Asking patients about pain is a major component of an initial evaluation as well as with follow-up treatments. Monitoring changes in pain behavior, the intensity and the location can help gauge treatment success and progress. However, not a lot of people are aware of a major source of pain which is visceral pain. Kevin Hellman, PhD from NorthShore University Health System gave an excellent lecture at IPPS 2018 on visceral pain. Today, I’m going to share the information I gleaned from his lecture so that we can answer the questions of why does this happen and how does this happen?
Visceral pain is characterized by pain elicited from organs. Think pain from the bladder, the intestine, the stomach or even the heart.
There are several different mechanisms which cause visceral pain.
Hypersensitivity
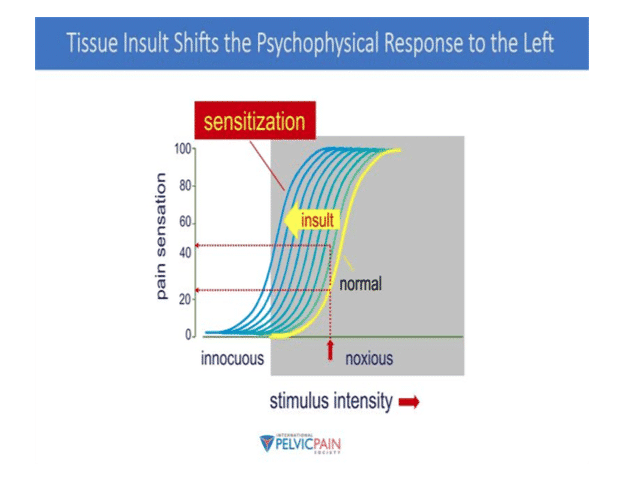
Hypersensitivity is when the tissue becomes more sensitized to a noxious (painful) stimulus. Think about it this way, if you were to poke your thumb with a thumbtack you would perceive a certain amount of pain as you push down on the tack which is a normal reaction. However, with repeated exposure the tissue on your thumb becomes more and more sensitive; this requires you to press less on the tack. Eventually your thumb is so sensitive that by just brushing your thumb by the tack you perceive pain. The same thing occurs with organs, with repeated exposure the tissue becomes more sensitive and is able to handle less intense stimulus.
Visceromotor Reflex
This reflex is defined as increased tension and tone of the tissues in the abdominal muscles resulting from a painful stimulus to an organ. This is why if you experience intense intestinal cramping the muscles lying on top of your abdomen feel rock hard. It is important to treat not just the viscera themselves but the overlying skeletal muscle to reduce pain.
Colonic pH
If high school or college chemistry was a distant bad memory let’s review what pH is and the purpose of it in our bodies. A pH level measures how acidic or alkaline something is, with 0 being completely acidic and 14 being completely alkaline, while a pH of 7 is neutral. The normal arterial blood range for a human is 7.35-7.45 depending on the source with the defined normal pH for a person is 7.4. The pH for the stomach is a lot lower – 3.5 since its job is to break down foods. The pH changes throughout the gastrointestinal tract – from a pH of 6 in the small intestine, to 5.7 in the caecum and a 6.7 in the rectum. The changes in pH throughout the tract are normal as the job of each organ changes. However, if your pH becomes altered this can cause significant pain and symptoms. Two of the studies Dr. Hellman cited demonstrated that patients with IBS have consistently altered pH levels throughout their colons.
Finally, what the heck do we do with all this information? How do we treat patients when all of these different mechanisms are working together to create pain?

Dr. Hellman did a great job concluding that a multidisciplinary approach is key to treatment. As of right now we don’t have the scientific tools to definitively determine which types of patients would benefit from which corresponding treatment. Therefore patients should be given a comprehensive evaluation and multimodal treatments should be used to target a patient’s symptoms. You’ll notice that Physical and Occupational Therapy is listed as one of these key treatments!
FAQ
What are pelvic floor muscles?
The pelvic floor muscles are a group of muscles that run from the coccyx to the pubic bone. They are part of the core, helping to support our entire body as well as providing support for the bowel, bladder and uterus. These muscles help us maintain bowel and bladder control and are involved in sexual pleasure and orgasm. The technical name of the pelvic floor muscles is the Levator Ani muscle group. The pudendal nerve, the levator ani nerve, and branches from the S2 – S4 nerve roots innervate the pelvic floor muscles. They are under voluntary and autonomic control, which is a unique feature only they possess compared to other muscle groups.
What is pelvic floor physical and occupational therapy?
Pelvic floor physical and occupational therapy is a specialized area of physical and occupational therapy. Currently, physical and occupational therapistss need advanced post-graduate education to be able to help people with pelvic floor dysfunction because pelvic floor disorders are not yet being taught in standard physical and occupational therapy curricula. The Pelvic Health and Rehabilitation Center provides extensive training for our staff because we recognize the limitations of physical and occupational therapy education in this unique area.
