Chronic Prostatitis! It’s not something discussed at a baseball game or at a family gathering. However, it is estimated that between 2-14% of men worldwide are diagnosed with chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS)1. But what exactly is CP/CPPS? According to the National Institutes of Health, CP/CPPS, also known as category III prostatitis, is characterized by pain in the pelvic area for 3 of the last 6 months without any signs of infection, malignancy, or structural abnormalities 2. In fact, it is the number one reason why men under the age of 50 visit a urologist. 95% of men with a “prostatitis” diagnosis actually have CPPS and in fact have NOTHING wrong with the prostate itself. Instead, there are almost always problems with the musculoskeletal system, including the pelvic floor muscles.
Men with CP/CPPS report genital and urinary symptoms including the following:
- Urinary frequency
- Urinary urgency
- Burning sensation with urination
- Hesitancy with starting stream
- Incomplete emptying of the bladder
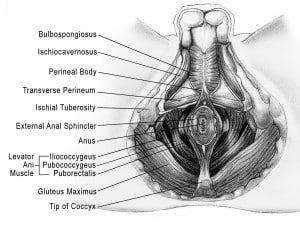
- Pain in the perineum – region between the testicles and anus
- Pain in the genital region
- Pain in the lower abdomen and/or low back
- Pain with ejaculation
- Pain with bowel movements
- Erectile dysfunction
How is CP/CPPS Diagnosed?
Medical doctors will conduct a systemic workup to exclude other possible diagnoses, such as cancer, painful bladder syndrome, or bowel pathologies. An extensive workup may consist of a urinalysis and culture, PSA study, cystoscopy, different types of imaging, such as a transrectal ultrasound, and any other studies a doctor may deem necessary. He/she will also conduct a thorough history exam asking questions regarding symptoms, past medical history, psychosocial history, family history, and medication. It is best to report all of your medical history to your doctor, even the things you might not find significant, such as cardiovascular disease or irritable bowel syndrome (IBS). Researcher are finding a correlation between CP/CPPS and other systems in the body, such as the gut and cardiovascular system. It is necessary to address and treat all impairments found when treating a patient with CP/CPPS.
Men with CP/CPPS have varying causes of their symptoms and therefore one standard treatment protocol, such as antibiotics, does not work for everyone. Repeated courses of antibiotics without a positive infection is NOT acceptable treatment. Research shows CP/CPPS is multifaceted with varying presentations. It is important to acknowledge and treat all possible causes of the symptoms.
The UPOINT classification system was created to help guide multimodal therapy for CP/CPPS. UPOINT is an acronym for urinary, psychosocial, organ-specific, infection, neurologic/systemic, and tenderness of muscles. These are all areas that can contribute towards CP/CPPS symptoms and need to be addressed. Research has shown that pelvic floor physical and occupational therapy is the FIRST line of treatment for the musculoskeletal impairments commonly found with CP/CPPS.
A physical and occupational therapists’s evaluation consists initially of a subjective exam. A PT will ask questions similar to the doctor’s history exam. We will want to know more about the behavior of the urinary, sexual, and pain symptoms, such as the quality, location, frequency, and severity of the pain, history of the symptoms, such as when they began, past medical history including surgeries and/or other injuries, psychosocial history, and questions regarding medication.
Next, a physical exam is conducted, which consists of an observation of the body looking for any abnormalities from the head down to the feet, an assessment of the pelvic girdle alignment (checking to see if the hips are in alignment), an assessment of the range of motion of the hips and low back, as well as palpation of the muscles in the abdomen, low back, hips, buttocks, thighs, and pelvic floor. When we palpate muscles, we are looking for tenderness, tightness, and myofascial trigger points in the muscles. Here at PHRC, we also assess for connective tissue restrictions throughout the abdomen, thighs, buttocks, low back, and bony pelvis. Please see our blog The Role of Connective Tissue Manipulation to learn more.
During the physical exam, an intrarectal exam is also performed to assess the pelvic floor muscles. We once again are looking for tightness, tenderness, and myofascial trigger points as well as pudendal nerve hypersensitivity. It is also important to assess motor control of the pelvic floor. Can our patient contract, relax, and lengthen the pelvic floor muscles when we ask him to? A primary goal of physical and occupational therapy is to teach our patients how to regain control of their muscles in order to reduce their symptoms and improve muscle function.
