to use the term female prostate, yet that being said I think the term serves a purpose far beyond naming an organ that already has a name. The term “prostate” was more so to stress on the organs’ thirst for testosterone for proper function and health. Stressing on this homology helps providers and patients who might be skeptic with the treatment options that entail prescribing Male Hormones to Female patients.
If men would accept calling their testicles the Male Ovaries or penis: the Male Clitoris then women should be ok with calling their Skene’s Glands Female prostates or Ovaries the Female Testicles. The name calling does not sound right and I can understand the urogynecologist’s concern and see where she/he is coming from.
I do believe there is a lot to blame on the original sin of calling Testosterone the :Male hormone and Estrogen the Female hormone. These are just hormones and are present in both sexes and serve their purpose.
With continued resistance to assimilate the use of androgens in treatment of female sexual pain and sexual dysfunction when indicated, I find myself obliged to use the term Female Prostate with patients to help them understand how androgen use can help their symptoms. Not because I think the term female prostate is appropriate, but more so because its the closest functional descriptor I can use to-date.
Sue Goldstein:
We think of breasts as being part of the female anatomy, yet we use the word breast when describing that body part on the man because they are the same anatomy. This is no different—they are the same anatomy. The clitoris and penis may have had the same embryologic origins but they are not the same anatomy. We use the same word for every other body part that is the same, so why should this be different?
Robert Pyke:
It doesn’t offend me any more than “male menopause.” That’s the way language develops naturally, by analogy and metaphor more than by coining a whole new, and thus unfamiliar, term. Metaphorical terms help us understand things, like “inspiration” (in-breaths). We may in our scientific precise-ness want a whole new term, one that’s as descriptive as we can pack it, like “peri-urethral gland,” but we often fall short in these attempts: “peri-urethral” still doesn’t tell us that the intended structure is in females only!
Jim Pfaus, PhD:
Well… it might be good for convenience sake, but it is kind of useless from a functional, anatomical, and embryological sexual differentiation point of view. In mammals, males differentiate from a “female default phenotype.” Testes could become ovaries, but descend and differentiate into testes. Scrotal sac differentiates from labia. The penis is a prolapsed clitoris. The female ductwork withers away in the presence of androgens and Mullerian Inhibiting Substance. Without the influence of androgens and MIS, we would come out – like people with Androgen Insensitivity Syndrome – looking anatomically female despite being genetically male (XY).
Now, calling the clitoris a “female penis” is simply wrong from the standpoint of the process of sexual differentiation (calling the vagina an “inverted penis” is downright ludicrous). It is far more correct to call the penis a “male” clitoris, but even that is not really correct from an anatomical point of view (e.g., Mother Nature would never put the urethra through the glans of the clitoris!). Once differentiated they are just that – differentiated into something different. Are they functionally different? Both the penis and clitoris provide pleasure. Both have cavernosa that engorge with blood. The glans of both are connected via a dorsal nerve to the pudendal. So the penis and clitoris are derived from homologous tissue and have homologous function (with the exception of where the urethra is, and the fact that boys sometimes think their penises are a firehose… which girls generally do not feel about their clitorises). Likewise, the testes are makes of steroid hormones and gametes… as are their progenitors the ovaries. And hormonal secretion occurs with LH and gamete production with FSH. But the content is a tad different both in terms of hormone release and type of gamete produced. So you have homologous tissue rendering somewhat homologous function.
Now what about the prostate? Clearly Skene’s gland contains prostatic antigen, which suggests that it could be the progenitor of the prostate. And clearly it produces an exudate that can be found around the vagina. Does it enlarge with androgen? Does it induce an “ejaculate” at orgasm per se, or during sex in general? These could be easy to test. It may well be that the prostate is a male “Skene’s gland, though again, from an anatomical point of view this is erroneous given the size and particular hormonal responsiveness of the prostate.
Indeed, calling something a “female __________” with the blank being something male, harkens back to the book of Genesis/Bereshit, where women and her lady parts are made from man and his manly parts, and not the other way around. And here is the potentially offensive part: It assumes that the male thing is somehow more important, and that the female thing is a vestige or dinkier version of the male part. And this is simply not true. The Skene’s gland may well help to lubricate the vagina and labia, much as gentle muscular contractions of the prostate result in the emission of “precum” that lubricates the urethra. Again, this would result in the two being somewhat homologous in function, though skene’s gland secretions are not necessary for ova to be released and lodge in the uterine wall.