What happens at pelvic floor therapy?
During an evaluation for pelvic floor dysfunction the physical and occupational therapists will take a detailed history. Following the history the physical and occupational therapists will leave the room to allow the patient to change and drape themselves. The physical and occupational therapists will return to the room and using gloved hands will perform an external and internal manual assessment of the pelvic floor and girdle muscles. The physical and occupational therapists will once again leave the room and allow the patient to dress. Following the manual examination there may also be an examination of strength, motor control, and overall biomechanics and neuromuscular control. The physical and occupational therapists will then communicate the findings to the patient and together with their patient they establish an assessment, short term and long term goals and a treatment plan. Typically people with pelvic floor dysfunction are seen one time per week for one hour for varying amounts of time based on the severity and chronicity of the disease. A home exercise program will be established and the physical and occupational therapists will help coordinate other providers on the treatment team. Typically patients are seen for 3 months to a year.
What is pudendal neuralgia and how is it treated?
Pudendal Neuralgia is a clinical diagnosis that means pain in the sensory distribution of the pudendal nerve. The pudendal nerve is a mixed nerve that exits the S2 – S4 sacral nerve roots, we have a right and left pudendal nerve and each side has three main trunks: the dorsal branch, the perineal branch, and the inferior rectal branch. The branches supply sensation to the clitoris/penis, labia/scrotum, perineum, anus, the distal ⅓ of the urethra and rectum, and the vulva and vestibule. The nerve branches also control the pelvic floor muscles. The pudendal nerve follows a tortuous path through the pelvic floor and girdle, leaving it vulnerable to compression and tension injuries at various points along its path.
Pudendal Neuralgia occurs when the nerve is unable to slide, glide and move normally and as a result, people experience pain in some or all of the above-mentioned areas. Pelvic floor physical and occupational therapy plays a crucial role in identifying the mechanical impairments that are affecting the nerve. The physical and occupational therapy treatment plan is designed to restore normal neural function. Patients with pudendal neuralgia require pelvic floor physical and occupational therapy and may also benefit from medical management that includes pharmaceuticals and procedures such as pudendal nerve blocks or botox injections.
What is interstitial cystitis and how is it treated?
Interstitial Cystitis is a clinical diagnosis characterized by irritative bladder symptoms such as urinary urgency, frequency, and hesitancy in the absence of infection. Research has shown the majority of patients who meet the clinical definition have pelvic floor dysfunction and myalgia. Therefore, the American Urologic Association recommends pelvic floor physical and occupational therapy as first-line treatment for Interstitial Cystitis. Patients will benefit from pelvic floor physical and occupational therapy and may also benefit from pharmacologic management or medical procedures such as bladder instillations.
Who is the Pelvic Health and Rehabilitation Team?
The Pelvic Health and Rehabilitation Center was founded by Elizabeth Akincilar and Stephanie Prendergast in 2006, they have been treating people with pelvic floor disorders since 2001. They were trained and mentored by a medical doctor and quickly became experts in treating pelvic floor disorders. They began creating courses and sharing their knowledge around the world. They expanded to 11 locations in the United States and developed a residency style training program for their employees with ongoing weekly mentoring. The physical and occupational therapistss who work at PHRC have undergone more training than the majority of pelvic floor physical and occupational therapistss and as a result offer efficient and high quality care.
How many years of experience do we have?
Stephanie and Liz have 24 years of experience and help each and every team member become an expert in the field through their training and mentoring program.
Why PHRC versus anyone else?
PHRC is unique because of the specific focus on pelvic floor disorders and the leadership at our company. We are constantly lecturing, teaching, and staying ahead of the curve with our connections to medical experts and emerging experts. As a result, we are able to efficiently and effectively help our patients restore their pelvic health.
Do we treat men for pelvic floor therapy?
The Pelvic Health and Rehabilitation Center is unique in that the Cofounders have always treated people of all genders and therefore have trained the team members and staff the same way. Many pelvic floor physical and occupational therapistss focus solely on people with vulvas, this is not the case here.
Do I need pelvic floor therapy forever?
The majority of people with pelvic floor dysfunction will undergo pelvic floor physical and occupational therapy for a set amount of time based on their goals. Every 6 -8 weeks goals will be re-established based on the physical improvements and remaining physical impairments. Most patients will achieve their goals in 3 – 6 months. If there are complicating medical or untreated comorbidities some patients will be in therapy longer.


Comments
Thanks for this fascinating update! I missed going to the IPPS this year and really appreciate your sharing this great info!
Nice summary of Dr Hellman’s lecture. Glad to see physical therapists getting the attention they deserve and a piece of the action. Medicine alone just doesn’t help these complicated problems.
Very useful information! Very nice explain! I’m sure doctor Julia Zaitsev treats her patients with a great knowledge and passion and respect!