By Joshua Gonzalez, MD
The advent of oral birth control pills in the 1960s was heralded as a huge victory for women’s rights. Finally, women could take control of their bodies and their fertility. Since then, oral contraceptive pills (OCPs) have become ubiquitous in reproductive aged women with nearly 10 million women today using The Pill as their primary means of contraception (Guttmacher).
Unfortunately, most of those women have no idea how these medications work and often have not been told of their potential side effects. Worse yet, many women are given oral birth control pills for non-contraceptive reasons: erratic mood, recurrent migraines, irregular menses, menstrual cramping, endometriosis, and even acne. Starting in adolescence, OCPs are handed out to women like candy. Women can spend many years in their young adult lives on these medications simply because they haven’t been properly counseled on alternative forms of contraception.
So what’s the big deal? Why should you be worried if you’re on an OCP? Well, let’s talk about how these medications work. OCPs are drugs mostly comprised of synthetic hormones. That is, fake hormones. These medications trick your ovary into thinking there’s enough real hormone around by exposing it to a hormone-like compound. Consequently, ovarian production of very important sex steroid hormones stops, as does ovulation. Hence, no pregnancy!
The problem is that your body needs sex steroid hormones for lots of different things. Estrogen, progesterone, and testosterone are all important for the health of a woman’s body. Yes, I said testosterone (more on that later). These hormones are important for bone health, cardiovascular health, libido, mood, cognition, and especially the health of the genital tissues. And when the body isn’t exposed to these hormones, like when you’re on an OCP, there can be consequences.
One recent study found that women using a hormonal contraceptive method experienced less frequent sexual activity, arousal, pleasure, and orgasm and more difficulty with lubrication (Smith). It is not uncommon for young women on OCPs to report pain with intercourse (called dyspareunia) as well. Some women may not experience dyspareunia but can present with other symptoms like urinary urgency, urinary frequency, recurrent urinary tract infections (UTI) or yeast infections. All of these things can happen with OCP use, but often go unrecognized or ignored.
To understand why this happens, one must appreciate the anatomy of the genital tissues and how they respond differently to specific hormones. These details are not known by most patients on OCPs and often are lost on the physicians who prescribe these medications.
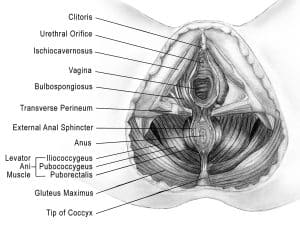
The female genitalia are comprised of three unique anatomic structures: the vulva, the vagina, and the vestibule. Each of these tissues arise from different embryological structures during fetal development. And each of these tissues respond uniquely to specific sex steroid hormones.
The vulva and vagina primarily rely on estrogen to maintain their health. When a woman goes through menopause and her ovary stops producing estrogen, these tissues can become dry, inflamed, chronically irritated, and literally shrink (atrophy). Similar things can happen to younger women on an OCP. When these tissues are chronically irritated they become a breeding ground for bacteria and yeast and can lead to recurrent infections. The lack of estrogen can also cause less vaginal lubrication, which can lead to pain with sexual activity.
The vestibule is a thin rim of tissue at the opening of the vagina. If you’ve never heard of it, you’re not alone. It is often ignored and easily missed during routine pelvic exams. Your gynecologist probably went right by it when she inserted that speculum. But it can cause even more problems than the vulva and vagina combined. The vestibule is an area responsible for mucus secretion, which provides lubrication during sexual activity. It is an area also intimately related to the urethra, the opening to the bladder that you urinate from. And unlike the vulva and vagina it is an area rich in testosterone receptors. When vestibular tissue is unhealthy, like when there are low levels of circulating testosterone caused by OCP use, it too becomes chronically inflamed or irritated. This can lead to pain with penetration and/or urinary symptoms that can be incorrectly assumed to be a UTI or yeast infection.