And Skene’s gland secretions may well mix with urine to become what people colloquially call “female ejaculate,” but the ejaculate volume and composition are somewhat different from male ejaculate. It is not as bad as analogy (e.g., between gills and lungs), but even as homologies, they are not really the same thing. So I fall on the side of NOT calling the G-spot/Skene’s glands/internal end of the clitoris are a “female prostate.” Cuz females don’t have prostates. They have their own gland from which the prostate may well differentiate.
Julie Dybbor, ARNP, PhD:
The reason it may be “offensive “ to some is the insinuation that, once again, the male version holds the default/normative position requiring no pre-requisite adjective. The female version of the ‘prostate’ certainly does not exist for the same purpose as it does in men, so perhaps we need an independent term that fits the anatomical/physiological function in the female, its raison d’être. My Mom was a pilot in the 2nd World War and she always thought it was so strange that the men were called “pilots”, and the women were “female pilots”, when they all flew the very same planes. The male prostate and the female prostate are not flying the same planes so we need a better moniker. Just because they look similar under the microscope does not mean they get to be called the same thing. “Sexually sensitive homologous “female prostate” peri-urethral anterior vaginal wall tissue” is too long of a name if you ask me, how about “Ante-eruptus”, since it usually kicks in just before orgasm and is often described as a feeling of extraordinary excitation that is distinct and just preceding the orgasm.
Barbra Taylor, MD:
I love Jim’s response. Qualifying any anatomical part as the “female version of the male anatomy” only serves to confuse and offend, no matter what the embryologic origin. It’s fine — in teaching anatomy — to define homologous structures or point out analogies. But to “name” an organ the female version of the male anatomy is just plain sad.
Surely we’re more sophisticated than that.
Jim Pfaus, PhD:
A bit of history then… Wilson (1992) specifically muses in his book about sex differences that the clitoris is a “vestigial penis” based on pleasure-inducing functionality. Many cultures viewed the clitoris as a “tiny phallus” for thousands of years, though debate arose starting with the 2nd Century physician Galen, who asserted that the vagina and NOT the clitoris was important for reproduction, therefore the vagina was the homology of the phallus (an “inverted phallus”) and that the clitoris was simply unimportant for reproduction since it only provided pleasure. This view was reiterated later on by physicians like Vesalius in the 16th Century, and managed to find their way into medical texts in the 19th Century (despite the obvious need for clitoral AND vaginal stimulation together to “treat” so-called “hysteria.”). For sure no one should refer to the clitoris as the “female penis” or as a “vestigial” anything. The fact that the popular media still do, and that a supposedly learned scholar used that term as recently as Wilson did, means that the perception is “out there” (like “the truth” in the X-Files).
I think if we want to call Skene’s glands a “prostate” we should see first if it responds to hormones the same way as in men, and if it has the same nerve innervation. We will also then have to differentiate it from the bulbs of the clitoris, which have sensory innervation that courses into the dorsal clitoral nerve, eventually hooking up with the pudendal. And for sure, we use the germ “gonad” for both ovary and testis, and castration for removal of either. So there are “gender neutral” terms that could be envisioned, applied, or even made up to be applied, to the Skene’s glad/prostate.
Laura Streicher, MD:
Jim Plaus has it exactly correct. Offensive or not, it is incorrect terminology. I do kind of like the idea of calling the penis the “male clitoris”
Sara Saunders, DPT:
Anatomy is not offensive.
Barbara Chubak, MD :
While I do not find the term “female prostate” “offensive” in itself, I do object to its use and would prefer that we as a group choose to use an alternative terminology for the relevant PSA- and androgen-sensitive vulvovaginal tissues.
You reference the history of the “female prostate” in anatomical literature to support the use of this term, but the history of medicine has a long and problematic record of using technical terminology to reinforce a notion that the female body is abnormal or derivative, compared to a male baseline by which normal structure and physiology are defined. For one excellent example of this phenomenon, please see this classic, but still very relevant paper by historians Lawrence and Bendixen:
http://digitalcommons.unl.edu/cgi/viewcontent.cgi?article=1034&context=historyfacpub
Rather than perpetuating the use of male-specific terminology to describe ambisexual homologous structures, which Lawrence and Bendixen describe as recapitulating broader social, political, and cultural injustices against women, I choose to describe female anatomical structures in their own terms, while acknowledging the many ways in which they are similar to male body parts. I find that thinking and talking about genital anatomy in this way is a helpful, not only to correct the endemic “othering” of normal female bodies, but also to create a discursive space for functionally normal bodies possessed of genital anatomy that does not fit binary sex norms, whether due to intersex/DSD or transgender.
