By Maryssa Steffen, DPT, PHRC Berkeley
“It doesn’t matter how much you drive around, you will never get to where you want to go if you don’t have the right map.” – Stanley Rosenberg
During this unprecedented time to slow down, shelter at home, and physical distance, I have taken the opportunity to dive deeper into embodied practices. In other words, I am interested in an integrated and embodied approach to movement, the body and consciousness. There are many paths that guide this type of work, but my recent journey has led me to Stephen Porges and his Polyvagal Theory. Proposed in 1994, it connects the dots between our internal organs and our emotional states.
The vagus nerve links our autonomic nervous system to our emotions and behavior and this theory has provided a map for psychotherapists, doctors, physical and occupational therapistss, and caregivers, to name a few. It is neurobiological evidence for the mind-body connection! I believe anyone may benefit from this knowledge, especially if they are experiencing chronic pelvic pain. Let me explain…
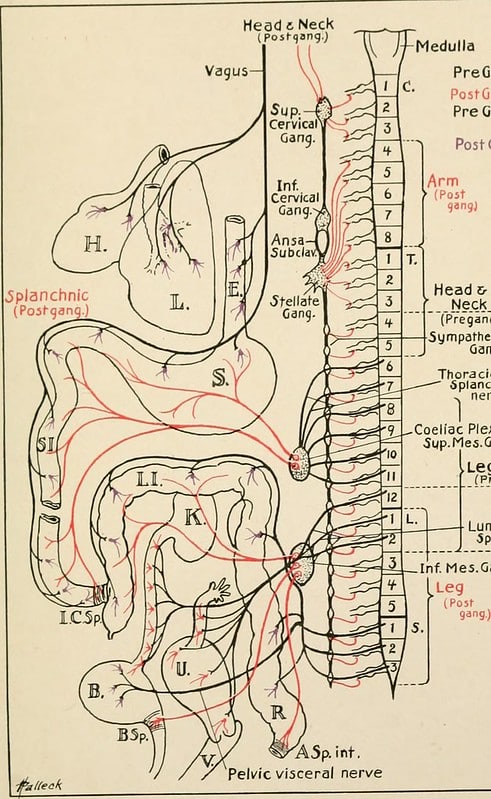
Before I get into what the Polyvagal Theory is, below is a picture of the vagus nerve so that you can appreciate how the longest cranial nerve travels from our brainstem to our pelvis:
Image courtesy of Flickr
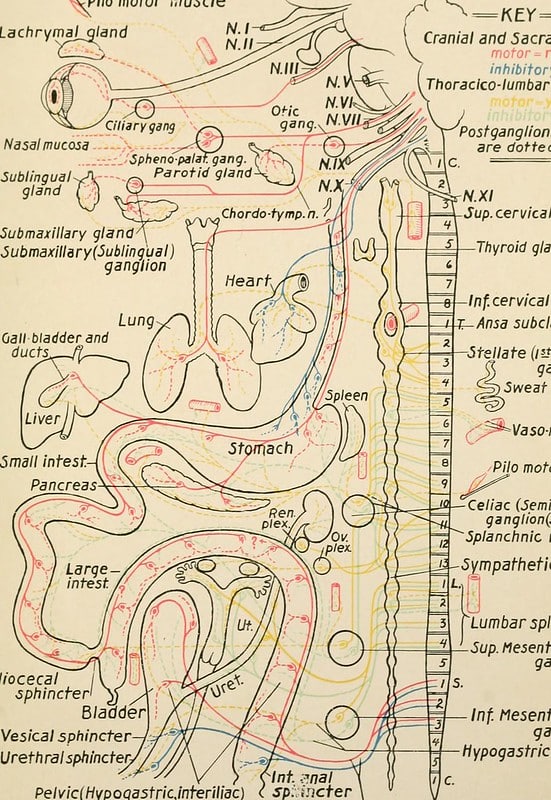
Next, you need to visualize the autonomic nervous system, which is the regulatory force governing sympathetic and parasympathetic nervous system states. The sympathetic and parasympathetic nervous system functions are described next.