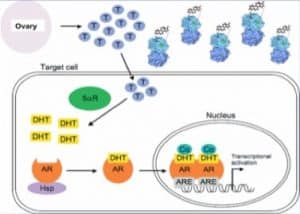
But the real damage of OCPs is their effect on a naturally occurring protein in your body called sex hormone binding globulin (SHBG). SHBG is a protein in the blood that binds testosterone and renders it inactive. Only a small amount of the testosterone your ovary makes then is actually used by the body. The rest is bound to SHBG. When women take OCPs, their SHBG skyrockets! Many physicians who prescribe these medications do not appreciate this point. With higher SHBG levels, more testosterone is bound and not usable by the body. OCPs already decrease ovarian testosterone production and now most of what’s left of your testosterone is being gobbled up by all the SHBG floating around. Worse yet, SHBG levels often remain elevated even after OCP discontinuation.
Many women I’ve treated have been misdiagnosed for years, told they have recurrent UTI or yeast infections or interstitial cystitis. Their physicians failed to appreciate that their symptoms were primarily a hormonal deficiency and that their OCP use was to blame. If you’re on The Pill now or were at one time you could be at risk. If you recognize or have experienced any of the symptoms I’ve mentioned, it’s worth discussing this with your health care provider. If they don’t believe you or have never heard of these potential adverse effects from OCPs, then maybe it’s time to find a new provider.
Case Example:
One particular patient stands out in my mind. When we first met, CL was 24 years old and had already been struggling with the effects of her birth control for more than two years. She first noticed pain in her vulva and vestibule (termed vulvodynia and vestibulodynia, respectively) during and after sexual intercourse. The pain was mild at first, but then intensified and lasted for longer periods as time went on. Soon she could barely sit more than a few minutes before a similar raw, burning pain would suddenly flare. She started avoiding sex and noticed a significant decrease in her libido. She began experiencing urinary frequency and urgency too. She was told by numerous physicians that she had recurrent urinary tract and yeast infections, prescribed countless rounds of antibiotics and fluconazole. She was even diagnosed and treated for interstitial cystitis. Despite being dismissed by many, she knew all the while the problem had not been addressed. This problem wasn’t in her head and it certainly wasn’t an infectious issue. Her problem was The Pill. When I first explained the real cause of her symptoms, CL cried both tears of sadness and relief.
Women have stayed quiet about these issues for far too long because they think painful sex or recurrent infections are “normal.” They’re not. I have no doubt that The Pill did a great deal for women’s reproductive rights, but at what cost? With alternative methods of contraception—non-hormonal, often more reliable methods—why are we still so quick to prescribe these jagged little pills. They may be easy for women to take, but the consequences may be ultimately too hard to swallow.
Continue on to Part Two: Treatment solutions and alternative birth control options here.
Additional reading:
In 2015 an International Consensus Conference on Vulvar Pain was held to examine levels of evidence surrounding causes of vulvar pain and associated factors. During this meeting, it was decided that hormonal insufficiencies can cause vulvar pain. The details and resource list have been published in three locations, the references are listed below.
http://www.nva.org/wp-content/uploads/2015/01/2015_ISSVD_ISSWSH_and_IPPS_Consensus_Terminology.2.pdf
http://www.sophiebergeron.ca/images/publications/Pukall_2016_Vulvodynia.pdf
American College of Obstetrics and Gynecology: http://www.sophiebergeron.ca/images/publications/Bornstein_2015_ISSVD.pdf
References.
- https://www.guttmacher.org/united-states/contraception
- Smith NK, Jozkowski KN, Sanders SA. Hormonal contraception and female pain, orgasm and sexual pleasure. J Sex Med. 2014 Feb;11(2):462-70.
FAQ
What are pelvic floor muscles?
The pelvic floor muscles are a group of muscles that run from the coccyx to the pubic bone. They are part of the core, helping to support our entire body as well as providing support for the bowel, bladder and uterus. These muscles help us maintain bowel and bladder control and are involved in sexual pleasure and orgasm. The technical name of the pelvic floor muscles is the Levator Ani muscle group. The pudendal nerve, the levator ani nerve, and branches from the S2 – S4 nerve roots innervate the pelvic floor muscles. They are under voluntary and autonomic control, which is a unique feature only they possess compared to other muscle groups.