What is physical and occupational therapy treatment?
Physical therapy treatment focuses on the neuromuscular impairments. It is very common for men experiencing CP/CPPS to present with increased muscle tone and myofascial trigger points, connective tissue restrictions, and altered peripheral nerve function throughout the pelvic girdle area, abdomen, pelvic floor muscles, and thighs. Manual therapy, especially intrarectal manual therapy, is often necessary to normalize these impairments. Training patients to voluntarily relax and lengthen the pelvic floor is also a must. It is common for patients experiencing pain to guard, which contributes towards pelvic floor tightness and trigger points. Men suffering from CP/CPPS benefit from learning to relax their pelvic floor muscles since these muscles play such a large role in their pain. We call this exercise “Pelvic Floor Dropping” and we teach our patients how to do this early on in their treatment plan. To learn how to do a pelvic floor drop please click here.
More often than not, the symptoms of CP/CPPS are associated with tight muscles rather than weak muscles. Therefore, the majority of men suffering from CP/CPPS will likely NOT need to perform Kegels as part of their treatment program.
How long is this going to take?
Typically, men with CP/CPPS have physical and occupational therapy 1 -2 times per week, usually for 3 – 6 months. The timeline will vary based on the chronicity, severity, and other contributing factors.
Men with CP/CPPS may have multiple impairments contributing towards the pain, such as inflammation, stress/anxiety, gut pathology, infection, systemic pain, for example chronic fatigue syndrome. A multidisciplinary approach is the most effective strategy when confronted with multiple causes of pain. Part of our job as a PHRC physical and occupational therapists is to coordinate the overall treatment plan with other providers that our patients are being treated by. Other treatments may include acupuncture, pharmaceutical management, procedures such as trigger point injections, botox injections, nerve blocks, and psychological services such as cognitive behavioral therapy.
Will prostatitis ever go away?
YES! Physical therapy involves developing an assessment as to how the symptoms developed and what impairments need to be treated. This open discussion between the physical and occupational therapists and the patient leads to the development of reasonable short term and long terms goals and a strategy for achieving these goals. Although improvement does not happen overnight, it does happen!
CP/CPPS may not be a common subject spoken about at the water cooler, however for millions of men around the world it is a part of their daily life. These men do not have to live with the symptoms. Treatment is available!
Readers we want to hear from you! If you have any questions regarding CP/CPPS, please do not hesitate to leave them in the comment section below.
And if you haven’t already, SUBSCRIBE to this blog (up top, to the right, under Stephanie’s photo!), so you can get weekly updates in your inbox, and follow us on Facebook and Twitter where the conversation on pelvic health is ongoing.
- Konkle, K. and Clemens, J. New Paradigms in Understanding Chronic Pelvic Pain Syndrome. Curr Urol Rep. 2011 Aug; 12 (4): 278-83.
- Pontari, M. and Giusto, L. New Developments in the Diagnosis and Treatment of Chronic Prostatitis/Chronic Pelvic Pain Syndrome. Curr Opin Urol. 2013 Nov; 23 (6): 565-9.
FAQ
What are pelvic floor muscles?
The pelvic floor muscles are a group of muscles that run from the coccyx to the pubic bone. They are part of the core, helping to support our entire body as well as providing support for the bowel, bladder and uterus. These muscles help us maintain bowel and bladder control and are involved in sexual pleasure and orgasm. The technical name of the pelvic floor muscles is the Levator Ani muscle group. The pudendal nerve, the levator ani nerve, and branches from the S2 – S4 nerve roots innervate the pelvic floor muscles. They are under voluntary and autonomic control, which is a unique feature only they possess compared to other muscle groups.
What is pelvic floor physical and occupational therapy?
Pelvic floor physical and occupational therapy is a specialized area of physical and occupational therapy. Currently, physical and occupational therapistss need advanced post-graduate education to be able to help people with pelvic floor dysfunction because pelvic floor disorders are not yet being taught in standard physical and occupational therapy curricula. The Pelvic Health and Rehabilitation Center provides extensive training for our staff because we recognize the limitations of physical and occupational therapy education in this unique area.
What happens at pelvic floor therapy?