Image courtesy of Flickr
Ok, now that you see this mind-body network, I will introduce you to Porges’s theory, which explains how the autonomic nervous system is supported by the three vagus nerve subsystems. The communication between the vagus nerve and the autonomic nervous system influences our behaviors, emotions, and perceptions. Here are the three vagal subsystems:
-
- The dorsal-vagal system. This is the most primitive of these three systems, originating about 600 million years ago in evolutionary biology. It is designed to immobilize and conserve energy during a shutdown state. Think about a lizard when you startle it in its tracks; it freezes! During that process, the dorsal-vagal system targets the internal organs and slows them down. If threatened, our heart rate decreases, breathing slows, and, in trauma, we often also experience fear, a sense of numbness and shutting down. In contrast, without fear, this system allows us to enjoy low-arousal activities, such as relaxation, meditation, restorative yoga and low-arousal emotions such as peaceful, calm, and contemplative states.
- The sympathetic nervous system. After the dorsal-vagal system developed in the evolutionary timeline, the sympathetic nervous system was next and it evolved from the reptilian period of about 400 million years ago. When this system is activated, it arouses the individual to prepare for mobilization and action. Blood is shunted towards our limbs to prepare for fight or flight. When our environment is absent of fear, this system gets us ready to engage in highly stimulating activities such as sports, dance, invigorating debates, and feel high-arousal emotions such as joy and elation.
- Ventral-vagal system. This phylogenetically most recent system (deriving from about 200 million years ago) exists only in mammals. It manages complex social and attachment behaviors. This branch of the vagus nerve activates our parasympathetic nervous system state, or “rest and digest.” A fun fact is that this ventral system links the cranial nerves to sound perception, vocalization, and facial expressions. That is why music and singing can be therapeutic and why bonding with others is possible when we feel safe and comfortable. Curiosity and play are alive in this state. Porges has cleverly referred to this integrated function as the social engagement system.
Whew! Are you still with me? So what does all of this have to do with chronic pelvic pain? Next, I will define neuroception, a term coined by Stephen Porges, which describes how our nervous system determines if a situation is safe or not. Our autonomic nervous system is always gathering information from our senses about our environment and the state of our body. We are not always conscious of this nervous system activity, which is why it is called autonomic! It is the difference between being on high alert or numb when our survival is compromised or in a friendly conversation when we feel safe. These switches between vigilance and comfort are super fast as our autonomic nervous system appraises cues from the environment.
Now, consider when we are in pain for longer than a couple of months, have unresolved trauma, or are under stress for extended periods of time at work or at home. In these unfortunate circumstances, we may not be able to regulate our own autonomic nervous system effectively because we did not have the chance to run from the threat or to shake it off. Rather than mobilize away from the threat, fear, or stress, our body is stuck in a dorsal-vagal or sympathetic nervous system loop. In this case, we may suffer from recurring inappropriate behaviors and constant physical symptoms of stress or shutdown. Over time, the accumulation of stress leads to an increase in different signs and symptoms of an unregulated autonomic nervous system and may help to explain the mysteries of why some individuals can develop chronic fatigue syndrome, fibromyalgia, migraines, and irritable bowel syndrome after months, or more, of these recurring triggers.
Alright! You made it this far, now what is the solution? We know that over 80% of the vagus nerve sends sensory information from various organs to our brain. Part of this intricate process involves the diaphragm, the breathing muscle. To learn more about the diaphragm and how it relates to pelvic floor function, check out this blog, https://pelvicpainrehab.com/low-tone-pelvic-floor-dysfunction/4427/diaphragmatic-deep-belly-breathing-pelvic-pain-pee-poop/.
Once you know the diaphragm’s function, you can use it to regulate your nervous system because the vagus nerve also plays a role in breathing. There are sensory nerve fibers in the vagus nerve that constantly detect the movements of breathing. When we perform diaphragmatic breathing patterns, our organs tell our brain that we are safe via the ventral-vagal branch. On the other hand, if we chest breathe, the muscles involved are activated by the sympathetic nervous system or dorsal-vagal branches. By chest breathing at rest, this sensation will communicate to our brain that we are in danger and we will probably experience pain.
One of the quickest ways to switch to a parasympathetic state is by elongating your out-breath and making it slower than your in-breath. Other techniques to mobilize your organs below your diaphragm include chants, sighs, and any vocalization that vibrates your belly. This practice offers new sensory signals to an otherwise shutdown or overstimulated nervous system. It is a tool to regulate your nervous system and improve your sensation of safety and pleasure. The brain will then send commands to initiate optimal digestive, sensory, and social functions. You should feel less pain, may hear rumbling sounds in your tummy, and should feel more ready to socialize.
If you feel like unresolved trauma is interfering with the processing of negative thoughts and triggers, I welcome you to seek out a mental health provider, and https://www.psychologytoday.com/us/therapists/trauma-and-ptsd is one potentially useful directory. Working with a compassionate psychotherapist can help you to process trauma while in a safe environment.