What is pelvic floor physical and occupational therapy?
Pelvic floor physical and occupational therapy is a specialized area of physical and occupational therapy. Currently, physical and occupational therapistss need advanced post-graduate education to be able to help people with pelvic floor dysfunction because pelvic floor disorders are not yet being taught in standard physical and occupational therapy curricula. The Pelvic Health and Rehabilitation Center provides extensive training for our staff because we recognize the limitations of physical and occupational therapy education in this unique area.
What happens at pelvic floor therapy?
During an evaluation for pelvic floor dysfunction the physical and occupational therapists will take a detailed history. Following the history the physical and occupational therapists will leave the room to allow the patient to change and drape themselves. The physical and occupational therapists will return to the room and using gloved hands will perform an external and internal manual assessment of the pelvic floor and girdle muscles. The physical and occupational therapists will once again leave the room and allow the patient to dress. Following the manual examination there may also be an examination of strength, motor control, and overall biomechanics and neuromuscular control. The physical and occupational therapists will then communicate the findings to the patient and together with their patient they establish an assessment, short term and long term goals and a treatment plan. Typically people with pelvic floor dysfunction are seen one time per week for one hour for varying amounts of time based on the severity and chronicity of the disease. A home exercise program will be established and the physical and occupational therapists will help coordinate other providers on the treatment team. Typically patients are seen for 3 months to a year.
What is pudendal neuralgia and how is it treated?
Pudendal Neuralgia is a clinical diagnosis that means pain in the sensory distribution of the pudendal nerve. The pudendal nerve is a mixed nerve that exits the S2 – S4 sacral nerve roots, we have a right and left pudendal nerve and each side has three main trunks: the dorsal branch, the perineal branch, and the inferior rectal branch. The branches supply sensation to the clitoris/penis, labia/scrotum, perineum, anus, the distal ⅓ of the urethra and rectum, and the vulva and vestibule. The nerve branches also control the pelvic floor muscles. The pudendal nerve follows a tortuous path through the pelvic floor and girdle, leaving it vulnerable to compression and tension injuries at various points along its path.
Pudendal Neuralgia occurs when the nerve is unable to slide, glide and move normally and as a result, people experience pain in some or all of the above-mentioned areas. Pelvic floor physical and occupational therapy plays a crucial role in identifying the mechanical impairments that are affecting the nerve. The physical and occupational therapy treatment plan is designed to restore normal neural function. Patients with pudendal neuralgia require pelvic floor physical and occupational therapy and may also benefit from medical management that includes pharmaceuticals and procedures such as pudendal nerve blocks or botox injections.
What is interstitial cystitis and how is it treated?
Interstitial Cystitis is a clinical diagnosis characterized by irritative bladder symptoms such as urinary urgency, frequency, and hesitancy in the absence of infection. Research has shown the majority of patients who meet the clinical definition have pelvic floor dysfunction and myalgia. Therefore, the American Urologic Association recommends pelvic floor physical and occupational therapy as first-line treatment for Interstitial Cystitis. Patients will benefit from pelvic floor physical and occupational therapy and may also benefit from pharmacologic management or medical procedures such as bladder instillations.
Who is the Pelvic Health and Rehabilitation Team?
The Pelvic Health and Rehabilitation Center was founded by Elizabeth Akincilar and Stephanie Prendergast in 2006, they have been treating people with pelvic floor disorders since 2001. They were trained and mentored by a medical doctor and quickly became experts in treating pelvic floor disorders. They began creating courses and sharing their knowledge around the world. They expanded to 11 locations in the United States and developed a residency style training program for their employees with ongoing weekly mentoring. The physical and occupational therapistss who work at PHRC have undergone more training than the majority of pelvic floor physical and occupational therapistss and as a result offer efficient and high quality care.
How many years of experience do we have?
Stephanie and Liz have 24 years of experience and help each and every team member become an expert in the field through their training and mentoring program.