During an evaluation for pelvic floor dysfunction the physical and occupational therapists will take a detailed history. Following the history the physical and occupational therapists will leave the room to allow the patient to change and drape themselves. The physical and occupational therapists will return to the room and using gloved hands will perform an external and internal manual assessment of the pelvic floor and girdle muscles. The physical and occupational therapists will once again leave the room and allow the patient to dress. Following the manual examination there may also be an examination of strength, motor control, and overall biomechanics and neuromuscular control. The physical and occupational therapists will then communicate the findings to the patient and together with their patient they establish an assessment, short term and long term goals and a treatment plan. Typically people with pelvic floor dysfunction are seen one time per week for one hour for varying amounts of time based on the severity and chronicity of the disease. A home exercise program will be established and the physical and occupational therapists will help coordinate other providers on the treatment team. Typically patients are seen for 3 months to a year.
What is pudendal neuralgia and how is it treated?
Pudendal Neuralgia is a clinical diagnosis that means pain in the sensory distribution of the pudendal nerve. The pudendal nerve is a mixed nerve that exits the S2 – S4 sacral nerve roots, we have a right and left pudendal nerve and each side has three main trunks: the dorsal branch, the perineal branch, and the inferior rectal branch. The branches supply sensation to the clitoris/penis, labia/scrotum, perineum, anus, the distal ⅓ of the urethra and rectum, and the vulva and vestibule. The nerve branches also control the pelvic floor muscles. The pudendal nerve follows a tortuous path through the pelvic floor and girdle, leaving it vulnerable to compression and tension injuries at various points along its path.
Pudendal Neuralgia occurs when the nerve is unable to slide, glide and move normally and as a result, people experience pain in some or all of the above-mentioned areas. Pelvic floor physical and occupational therapy plays a crucial role in identifying the mechanical impairments that are affecting the nerve. The physical and occupational therapy treatment plan is designed to restore normal neural function. Patients with pudendal neuralgia require pelvic floor physical and occupational therapy and may also benefit from medical management that includes pharmaceuticals and procedures such as pudendal nerve blocks or botox injections.
What is interstitial cystitis and how is it treated?
Interstitial Cystitis is a clinical diagnosis characterized by irritative bladder symptoms such as urinary urgency, frequency, and hesitancy in the absence of infection. Research has shown the majority of patients who meet the clinical definition have pelvic floor dysfunction and myalgia. Therefore, the American Urologic Association recommends pelvic floor physical and occupational therapy as first-line treatment for Interstitial Cystitis. Patients will benefit from pelvic floor physical and occupational therapy and may also benefit from pharmacologic management or medical procedures such as bladder instillations.
Who is the Pelvic Health and Rehabilitation Team?
The Pelvic Health and Rehabilitation Center was founded by Elizabeth Akincilar and Stephanie Prendergast in 2006, they have been treating people with pelvic floor disorders since 2001. They were trained and mentored by a medical doctor and quickly became experts in treating pelvic floor disorders. They began creating courses and sharing their knowledge around the world. They expanded to 11 locations in the United States and developed a residency style training program for their employees with ongoing weekly mentoring. The physical and occupational therapistss who work at PHRC have undergone more training than the majority of pelvic floor physical and occupational therapistss and as a result offer efficient and high quality care.
How many years of experience do we have?
Stephanie and Liz have 24 years of experience and help each and every team member become an expert in the field through their training and mentoring program.
Why PHRC versus anyone else?
PHRC is unique because of the specific focus on pelvic floor disorders and the leadership at our company. We are constantly lecturing, teaching, and staying ahead of the curve with our connections to medical experts and emerging experts. As a result, we are able to efficiently and effectively help our patients restore their pelvic health.
Do we treat men for pelvic floor therapy?
The Pelvic Health and Rehabilitation Center is unique in that the Cofounders have always treated people of all genders and therefore have trained the team members and staff the same way. Many pelvic floor physical and occupational therapistss focus solely on people with vulvas, this is not the case here.
Do I need pelvic floor therapy forever?
The majority of people with pelvic floor dysfunction will undergo pelvic floor physical and occupational therapy for a set amount of time based on their goals. Every 6 -8 weeks goals will be re-established based on the physical improvements and remaining physical impairments. Most patients will achieve their goals in 3 – 6 months. If there are complicating medical or untreated comorbidities some patients will be in therapy longer.