Also, if you have neuromusculoskeletal impairments that result from diseases, disorders, conditions, or injuries, and they are interfering with your function and quality of life, then I welcome you to consult with a physical and occupational therapists. If you are experiencing pelvic pain or pelvic floor dysfunction, then please visit https://pelvicpainrehab.com!
I encourage us to play, sing, dance, or go for a walk with someone. We can restoratively surrender to the moment when we meditate, practice tai chi, or yogic breathing. We can teach ourselves to overcome the impulse to fight or run when we sit still and breathe instead. Be present and avoid the tendency to withdraw and dissociate, especially during slow and mindful exercise. “Body-full” movements train us to embody a relaxed state. In this American landscape, I hope that one day we will not judge success by economic growth or wealth, but recognize success by how well an individual can regulate their own nervous system during prosocial behaviors.
References:
Stephen Porges and Deb Dana, Editors. Clinical Applications of the Polyvagal Theory: The Emergence of Polyvagal-Informed Therapies. Norton, 2018.
Rosenberg, Stanley. Accessing the Healing Power of the Vagus Nerve. North Atlantic Books, 2017.
______________________________________________________________________________________________________________________________________
Are you unable to come see us in person? We offer virtual physical and occupational therapy appointments too!
Due to COVID-19, we understand people may prefer to utilize our services from their homes. We also understand that many people do not have access to pelvic floor physical and occupational therapy and we are here to help! The Pelvic Health and Rehabilitation Center is a multi-city company of highly trained and specialized pelvic floor physical and occupational therapistss committed to helping people optimize their pelvic health and eliminate pelvic pain and dysfunction. We are here for you and ready to help, whether it is in-person or online.
Virtual sessions are available with PHRC pelvic floor physical and occupational therapistss via our video platform, Zoom, or via phone. The cost for this service is $85.00 per 30 minutes. For more information and to schedule, please visit our digital healthcare page.
In addition to virtual consultation with our physical and occupational therapistss, we also offer integrative health services with Jandra Mueller, DPT, MS. Jandra is a pelvic floor physical and occupational therapists who also has her Master’s degree in Integrative Health and Nutrition. She offers services such as hormone testing via the DUTCH test, comprehensive stool testing for gastrointestinal health concerns, and integrative health coaching and meal planning. For more information about her services and to schedule, please visit our Integrative Health website page.
PHRC is also offering individualized movement sessions, hosted by Karah Charette, DPT. Karah is a pelvic floor physical and occupational therapists at the Berkeley and San Francisco locations. She is certified in classical mat and reformer Pilates, as well as a registered 200 hour Ashtanga Vinyasa yoga teacher. There are 30 min and 60 min sessions options where you can: (1) Consult on what type of Pilates or yoga class would be appropriate to participate in (2) Review ways to modify poses to fit your individual needs and (3) Create a synthesis of your home exercise program into a movement flow. To schedule a 1-on-1 appointment call us at (510) 922-9836
FAQ
What are pelvic floor muscles?
The pelvic floor muscles are a group of muscles that run from the coccyx to the pubic bone. They are part of the core, helping to support our entire body as well as providing support for the bowel, bladder and uterus. These muscles help us maintain bowel and bladder control and are involved in sexual pleasure and orgasm. The technical name of the pelvic floor muscles is the Levator Ani muscle group. The pudendal nerve, the levator ani nerve, and branches from the S2 – S4 nerve roots innervate the pelvic floor muscles. They are under voluntary and autonomic control, which is a unique feature only they possess compared to other muscle groups.
What is pelvic floor physical and occupational therapy?
Pelvic floor physical and occupational therapy is a specialized area of physical and occupational therapy. Currently, physical and occupational therapistss need advanced post-graduate education to be able to help people with pelvic floor dysfunction because pelvic floor disorders are not yet being taught in standard physical and occupational therapy curricula. The Pelvic Health and Rehabilitation Center provides extensive training for our staff because we recognize the limitations of physical and occupational therapy education in this unique area.
What happens at pelvic floor therapy?
During an evaluation for pelvic floor dysfunction the physical and occupational therapists will take a detailed history. Following the history the physical and occupational therapists will leave the room to allow the patient to change and drape themselves. The physical and occupational therapists will return to the room and using gloved hands will perform an external and internal manual assessment of the pelvic floor and girdle muscles. The physical and occupational therapists will once again leave the room and allow the patient to dress. Following the manual examination there may also be an examination of strength, motor control, and overall biomechanics and neuromuscular control. The physical and occupational therapists will then communicate the findings to the patient and together with their patient they establish an assessment, short term and long term goals and a treatment plan. Typically people with pelvic floor dysfunction are seen one time per week for one hour for varying amounts of time based on the severity and chronicity of the disease. A home exercise program will be established and the physical and occupational therapists will help coordinate other providers on the treatment team. Typically patients are seen for 3 months to a year.