Why PHRC versus anyone else?
PHRC is unique because of the specific focus on pelvic floor disorders and the leadership at our company. We are constantly lecturing, teaching, and staying ahead of the curve with our connections to medical experts and emerging experts. As a result, we are able to efficiently and effectively help our patients restore their pelvic health.
Do we treat men for pelvic floor therapy?
The Pelvic Health and Rehabilitation Center is unique in that the Cofounders have always treated people of all genders and therefore have trained the team members and staff the same way. Many pelvic floor physical and occupational therapistss focus solely on people with vulvas, this is not the case here.
Do I need pelvic floor therapy forever?
The majority of people with pelvic floor dysfunction will undergo pelvic floor physical and occupational therapy for a set amount of time based on their goals. Every 6 -8 weeks goals will be re-established based on the physical improvements and remaining physical impairments. Most patients will achieve their goals in 3 – 6 months. If there are complicating medical or untreated comorbidities some patients will be in therapy longer.


Comments
Hi Dr. Gonzalez – I have a specific question that may get answered in your follow-up blog so feel free to ask me to wait.
My wife started on the Pill when she was 25 or so and was on it for a couple of years. She used to have a high libido and we both noticed that it pretty much went out the window so she stopped. She is now 35 and her libido has never returned to the way it was before. I’m sure there are various contributing factors (e.g. stress with work, though no kids right now), but she feels pretty strongly that it was the pill. This has caused occasional strain in our marriage as my libido is strong while hers is low.
Any suggestions?
Thanks
Author Dr. Gonzalez says:
“Thank you for your post. Your wife’s use of the Pill in her 20s could certainly have negative effects on her libido. As my blog mentioned, the effects of the Pill can last for a long time after discontinuation. The Pill can cause an elevation in sex hormone binding globulin (SHBG) that persists for years. The SHBG binds up most of the circulating testosterone (T) and effectively puts your wife in a chronic low T state. T is extremely important for a healthy libido and without it, I wouldn’t be surprised if your wife continues to struggle with low libido.
My suggestion is that you have her come see me or another specialist in this field. If you are not local and are looking for someone closer to you, please see the various websites I included in the blog. You can search for local physicians on several of the sites.
Good luck!”
I was put on birth control for endometriosis at the age of 17. I have suffered all of the mentioned consequences in addition to PGAD, PERSISTENT GENITAL AROUSAL DISORDER. it appalls me that we have more and more suffering from this in their early 20’s in addition to very young children. Thank you for this article It’s too bad ACOG, the American College of Obstitrcians and Gynocologists won’t even address these pelvic issus much less pelvic pain.
I have a really bad bladder pain that flares up if I’m on an OCP. How do I know if I have interstitial cystitis or if it’s something else? I should also note that not being on OCP relieves a lot of my bladder pain and discomfort, but does not take it away completely. I still have days where I have a flare and I’m not on the pill. At this point I can’t tell if it’s my birth control, my hormones, or what that’s triggering this bladder pain.
Hi Marelisa,
A pelvic floor physical therapist would be able to help you. Please use the link below to find one in your area.
https://pelvicguru.com/2016/02/13/find-a-pelvic-health-professional/
Regards,
Admin
Hello!
I am so grateful I found this article. I am 23 years old and have been battling awful bladder and Vulvar pain for 3 months. My question is, what is the treatment for this?? I have stopped the pill but am definitely still experiencing the symptoms of IC.
Hi Emmie,
We recommend being evaluated by a pelvic floor physical therapist, you can use the link below to find one in your area.
https://pelvicguru.com/2016/02/13/find-a-pelvic-health-professional/
Regards,
Admin
Hey Emmie,
I’m suffering the same symptoms. Did they go away once you stopped bc?
Hello I started gederal the oral contraceptive pill and almost immediately got a UTi that lasted a month, now after sex I get discomfort up my urethra and the urge to urinate but no infection. Could this be my pill causing this. I am at my wits end. HELP!!!