While I absolutely agree that it is desirable to eliminate the gratuitous use of sexual adjectives as modifiers of sex-neutral structures, I argue again that it is inappropriate to use the term prostate to describe the relevant portion of female anatomy in this case. Convention dictates that body parts are named not for their biochemical characteristics, but for their gross appearance. Women do not have a structurally discrete prostate gland; men do. To insist that women have a prostate is, again, to define female anatomy in terms of male structure, and deny the value of female parts on their own merits.
Michael Perelman, MD:
Given the numerous good but differing arguments provided on this list so far regarding the nosology of the terms under question, I tend to agree with Barbara below. It is true that labeling these various female anatomic structures as either the “prostate” or “female prostate” is an extremely useful heuristic when teaching, in order to raise consciousness regarding the huge number of overlapping similarities between women and men; the suggestion that either of the terms should be used in anyway beyond colloquial is ill conceived in my opinion.
Another anonymous physician adds:
I wasn’t going to chime in until I shared this email thread with my wonderfully feminist daughter, who is a therapist, to get her point of view. She has heard her dad refer to medical parts and terms for 30 years and probably cringed many times!
But her take was great, I thought, as she suggested naming it the Organ of Graffenberg, and the reasoning was sound. It has a combination of recognition in both the lay and academic populace and because it is named after the discovering anatomist, it has gender neutrality. I agreed with her and shared my knowledge of anatomical structures that had been named after the (not always) original anatomist who had first identified it. Moreover, many of the organs had uncertain functions and physiologies at the time of discovery, so there is no need to “modernize’ the term.
And she’ll kill me for sharing this, but the rest is great! “We women have clitoral orgasms and vaginal orgasms and G spot orgasms…I’d like to see a prostate do any of THOSE! What woman needs one!” I know only an audience of sexual medicine experts will laugh along with me!
Indeed, a great discussion. After doing my own research I do not think it’s technically accurate to call the Skene’s Gland the ‘female prostate’. I believe the desire to call it this lies in the intention to better educate the medical community about female physiology, diseases, and treatments. The term ‘female prostate’ may be helpful for educational purposes outside of the medical community, helping people understand why certain women may benefit from testosterone or why oral contraceptives can be problematic to female genital anatomy.
I don’t find the term “female prostate” politically offensive but the technical inaccuracy bothers me. In 2002, the Federative International Committee on Anatomical Terminology actually renamed Skene’s glands the Female Prostate. I assume this was not universally accepted or this discussion would not be happening now in 2017.
Not enough is known inside or outside of the medical about women’s sexual function, dysfunction and pain. ISSWSH is charged with the task of addressing this terminology issue and we want to thank them for working hard on this topic and others to raise awareness and improve medical management.
FAQ
What are pelvic floor muscles?
The pelvic floor muscles are a group of muscles that run from the coccyx to the pubic bone. They are part of the core, helping to support our entire body as well as providing support for the bowel, bladder and uterus. These muscles help us maintain bowel and bladder control and are involved in sexual pleasure and orgasm. The technical name of the pelvic floor muscles is the Levator Ani muscle group. The pudendal nerve, the levator ani nerve, and branches from the S2 – S4 nerve roots innervate the pelvic floor muscles. They are under voluntary and autonomic control, which is a unique feature only they possess compared to other muscle groups.
What is pelvic floor physical and occupational therapy?
Pelvic floor physical and occupational therapy is a specialized area of physical and occupational therapy. Currently, physical and occupational therapistss need advanced post-graduate education to be able to help people with pelvic floor dysfunction because pelvic floor disorders are not yet being taught in standard physical and occupational therapy curricula. The Pelvic Health and Rehabilitation Center provides extensive training for our staff because we recognize the limitations of physical and occupational therapy education in this unique area.
What happens at pelvic floor therapy?
During an evaluation for pelvic floor dysfunction the physical and occupational therapists will take a detailed history. Following the history the physical and occupational therapists will leave the room to allow the patient to change and drape themselves. The physical and occupational therapists will return to the room and using gloved hands will perform an external and internal manual assessment of the pelvic floor and girdle muscles. The physical and occupational therapists will once again leave the room and allow the patient to dress. Following the manual examination there may also be an examination of strength, motor control, and overall biomechanics and neuromuscular control. The physical and occupational therapists will then communicate the findings to the patient and together with their patient they establish an assessment, short term and long term goals and a treatment plan. Typically people with pelvic floor dysfunction are seen one time per week for one hour for varying amounts of time based on the severity and chronicity of the disease. A home exercise program will be established and the physical and occupational therapists will help coordinate other providers on the treatment team. Typically patients are seen for 3 months to a year.
What is pudendal neuralgia and how is it treated?