What is pudendal neuralgia and how is it treated?
Pudendal Neuralgia is a clinical diagnosis that means pain in the sensory distribution of the pudendal nerve. The pudendal nerve is a mixed nerve that exits the S2 – S4 sacral nerve roots, we have a right and left pudendal nerve and each side has three main trunks: the dorsal branch, the perineal branch, and the inferior rectal branch. The branches supply sensation to the clitoris/penis, labia/scrotum, perineum, anus, the distal ⅓ of the urethra and rectum, and the vulva and vestibule. The nerve branches also control the pelvic floor muscles. The pudendal nerve follows a tortuous path through the pelvic floor and girdle, leaving it vulnerable to compression and tension injuries at various points along its path.
Pudendal Neuralgia occurs when the nerve is unable to slide, glide and move normally and as a result, people experience pain in some or all of the above-mentioned areas. Pelvic floor physical and occupational therapy plays a crucial role in identifying the mechanical impairments that are affecting the nerve. The physical and occupational therapy treatment plan is designed to restore normal neural function. Patients with pudendal neuralgia require pelvic floor physical and occupational therapy and may also benefit from medical management that includes pharmaceuticals and procedures such as pudendal nerve blocks or botox injections.
What is interstitial cystitis and how is it treated?
Interstitial Cystitis is a clinical diagnosis characterized by irritative bladder symptoms such as urinary urgency, frequency, and hesitancy in the absence of infection. Research has shown the majority of patients who meet the clinical definition have pelvic floor dysfunction and myalgia. Therefore, the American Urologic Association recommends pelvic floor physical and occupational therapy as first-line treatment for Interstitial Cystitis. Patients will benefit from pelvic floor physical and occupational therapy and may also benefit from pharmacologic management or medical procedures such as bladder instillations.
Who is the Pelvic Health and Rehabilitation Team?
The Pelvic Health and Rehabilitation Center was founded by Elizabeth Akincilar and Stephanie Prendergast in 2006, they have been treating people with pelvic floor disorders since 2001. They were trained and mentored by a medical doctor and quickly became experts in treating pelvic floor disorders. They began creating courses and sharing their knowledge around the world. They expanded to 11 locations in the United States and developed a residency style training program for their employees with ongoing weekly mentoring. The physical and occupational therapistss who work at PHRC have undergone more training than the majority of pelvic floor physical and occupational therapistss and as a result offer efficient and high quality care.
How many years of experience do we have?
Stephanie and Liz have 24 years of experience and help each and every team member become an expert in the field through their training and mentoring program.
Why PHRC versus anyone else?
PHRC is unique because of the specific focus on pelvic floor disorders and the leadership at our company. We are constantly lecturing, teaching, and staying ahead of the curve with our connections to medical experts and emerging experts. As a result, we are able to efficiently and effectively help our patients restore their pelvic health.
Do we treat men for pelvic floor therapy?
The Pelvic Health and Rehabilitation Center is unique in that the Cofounders have always treated people of all genders and therefore have trained the team members and staff the same way. Many pelvic floor physical and occupational therapistss focus solely on people with vulvas, this is not the case here.
Do I need pelvic floor therapy forever?
The majority of people with pelvic floor dysfunction will undergo pelvic floor physical and occupational therapy for a set amount of time based on their goals. Every 6 -8 weeks goals will be re-established based on the physical improvements and remaining physical impairments. Most patients will achieve their goals in 3 – 6 months. If there are complicating medical or untreated comorbidities some patients will be in therapy longer.


Comments
Excellent article- makes sense!!
Fantastic information re : breathing slowing on the out breath
This blog is very helpful in explaining a complex integration of the mind-body response i& how this can affect our well-being. Thank you!
Really good synopsis Maryssa!
I love the article and connections made, Th at you Marissa! I come from the approach of sound as a singer and vocal coach and have experienced myself and in my coaching the correctness and inter connectiveness of the polyvagal map and systems with daily exercises and approaches found in singing and teaching breathing, speaking and singing, I hope many people can benefit from this having been put to a ( hopefully) transitory “ stuck” place and situation during Covit19. Beatrice