Comments
This is me to a tee. Started with car accident and the force jammed my leg functional length was the same but left leg presented1/2 shorter. Then came Bacterial Prostatitis. Then the Chronic recurrent diagnosis was next. Finally it burned out at four years duration. Now 23 years later found a therapist who has treated internal trigger points. At first it was very painful and now my body has relaxed and finally has given me relief and my left leg at times resumes comparable length to the right one. 1992 until 2015 is my duration and only recently has this treatment started to come into its own.
Hello Mark,
Thank you for sharing your story! I am happy to hear that you have found a PF therapist who has helped you. Yes, it has taken some time for the medical community to understand all of the dimensions behind pelvic floor dysfunctions, but thanks to many technological and scientific advancements, more information is now available for patients and providers alike. We hope our blog can continue to share such vital information in order to better inform our readers.
Kindly,
Malinda
I saw stretches and exercises on the site but now I cannot find them. Would you tell me how to get there?
Hello Wayne,
You can perform a keyword search on our blog, and it will pull up the results for every exercise related blog we have written. There are several, so it is hard for me to guess which one you are referring to and provide you a link.
Regards,
Malinda
You still didn’t answer my question where are the structures on this website .I saw him before but I can’t find out please respond. Also what word do I search for defined the stretches.? Let me know where you to search thank you Wayne
Hello Wayne,
You did not mention “structures” before, and Im afraid I do not know what you are referring to. Below is a link to our exercise blogs:
https://pelvicpainrehab.com/?s=exercise
Regards,
Malinda
Malinda, do you have a reference for that “95% of men don’t actually have anything wrong with the prostate” statement? Or is it part of the Pontari article? Thanks!
Hello Ann,
Yes! The statistic is a quote from A Headache in the Pelvis:
Wise D and Anderson RU: A Headache in the Pelvis: A New Understanding and Treatment for Chronic Pelvic Pain Syndromes, 6th edition. National Center for Pelvic Pain, 2010.
Kindly,
Malinda
i’m a 35 year old guy who has been going to a physical therapist for pelvic pain/prostatitis for 3+ months now. I’ve also been dealing with mild anxiety and depression off and on for 5 years or so. My pelvic condition is mild and is mostly just a squirmish discomfort in my groin when sitting on hard surfaces for long periods of time and a bit of post-urination anxiety and tension in my penis. In my sessions we’ve been doing stretches, external massages, leg and pelvic exercises, and TENS unit stuff. Over the course of therapy i have had some minor relief. However, most of what we’ve been doing ranges from being only mildly beneficial at best (stretches and massaging) to actually making things worse (kegels, drinking more water when i’m already drinking a plenty). What helps the best, better than anything the therapist has had me do, is to gently massage my groin and buttocks in a warm bath, and to masturbate regularly (which i have no problem with) both which my urologist suggested. The therapist also tried internal message for several minutes in an earlier session but i nearly had a panic attack and was anxious and physically nauseous for days afterwards. It bordered on traumatic, even though i have no history of sexual or physical abuse. I have one more, final session with this therapist in a few weeks. She said we’ve done everything there is to do except internal massage and all i can do is keep up with the stretching and exercises she taught me. But what really bothered me is that she told me the ONLY way to get my pain down to 0 would be to start doing internal work. She realizes that is difficult for me, and she certainly isn’t trying to force it on me, but i just felt very angry that she presented this as the only choice i have to completely free myself of the pain. I feel that internal work is too disruptive to my body and would definitely make me feel significantly worse almost immediately. I’d bet my pelvic floor pain is closely tied to my anxiety and i cannot possibly agree with her that something that would cause such a significant surge in my anxiety would somehow be dramatically offset by the massaging of my internal muscles. Additionally i’m not all that confident in the therapy i’ve already received given how minorly effective it’s been. I understand that it may work for some but i fail to see how she can be so certain that internal massage will be the magic cure for me and how she can be so oblivious to the anxiety it caused me even after we discussed it and i’ve discussed my past anxiety issues with her. Given all the time and money i put into therapy to feel better, as it’s nearing its end I feel angered and annoyed that i’m being told that something that makes me fill ill IS the missing ingredient. Do i honestly need to subject myself to internal massage to feel better?