Pudendal Neuralgia is a clinical diagnosis that means pain in the sensory distribution of the pudendal nerve. The pudendal nerve is a mixed nerve that exits the S2 – S4 sacral nerve roots, we have a right and left pudendal nerve and each side has three main trunks: the dorsal branch, the perineal branch, and the inferior rectal branch. The branches supply sensation to the clitoris/penis, labia/scrotum, perineum, anus, the distal ⅓ of the urethra and rectum, and the vulva and vestibule. The nerve branches also control the pelvic floor muscles. The pudendal nerve follows a tortuous path through the pelvic floor and girdle, leaving it vulnerable to compression and tension injuries at various points along its path.
Pudendal Neuralgia occurs when the nerve is unable to slide, glide and move normally and as a result, people experience pain in some or all of the above-mentioned areas. Pelvic floor physical and occupational therapy plays a crucial role in identifying the mechanical impairments that are affecting the nerve. The physical and occupational therapy treatment plan is designed to restore normal neural function. Patients with pudendal neuralgia require pelvic floor physical and occupational therapy and may also benefit from medical management that includes pharmaceuticals and procedures such as pudendal nerve blocks or botox injections.
What is interstitial cystitis and how is it treated?
Interstitial Cystitis is a clinical diagnosis characterized by irritative bladder symptoms such as urinary urgency, frequency, and hesitancy in the absence of infection. Research has shown the majority of patients who meet the clinical definition have pelvic floor dysfunction and myalgia. Therefore, the American Urologic Association recommends pelvic floor physical and occupational therapy as first-line treatment for Interstitial Cystitis. Patients will benefit from pelvic floor physical and occupational therapy and may also benefit from pharmacologic management or medical procedures such as bladder instillations.
Who is the Pelvic Health and Rehabilitation Team?
The Pelvic Health and Rehabilitation Center was founded by Elizabeth Akincilar and Stephanie Prendergast in 2006, they have been treating people with pelvic floor disorders since 2001. They were trained and mentored by a medical doctor and quickly became experts in treating pelvic floor disorders. They began creating courses and sharing their knowledge around the world. They expanded to 11 locations in the United States and developed a residency style training program for their employees with ongoing weekly mentoring. The physical and occupational therapistss who work at PHRC have undergone more training than the majority of pelvic floor physical and occupational therapistss and as a result offer efficient and high quality care.
How many years of experience do we have?
Stephanie and Liz have 24 years of experience and help each and every team member become an expert in the field through their training and mentoring program.
Why PHRC versus anyone else?
PHRC is unique because of the specific focus on pelvic floor disorders and the leadership at our company. We are constantly lecturing, teaching, and staying ahead of the curve with our connections to medical experts and emerging experts. As a result, we are able to efficiently and effectively help our patients restore their pelvic health.
Do we treat men for pelvic floor therapy?
The Pelvic Health and Rehabilitation Center is unique in that the Cofounders have always treated people of all genders and therefore have trained the team members and staff the same way. Many pelvic floor physical and occupational therapistss focus solely on people with vulvas, this is not the case here.
Do I need pelvic floor therapy forever?
The majority of people with pelvic floor dysfunction will undergo pelvic floor physical and occupational therapy for a set amount of time based on their goals. Every 6 -8 weeks goals will be re-established based on the physical improvements and remaining physical impairments. Most patients will achieve their goals in 3 – 6 months. If there are complicating medical or untreated comorbidities some patients will be in therapy longer.

Comments
What a great article.
Why the debate?
For simplicity’s sake, why not just call it a prostate as we do in men. After all, breasts are breasts in the male or female. Why must we always complicate things?
If you want to call my prostate a male prostate then fine. I still know what it is in a woman.By the way, I have male breasts. Am sure that name will make some people feel better.
Let’s spend this time on subjects that we can all learn from.
M.M. M.D.
Hi Michael,
Thanks for your comment. From my perspective, the structures in question are actually different, I think we should leave the anatomy termed Skene’s glands in women and the prostate gland in men. However, both structures need and secrete similar hormones to function optimally. The folks at ISSWSH work hard to improve the management of sexual health concerns in women, and for a long time testosterone was not considered necessary or important for women. Without putting words in their mouth, the anatomical terms matter if it affects medical management. Again, thanks for reading and for your comments.
Fantastic article. Ironically, the very first article that I placed on the IC Network back in 1996 or so was a discussion of this from the LA Times. In women who struggle with recurring urethral irritation, one of the things worth ruling out is an infection of the periurethral gland. I’ve worked with several women who had heterogenous colonies of pathogenic bacteria confirmed by culture. The challenge, of course, is expressing that fluid, usually with manual manipulation (catheter in urethra, finger in vagina pushing against the gland to drain it). Biofilms are likely present as well.