Hello Caesar,
Internal manual therapy is an essential part of treatment that helps our patients significantly. However, addressing your anxiety will also be a key component for you. Please read our blog on male anatomy, and pelvic pain for a better explanation. Additionally, I recommend that you look to Dr.Lorimer Moseley’s book for helpful tools to address your anxiety.
https://pelvicpainrehab.com/male-pelvic-pain/2911/a-cock-in-the-hen-house-a-look-inside-the-male-anatomy/
http://www.noigroup.com/en/Product/EPBII
Youtube Video of Dr. Lorimer Moseley:
https://www.youtube.com/watch?v=gwd-wLdIHjs
Regards,
Malinda
I am a 63 year old male. I have been treated for prostatitis and sciatica since I was 28 years old. When my wife and I got married we bought a washing machine. While loading it on my truck my friend dropped his side and I tried to catch the washer by myself. The next morning the left side of my lower back and hip were killing me. I hace seen chiropractors regularly since then with very little results. I have all the symptoms of CPPS. Could that injury have caused this? I have had multiple cystoscopys, Prostate resection ( TURP ) and been on antibiotics for up to 8 weeks at a time with no improvements in symptoms. Is there anyone in Memphis, TN that you could reccomend that could help me?
Hello John,
Here are the therapists we recommend in your area:
Nieves Alfredo MD Chattanooga TN (423) 4901136 [email protected] Pelvic Pain and Reconstructive Surgery Center
Kubic Melissa PT Chattanooga TN (423)778-8660 [email protected]
Best,
Malinda
Hi Malinda. I am a 68 year old male that has been tortured by what has been described as chronic prostatitis since I was 24 years old. The pain at times has been excruciating and my past is littered with lost opportunities and relationships. The pain never leaves me, only varying in intensity. I have seen multiple urologists and have taken every antibiotic known to man with little success. I am retired now but there were many, many days I would drag my body to work praying to God that he would give me the strength to bear the pain. I have read about pelvic floor therapy and myofascial release and have come to believe that there must be some connection between what I am experiencing and some malfunction in the pelvic floor. I have worked in electronic problem solving my entire life and I know that no problem exists without a specific cause. Finding the cause can be extremely troublesome but a cause exists none the less and applying the same measures to a problem over and over again with no good result can only lead a reasonable person to suspect they are applying the wrong measures. Time for something new. I live in southern New Jersey in Camden county but have been unable to find someone who knows Myofascial release techniques or how to explore the pelvic floor properly for any abnormalities. If you can help me I would be most grateful. Thank you in advance for caring about us males and for all your work in this area.
Hi Barry,
We recommend Michelle Dela Rosa, DPT in Columbus, NJ. Her number is (609) 379-0900.
Regards,
Admin
Hi Melinda,
I have been having a feeling of constant sensitive bladder need to urinate. My urologist said it’s sensory urgency and gave me MedI cation. I have had this for 18months a PT said I had pelvic floor dysfunction. This all started with bad back pains for months then it disappeared and left me with this. I do have a small prolapsed disc and small bulge disc in lumbar region. I am currently seeing a specialist who I can only see once a month, but see an oesteopath 1 x per week. My back always feel stiff. Will I ever get better ? What csn I do at home? Will oesteopath help? And what should they be doing?
Author Malinda Wright says:
Hi Bejamin,
I’m sorry to hear about the urinary urgency and frequency. I recommend seeing a pelvic floor physical therapist for an evaluation of your pelvic floor. To understand what pelvic floor physical therapy should consist of, please check out this blog. There are things you can do at home, however we first need to find out if your pelvic floor is weak or tight. I highly recommend seeing a pelvic floor PT in your area. If you need help finding someone in your area, please let us know.
Kindly,
-Malinda
Hello, I pelvic floor PT did say there pretty certain i have PFD. My question is also, can prolapsed discs in Lumbar region or a bulged disc cause PFD?
Author Malinda Wright says:
Yes, they can be related. When we feel pain in our backs, we tend to guard with other muscles to protect the injury. The pelvic floor can go into this guarded and protective position, which is a contracted position. Overtime, holding your pelvic floor in a guarded position can lead to trigger points, aka muscle spasms, creating pelvic floor dysfunction.
Kindly,
-Malinda